CKD Basics - Tiny Kidneys, Big Trouble
- Definition: Kidney damage OR GFR < 60 mL/min/1.73m² for ≥ 3 months.
- Pediatric Focus:
- CAKUT (Congenital Anomalies of Kidney and Urinary Tract) is the primary cause.
- Growth failure & hypertension are key complications.
- KDOQI Staging (GFR in mL/min/1.73m²):
- Stage 1: GFR ≥ 90 (with kidney damage)
- Stage 2: GFR 60-89 (mild ↓)
- Stage 3: GFR 30-59 (moderate ↓)
- Stage 4: GFR 15-29 (severe ↓)
- Stage 5: GFR < 15 or dialysis (kidney failure)
⭐ The most common method for eGFR estimation in children is the Schwartz formula, which relates eGFR to height and serum creatinine.
-
Formula: $eGFR = k \times \frac{Height (cm)}{Serum Creatinine (mg/dL)}$.
-
Early Clues: Often subtle; e.g., polyuria, enuresis, poor growth.
CKD Causes - The Usual Suspects

- CAKUT (Congenital Anomalies of Kidney & Urinary Tract): Most common (~50% of peds CKD)
- Renal dysplasia/hypoplasia
- Obstructive uropathy (e.g., PUV, UPJ obstruction)
- Reflux nephropathy (VUR)
- Glomerulonephritis (GN): Significant group (~15-20%)
- FSGS (common in SRNS)
- Chronic GN (e.g., IgA nephropathy, MPGN)
- Systemic: Lupus nephritis, HSP nephritis
- Hereditary Nephropathies: Genetically determined (~10-15%)
- Alport syndrome (COL4A defect)
- ARPKD (Autosomal Recessive Polycystic Kidney Disease)
- Nephronophthisis
- Cystinosis
- Other Causes: Diverse; includes:
- HUS (Thrombotic microangiopathy)
- Renal vascular (e.g., RVT, RAS)
- Severe AKI sequelae (e.g., cortical necrosis)
⭐ Congenital Anomalies of the Kidney and Urinary Tract (CAKUT) are the leading cause of pediatric CKD and ESRD in most countries.
CKD Signs & Symptoms - Spotting the Signals
- Presentation often insidious; non-specific in early stages.
- Early Clues:
- Growth failure: frequently the first indicator.
- Anorexia, nausea, vomiting.
- Polyuria, nocturia, secondary enuresis (impaired concentrating ability).
- Pallor (anemia from ↓ erythropoietin).
- Unexplained fatigue, lethargy.
- As GFR Declines:
- Hypertension.
- Edema (peripheral, periorbital).
- Bone pain, deformities (renal osteodystrophy, rickets).
- Pruritus.
- Neurological: headache, poor concentration, seizures (uremic encephalopathy).
- Electrolyte imbalances (e.g., hyperkalemia, acidosis).
⭐ Growth failure is often the earliest and most prominent clinical manifestation of CKD in children, significantly impacting quality of life.
CKD Management - The Balancing Act
- Core Goals: Delay progression, manage complications, prepare for Renal Replacement Therapy (RRT).
- Key Interventions (The Balance):
- Blood Pressure: Target <90th percentile or <130/80 mmHg. ACEi/ARBs often used.
- Anemia: Iron, Erythropoiesis-Stimulating Agents (ESAs). Target Hb 10-12 g/dL.
- CKD-MBD: Phosphate binders, Vitamin D sterols. Control P, Ca, PTH.
- Growth: Recombinant human Growth Hormone (rhGH) if GFR <50 ml/min/1.73m².
- Acidosis: Oral alkali (e.g., NaHCO₃). Target serum bicarbonate >22 mEq/L.
- Nutrition: Adequate calories; protein, Na⁺, K⁺, P, fluid restriction as per stage.
- Immunizations: Crucial; follow specific schedules.
- Renal Replacement Therapy (RRT):
- Dialysis: Peritoneal (PD) often preferred in younger children; Hemodialysis (HD).
- Transplantation: Optimal long-term solution.
⭐ Kidney transplantation offers the best long-term outcome and quality of life for children with ESRD, improving growth and neurocognitive development.
High‑Yield Points - ⚡ Biggest Takeaways
- CAKUT (Congenital Anomalies of Kidney and Urinary Tract) is the leading cause of pediatric CKD.
- Growth failure is a cardinal sign, requiring prompt intervention.
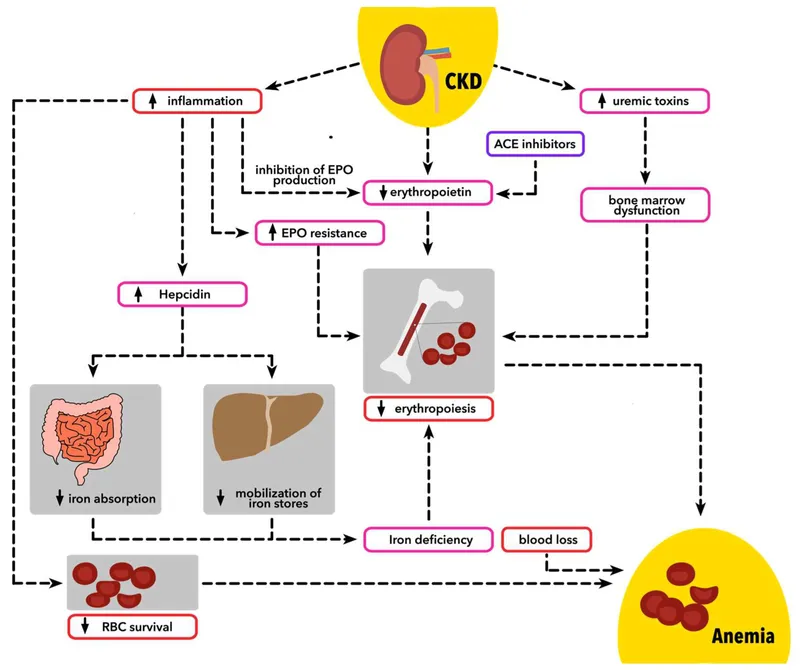
- Anemia (due to ↓ erythropoietin) is frequent and significant.
- CKD-MBD causes renal osteodystrophy, affecting growth and bone integrity.
- Hypertension is common, accelerates CKD progression and cardiovascular risk.
- Estimate GFR in children using the height-based Schwartz formula.
- Proteinuria is a key marker of kidney damage and predicts progression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

