Intro & Pathophysiology - Leaky Kidney Saga
- Nephrotic Syndrome (NS): Triad/Tetrad:
- Massive Proteinuria: > 40 mg/m²/hr or Urine Protein:Creatinine ratio > 2 mg/mg.
- Hypoalbuminemia: < 3 g/dL.
- Generalized Edema.
- Hyperlipidemia (often present).
- Pathophysiology: "Leaky" Glomerular Filtration Barrier (GFB).
- Podocyte injury (foot process effacement) is key.
- Loss of GFB charge/size selectivity → heavy albuminuria.
- Hypoalbuminemia → ↓ plasma oncotic pressure → edema.
- Hepatic lipoprotein synthesis ↑ → hyperlipidemia.
- Types: Primary (idiopathic, e.g., MCD, FSGS) vs. Secondary (systemic disease, infection, drugs).
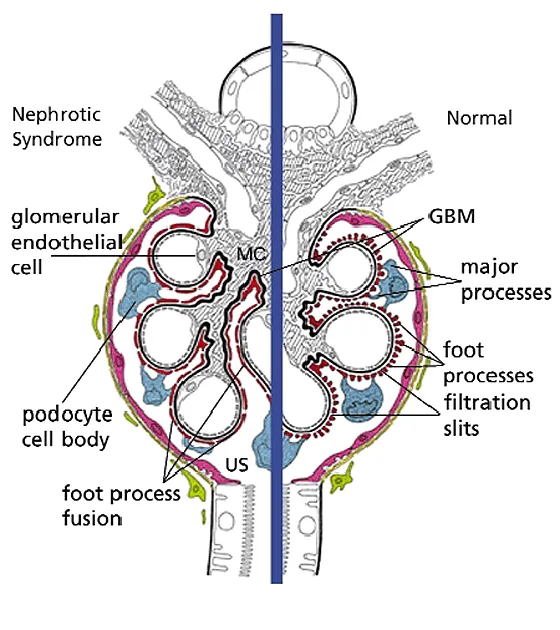
⭐ Minimal Change Disease (MCD) is the most common cause of nephrotic syndrome in children (80-90% of cases).
Clinical Features - Puffy Kid Parade
- Massive Edema: Cardinal sign. Soft, pitting, generalized.
- Initial: Periorbital (esp. morning), facial puffiness.
- Progresses to: Dependent areas (ankles, legs, scrotum/labia), ascites, pleural effusion.
- Frothy Urine: Due to severe proteinuria.
- Systemic: Anorexia, malaise, irritability, abdominal distension/pain.
- BP: Typically normal; occasionally transient hypertension.
- Urine output: May be ↓ (oliguria) during severe edema.
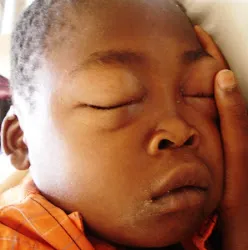
⭐ Periorbital edema, especially prominent in the morning and preceding peripheral edema, is a classic early sign.
Diagnostic Workup - Sleuthing Syndrome Clues
- Renal Biopsy If:
- Age <1 yr or >12 yrs.
- Atypical: Hematuria, HTN, ↓GFR, low C3.
- Steroid-resistant.
⭐ Diagnostic hallmark: Nephrotic-range proteinuria is defined as > 40 mg/m²/hour or a spot urine protein/creatinine ratio > 2-3 mg/mg (or > 200-300 mg/mmol).
Management - Steroid Power Play
- Initial Therapy (First Episode):
- Prednisolone: 2 mg/kg/d (max 60 mg) x 6 wks.
- Then: 1.5 mg/kg alt. days x 6 wks, then taper.
- Key Definitions:
- Remission: Urine alb nil/trace x 3 days.
- Relapse: Urine alb ≥2+ x 3 days.
- FRNS: ≥2 relapses/6mo or ≥4/12mo.
- SDNS: Relapse on taper / within 2 wks post-steroid.
- SRNS: No remission after 8 wks daily prednisolone.
- Relapse:
- Prednisolone 2 mg/kg/d till remission, then 1.5 mg/kg alt. days x 4 wks, taper.
⭐ 80-90% of Minimal Change Disease cases achieve remission with corticosteroids.
Complications & Prognosis - Dodging Danger Zones
- Infections: ⚠️ SBP, cellulitis. Due to ↓IgG.
- Thromboembolism: DVT, PE, RVT. Loss of antithrombin III.
- Hyperlipidemia: ↑ Cholesterol, triglycerides.
- AKI: From hypovolemia.
- Steroid Side Effects: Growth failure, cushingoid.
- Prognosis:
- MCD: Excellent (>90% steroid-sensitive); relapses common.
- FSGS: Guarded (~50% ESRD).
⭐ Patients with nephrotic syndrome are at high risk of infections, especially Spontaneous Bacterial Peritonitis (SBP) caused by encapsulated organisms like Streptococcus pneumoniae.
High‑Yield Points - ⚡ Biggest Takeaways
- Characterized by massive proteinuria (>40 mg/m²/hr or UPC >2), hypoalbuminemia (<2.5 g/dL), generalized edema, and hyperlipidemia.
- Minimal Change Disease (MCD) is the predominant cause in children (>80%), typically idiopathic.
- Majority of MCD cases are steroid-sensitive, showing good response to initial corticosteroid therapy.
- Major complications include serious infections (especially Spontaneous Bacterial Peritonitis due to S. pneumoniae) and thromboembolic events.
- Renal biopsy is usually reserved for atypical features (e.g., age <1 year or >12 years, persistent hypertension, gross hematuria) or steroid resistance.
- Look for frothy urine and periorbital edema as classic early presenting signs in children.
- Management focuses on inducing remission with steroids, managing edema, and preventing complications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

