Intro & Causes - Brain's Early Hiccups
-
Cerebral Palsy (CP): Permanent, non-progressive motor disorders.
-
Affects movement, tone, posture. From insult to developing fetal/infant brain.
-
Incidence: ~2-3/1000 live births. Most common childhood motor disability.
-
Etiology (Brain Insult Timing):
- Prenatal (70-80%):
- Intrauterine infections (TORCH)
- Maternal: thyroid, toxins, trauma
- Congenital malformations
- Multiple gestation
- Perinatal (10%):
- Birth asphyxia (HIE)
- Prematurity (<32 wks, <1500g), IVH, PVL
- Birth trauma
- Postnatal (10%):
- CNS infections (meningitis, encephalitis)
- Head trauma (NAI)
- Kernicterus
- Near-drowning
- Prenatal (70-80%):
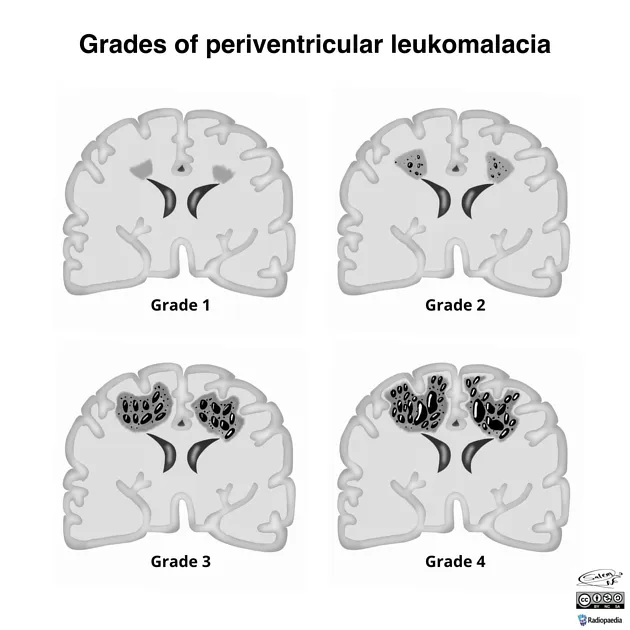
⭐ Periventricular Leukomalacia (PVL) is the most common ischemic brain injury in premature infants leading to CP, particularly spastic diplegia.
CP Types - Movement Mayhem Map
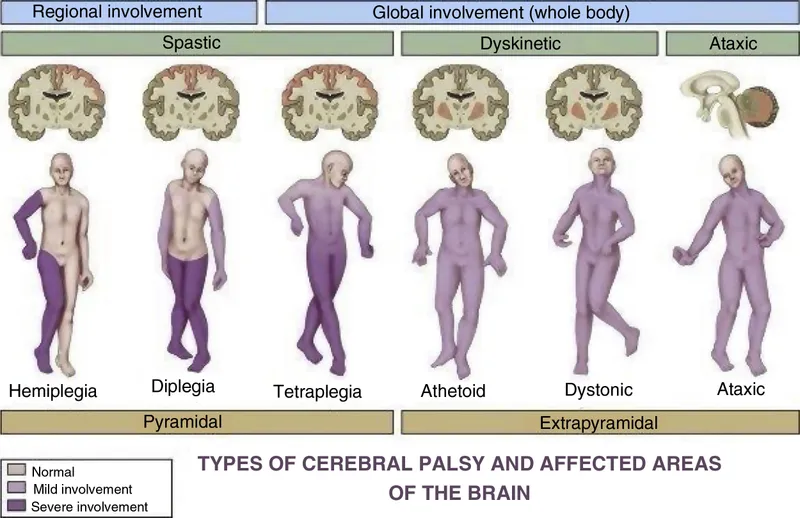
Cerebral Palsy manifests in several primary forms, categorized by movement disorder and affected brain regions. 📌 Mnemonic: Some Days Are Mixed (Spastic, Dyskinetic, Ataxic, Mixed).
| Type | Key Area | Dominant Feature(s) |
|---|---|---|
| Spastic | Pyramidal Tract | ↑ Tone, UMN signs. Subtypes: Hemiplegia, Diplegia (scissor gait), Quadriplegia. |
| Dyskinetic | Basal Ganglia | Involuntary movements: Athetosis (slow, writhing), Chorea (jerky), Dystonia (posturing). |
| Ataxic | Cerebellum | Incoordination, ↓ tone, wide gait, intention tremor. |
| Mixed | Multiple | Combination of above, e.g., spastic-dyskinetic. |
Signs & Dx - Spotting the Signals
- Key Indicators (Red Flags):
- Delayed motor milestones (e.g., no head control by 4 months, not sitting by 9 months).
- Abnormal muscle tone: spasticity (clasp-knife), hypotonia, dystonia, athetosis.
- Persistent primitive reflexes (e.g., Moro, ATNR > 6 months).
- Early asymmetric hand function or preference (< 1 year).
- Feeding/swallowing difficulties.
- Diagnostic Approach:
- Clinical diagnosis: history (perinatal risk factors), neurodevelopmental exam.
- MRI brain: preferred imaging to identify structural lesions (e.g., PVL, HIE changes).
- Standardized assessments: HINE, GMFCS (I-V).
⭐ Asymmetric tonic neck reflex (ATNR) persisting beyond 6 months is a strong predictor of CP.

Treatment & Co-issues - Care & Companions
- Multidisciplinary Team (MDT): CRUCIAL
- Pediatrician, Neurologist, Orthopedician.
- Physio (PT), Occupational (OT), Speech-Language Therapist (SLT).
- Psychologist, Social worker.
- Spasticity Management:
- PT: Stretching, ROM exercises.
- Oral: Baclofen, Diazepam, Tizanidine.
- Focal: Botulinum Toxin A (BoNT-A) injections.
- Severe/Generalized: Intrathecal Baclofen (ITB), Selective Dorsal Rhizotomy (SDR).
- Orthopedic Care:
- Braces, splints, casting.
- Surgery: Contractures, deformities (tendon release, osteotomy).
- Hip surveillance (risk of dislocation).
- Addressing Co-morbidities:
- Epilepsy (~40%): Antiepileptics.
- Pain: Identify source, manage.
- Feeding difficulties/GERD: Nutritional support, G-tube if severe.
- Drooling: Glycopyrrolate, Salivary BoNT-A.
- Sensory: Vision/hearing aids.
- Cognitive/Behavioral: Early intervention, education support.
- Sleep disturbances.
- Family Support & Education: Counseling, respite care.

⭐ Regular hip surveillance (X-ray) is vital in non-ambulant CP children (GMFCS IV-V) to detect hip displacement/subluxation early.
High‑Yield Points - ⚡ Biggest Takeaways
- Cerebral Palsy (CP): non-progressive motor disorder from early brain injury (prenatal/perinatal/postnatal).
- Spastic CP is most common; presents with UMN signs (hypertonia, hyperreflexia).
- Major risk factors: prematurity, low birth weight, birth asphyxia, intrauterine infections.
- Associated co-morbidities: seizures (most common), intellectual disability, visual/hearing issues.
- Diagnosis is clinical; MRI brain confirms structural lesions, rules out progressive disorders.
- Management: multidisciplinary team approach (physio, OT, speech), symptomatic treatment (e.g., baclofen).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

