Initial Assessment & Golden Minute - Golden Minute Moves
At Birth: Rapid Assessment
- Term gestation?
- Good muscle tone?
- Breathing or crying?
If NO to any $\rightarrow$ Proceed to Golden Minute interventions.
Golden Minute (First 60 seconds): Key actions to establish effective ventilation:
- Warm: Place under radiant warmer, prevent heat loss.
- Dry: Thoroughly dry infant, remove wet linens.
- Stimulate: Gently rub back or flick soles.
- Position Airway: Slight neck extension ("sniffing" position).
- Suction (If Obvious Obstruction): Mouth first, then nose (📌 M before N).
Assess response: Respirations and Heart Rate (HR).
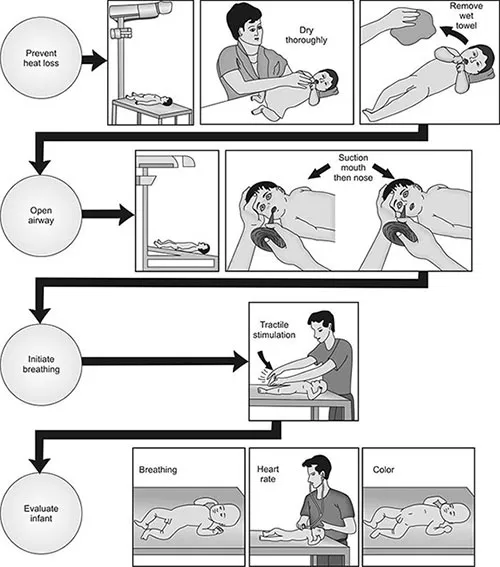
⭐ The most crucial initial steps are ensuring the baby is warm, the airway is clear, and stimulating the baby to breathe. Most neonates respond to these measures alone within the first 60 seconds.
If HR < 100 bpm or apnea/gasping persists after initial steps $\rightarrow$ Start Positive Pressure Ventilation (PPV).
Positive Pressure Ventilation - Pump Up The Lungs
- Indications: Apnea/gasping, or Heart Rate (HR) < 100 bpm despite initial steps.
- Technique:
- Rate: 40-60 breaths/min ("squeeze-release-release").
- Pressure: Initial 20-25 cm H₂O (term), 20 cm H₂O (preterm).
- FiO₂: Term (≥35 wks): 21% (Room Air). Preterm (<35 wks): 21-30%. Titrate to SpO₂ targets.
- Check for Efficacy: Chest rise, HR ↑, SpO₂ ↑.
- Troubleshooting (If no improvement): 📌 MRSOPA
- Mask adjustment
- Reposition airway
- Suction mouth then nose
- Open mouth
- Pressure increase (max 30-40 cm H₂O)
- Alternative airway (ETT/LMA)
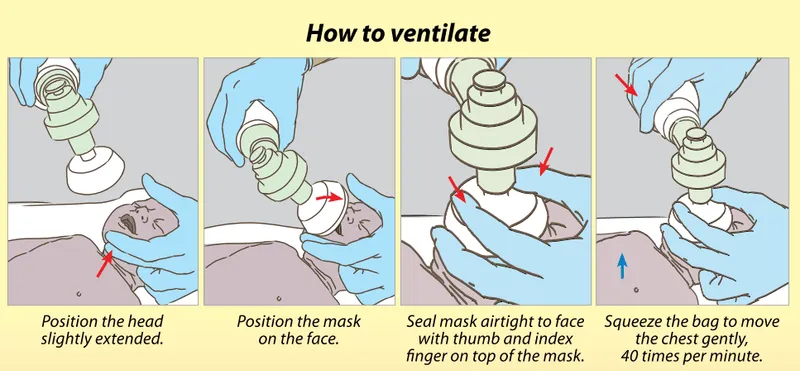
⭐ Effective ventilation is the single most important and effective step in neonatal resuscitation; most neonates respond to PPV alone.
Chest Compressions & Advanced Airway - Heartbeat Heroes
- CC Indication: HR < 60/min despite 30s effective PPV.
- CC Technique: 2-thumb, lower ⅓ sternum, depth ⅓ AP. Rate: 90/min.
- CC:V Ratio: 3:1 (Total 120 events/min). 📌 "One-Two-Three-Breathe".
- Advanced Airway (ETT/LMA): If BMV ineffective, prolonged PPV, surfactant.
- ETT (mm): <1kg: 2.5; 1-2kg: 3.0; >2kg: 3.5. Confirm: EtCO2.
- Epinephrine: If HR < 60/min after 60s CC+PPV.
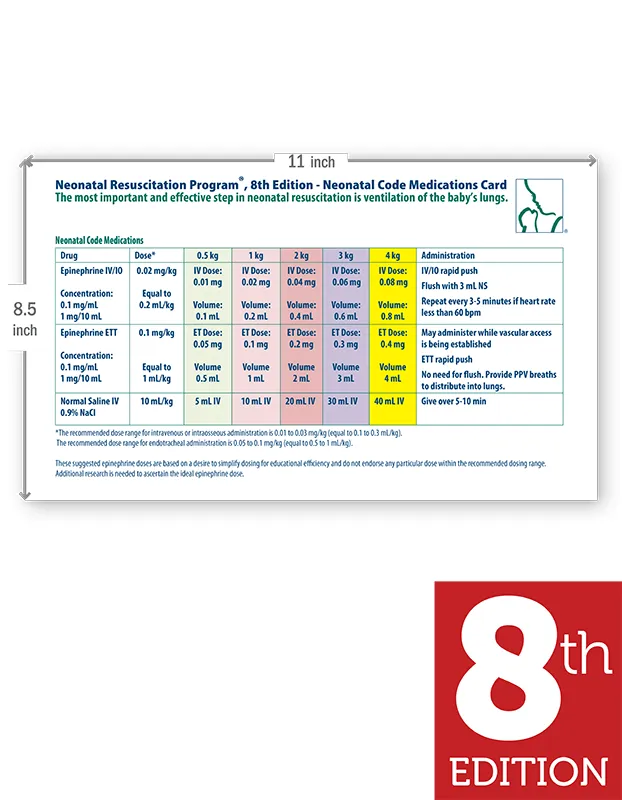
- Dose (1:10,000): IV/IO: 0.01-0.03 mg/kg. ETT: 0.05-0.1 mg/kg.
- Repeat q 3-5 min.
- Reassess HR: q 60s.

⭐ IV/IO Epinephrine is preferred over ETT for neonatal resuscitation due to reliable absorption.
Medications & Special Considerations - Potions & Precautions
- Epinephrine: HR < 60/min despite adequate ventilation & compressions.
- IV/IO (preferred): 0.01-0.03 mg/kg (1:10,000).
- ET: 0.05-0.1 mg/kg (1:10,000).
- Volume (NS/RL): Hypovolemia.
- Dose: 10 mL/kg IV/IO over 5-10 min.
- Naloxone: Maternal opioids (<4h); ensure PPV.
- Dose: 0.1 mg/kg. ⚠️ Avoid if maternal opioid dependence (seizure risk).
- Glucose (D10W): Hypoglycemia.
- Dose: 2 mL/kg IV (0.2 g/kg).
- Special Conditions:
- Preterm: Thermoregulation (↑room temp 23-25°C), gentle PPV, CPAP/surfactant.
- CDH: Intubate immediately, NG/OG tube; avoid BMV.
⭐ Non-vigorous MSAF: Suction mouth/nose. Routine intubation/tracheal suction NO longer advised.
High‑Yield Points - ⚡ Biggest Takeaways
- Golden Minute: Initial steps (warm, dry, stimulate, position, clear secretions) within 60 seconds.
- PPV if HR <100 bpm, apnea, or gasping.
- Chest compressions if HR <60 bpm after 30s effective PPV; 3:1 ratio.
- Epinephrine if HR <60 bpm despite effective PPV & compressions.
- Target pre-ductal SpO2: 1 min (60-65%), 5 min (80-85%), 10 min (85-95%).
- MSAF: Vigorous infants - no routine intubation; suction if obstructing.
- Delayed cord clamping (30-60s) for vigorous infants.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

