IVH Basics - Preemie Brain Bleeds 101
- Definition: Bleeding in brain ventricles, from germinal matrix.
- Incidence: Mainly in preemies; risk ↑ with ↓ GA & BW.
- Key Risk Factors:
- Prematurity (esp. <32 weeks GA)
- Low birth weight (esp. <1500g BW)
- Respiratory Distress Syndrome (RDS)
- Perinatal asphyxia
- Rapid bicarbonate infusion
⭐ IVH is most common in premature infants, especially those <32 weeks gestation or <1500g BW.
Pathophysiology & Origin - Why Fragile Vessels Weep
- Germinal Matrix (GM):
- Location: Highly vascular region, subependymal, adjacent to lateral ventricles.
- Vessels: Fragile capillaries with minimal structural support (poor pericyte, collagen, and glial support).
- Involution: Begins around 28-32 weeks gestation; largely regresses by term.
- Pathogenesis Triggers:
- Fluctuations in Cerebral Blood Flow (CBF): Common in premature infants (e.g., due to RDS, PDA, sepsis).
- Hypoxia-ischemia-reperfusion injury: Damages vulnerable GM endothelium.
- Impaired cerebral autoregulation: Inability to maintain stable CBF despite systemic blood pressure changes.
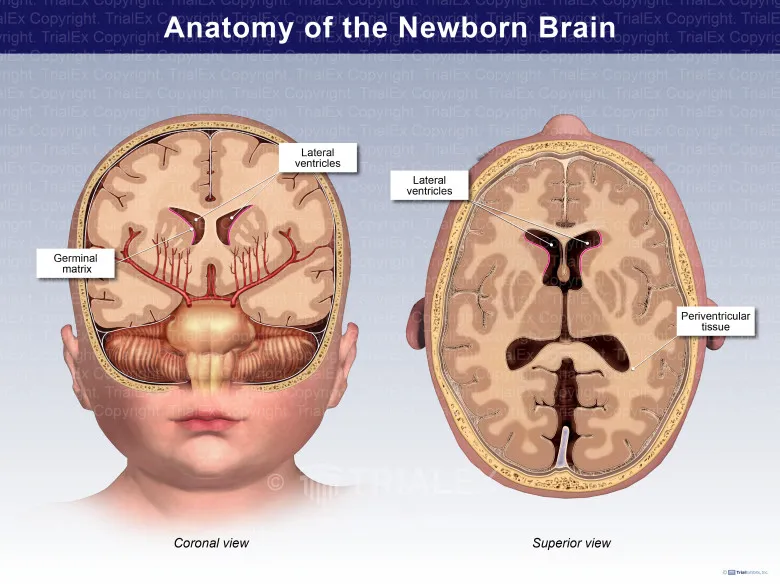
⭐ The subependymal germinal matrix is the primary site of IVH origin due to its rich but fragile capillary network, particularly vulnerable before 32 weeks gestation.
Grading the Bleed - Papile's IVH Scorecard
The Papile Classification grades Intraventricular Hemorrhage (IVH) severity in preterm infants via cranial ultrasound, impacting prognosis and management.
| Grade | Description |
|---|---|
| I | Germinal Matrix Hemorrhage (GMH) only; bleed confined to subependymal region. |
| II | IVH without ventricular dilatation; blood enters ventricles, normal size. |
| III | IVH with ventricular dilatation; ventricles enlarged by blood. |
| IV | IVH with intraparenchymal hemorrhage (PVHI); bleed extends into brain tissue. |
⭐ Grade IV IVH, with parenchymal involvement (echodensity), has the worst prognosis and highest risk of neurodevelopmental impairment.
Signs & Screening - Catching the Crimson Tide
- Clinical Features:
- Often silent.
- Subtle: Apnea, bradycardia, ↓LOC, hypotonia, bulging fontanelle.
- Catastrophic: Collapse, coma, decerebrate, fixed pupils.
- Screening: Cranial Ultrasound (CUS) is key.
⭐ Approx. 90% of IVH occurs within the first 72 hours of life, 50% on day 1.
Management & Prevention - Brain-Saving Strategies
- Prevention Strategies:
- Antenatal corticosteroids (for mothers at risk of preterm delivery).
- Delayed cord clamping.
- Optimal perinatal care: Gentle handling, avoid birth asphyxia, maintain stable BP/perfusion.
- Management Approach:
- Supportive care: Maintain physiological stability (ventilation, BP, glucose, electrolytes, acid-base balance).
- Serial Cranial Ultrasound (CUS) monitoring.
- Manage complications: E.g., post-hemorrhagic hydrocephalus (PHH) with lumbar punctures, VP shunt.
- Avoid rapid infusions.
⭐ Antenatal corticosteroids administered to the mother are the most effective intervention for preventing IVH in preterm infants.
Outcomes & Outlook - The Aftermath & Ahead
- Complications: Post-Hemorrhagic Hydrocephalus (PHH), periventricular hemorrhagic infarction (PVHI - Grade IV), cystic Periventricular Leukomalacia (PVL), seizures, cerebral palsy, developmental delay.
- Prognosis: Grade-dependent. Grade I/II generally good; Grade III/IV ↑risk mortality & neurodevelopmental impairment.
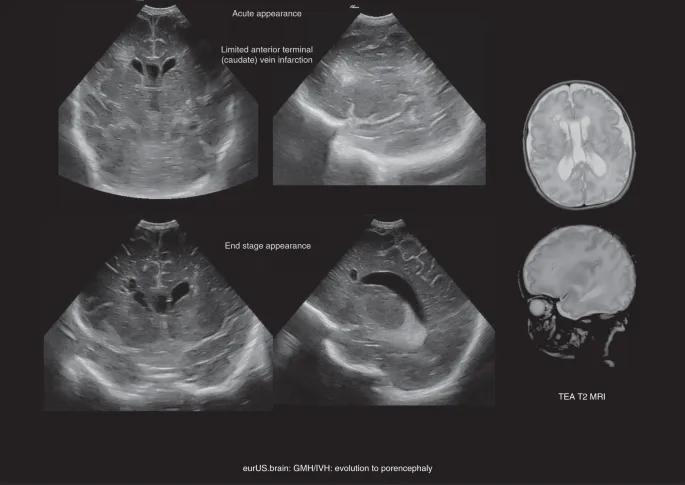
⭐ Post-hemorrhagic hydrocephalus (PHH) is a common complication of severe IVH, often requiring neurosurgical intervention.
High-Yield Points - ⚡ Biggest Takeaways
- Primarily affects preterm infants, especially < 32 weeks gestation and < 1500g birth weight.
- Bleeding originates from the fragile germinal matrix capillaries, usually within the first 72 hours of life.
- Cranial ultrasound is the gold standard for diagnosis, using Papile grading (I-IV) for severity.
- Grade I is subependymal hemorrhage; Grade II involves intraventricular extension without dilatation.
- Grade III shows ventricular dilatation; Grade IV indicates intraparenchymal involvement.
- Key complications include post-hemorrhagic hydrocephalus, periventricular leukomalacia (PVL), and neurodevelopmental delay.
- Antenatal corticosteroids significantly reduce incidence and severity in preterm births.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

