RDS Intro - Lungs Gasping
- Definition: Acute lung disease of premature infants, causing respiratory distress shortly after birth.
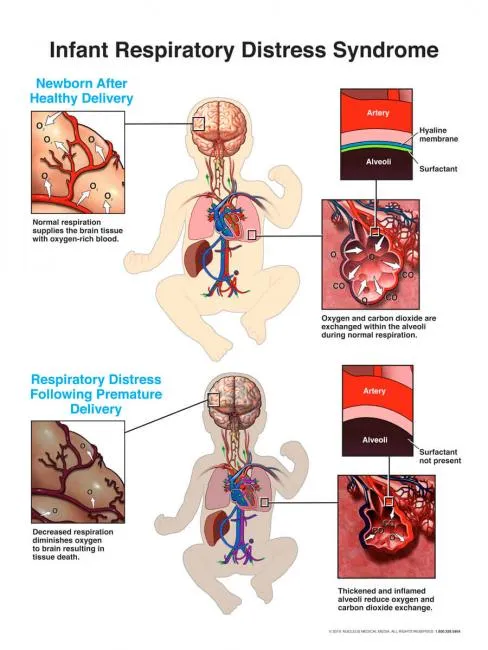
- Core Defect: Insufficient pulmonary surfactant production and secretion by Type II pneumocytes.
- Pathophysiology:
- Surfactant ↓ → Alveolar surface tension ↑ → Diffuse alveolar atelectasis.
- Consequences: ↓ Lung compliance (stiff lungs), ↑ Work of breathing.
- Gas Exchange: Ventilation-Perfusion (V/Q) mismatch → Hypoxemia, Hypercarbia, Respiratory acidosis.
⭐ RDS is also known as Hyaline Membrane Disease due to the characteristic eosinophilic membranes (fibrin, cellular debris) lining alveoli seen on histology.
RDS Risks - Danger Signals
- Major Risk Factors (↑ RDS Incidence/Severity):
- Prematurity: Greatest risk, esp. < 34 weeks, severe < 28 weeks.
- Maternal Diabetes: Impairs surfactant production.
- Cesarean Section: Particularly elective, without labor.
- Male Gender: Slower lung maturation.
- Perinatal Asphyxia: Damages type II pneumocytes.
- Family History/Genetics: Previous sibling with RDS.
- Mitigating Factors (↓ RDS Risk):
- Antenatal Corticosteroids: Stimulate surfactant synthesis.
- Chronic Intrauterine Stress: (e.g., PIH, IUGR, PROM) accelerates lung maturity.
- Female Gender.
⭐ Maternal diabetes increases fetal insulin, which antagonizes cortisol and inhibits surfactant synthesis, significantly ↑ RDS risk.
RDS Signs & Dx - Spotting Trouble
- Clinical Manifestations (Onset: birth to hours):
- Tachypnea (respiratory rate >60/min)
- Expiratory grunting (to maintain Functional Residual Capacity - FRC)
- Nasal flaring, intercostal & subcostal retractions
- Cyanosis (central, often requiring supplemental O₂)
- Auscultation: Decreased air entry, fine end-inspiratory crackles
- Diagnostic Evaluation:
- Arterial Blood Gas (ABG): Hypoxemia ($P_aO_2$ < 50 mmHg in room air), hypercarbia ($P_aCO_2$ > 65 mmHg), respiratory or mixed acidosis.
- Chest X-ray (CXR): Key for diagnosis & severity.
- Bilateral, diffuse reticulogranular ("ground-glass") opacities
- Prominent air bronchograms (dark, air-filled bronchi against opaque alveoli)
- Low lung volumes / bell-shaped thorax
⭐ Chest X-ray showing a "white-out" appearance in severe RDS indicates extensive atelectasis and poor prognosis.
RDS Management - Breathing Easy
- Goal: Adequate oxygenation & ventilation, minimize lung injury.
- Supportive Care:
- Thermoregulation: Maintain neutral thermal environment.
- Fluid & Nutrition: IV fluids, early parenteral/enteral nutrition.
- Monitor: Vitals, blood gas, electrolytes.
- Respiratory Support:
- Nasal CPAP (nCPAP): Preferred initial mode if spontaneous breathing.
- Surfactant Replacement: Via endotracheal tube. Consider early rescue.
- 📌 INSURE (Intubate-Surfactant-Extubate).
- Mechanical Ventilation: If CPAP fails or apnea. Gentle ventilation strategies.
⭐ Antenatal corticosteroids (e.g., Betamethasone 2 doses 12mg IM 24h apart) significantly reduce RDS incidence and severity when given between 24-34 weeks gestation.
RDS Complications - Future Watch
- Acute Risks:
- Air Leaks: Pneumothorax, Pulmonary Interstitial Emphysema (PIE).
- Hemorrhage: Intraventricular (IVH), pulmonary.
- Infection: Nosocomial sepsis.
- Cardiovascular: Patent Ductus Arteriosus (PDA), hypotension.
- Long-term Outlook (Future Watch):
-
⭐ Bronchopulmonary Dysplasia (BPD) is a major long-term complication, defined as oxygen dependency at 36 weeks postmenstrual age.
- Retinopathy of Prematurity (ROP): Risk with prolonged O₂ therapy.
- Neurodevelopmental Impairment (NDI): Includes cerebral palsy, significant cognitive, motor, or sensory deficits.
- Chronic Respiratory Morbidity: Increased risk of asthma, recurrent wheezing, and respiratory infections.
-
High-Yield Points - ⚡ Biggest Takeaways
- RDS arises from surfactant deficiency in preterm infants, leading to progressive atelectasis.
- CXR hallmark: Diffuse bilateral reticulogranular ("ground-glass") pattern and air bronchograms.
- Clinical onset soon after birth: tachypnea, audible grunting, significant retractions, nasal flaring, cyanosis.
- Prevention: Antenatal corticosteroids administered to mothers at risk of premature delivery.
- Management: Intratracheal exogenous surfactant and respiratory support (CPAP or mechanical ventilation).
- Monitor for common complications: PDA, Bronchopulmonary Dysplasia (BPD), IVH, ROP.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


