Congenital Anomalies: General Principles - Tiny Troublemakers
- Structural/functional defects at birth; major cause of infant mortality.
- Classification:
- Malformation: Intrinsic error in morphogenesis (e.g., cleft palate).
- Deformation: Extrinsic mechanical forces (e.g., positional talipes).
- Disruption: Breakdown of normal tissue (e.g., amniotic bands).
- Dysplasia: Abnormal cell organization in tissue (e.g., skeletal dysplasias).
- Sequence: Anomalies from single defect (e.g., Potter sequence).
- Syndrome: Multiple anomalies, common cause (e.g., Down syndrome).
- Teratogens: Agents causing birth defects.
- Critical period: Organogenesis (3-8 weeks).
- 📌 TORCH (Toxo, Other, Rubella, CMV, Herpes).
- Drugs: Thalidomide, Valproate (NTDs), Warfarin, ACEi.
- Maternal: Diabetes (caudal regression, VSD), PKU.
- Prevention: Folic acid (0.4 mg/day).
⭐ The most common major congenital anomaly is congenital heart disease.
Congenital Anomalies: CNS - Brainy Birth Bumps
- Neural Tube Defects (NTDs)
- Prevention: Folic acid (0.4 mg/day; 4 mg/day high risk).
- Dx: ↑AFP, ↑Amniotic AChE.
- Types:
Type Key Feature Anencephaly Absent brain/skull; "frog-like" Encephalocele Brain/meninges herniation via skull Spina Bifida Occulta Vertebral defect, hair tuft Spina Bifida Cystica Meningocele, Myelomeningocele (+neural tissue)
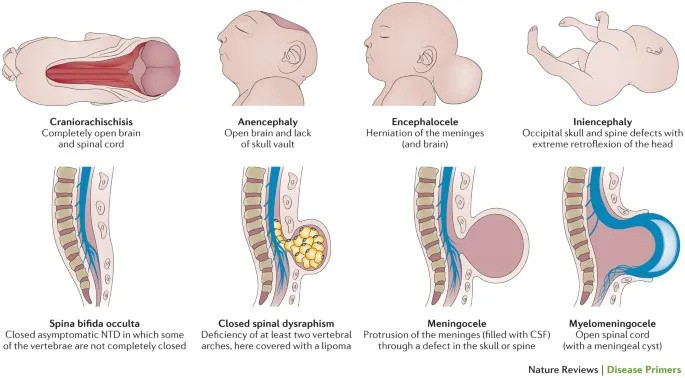
- Hydrocephalus: ↑CSF; Signs: ↑HC, bulging fontanelle, sunset eyes.
- Types: Communicating (↓absorption), Non-communicating (obstruction, e.g., aqueductal stenosis).
- Holoprosencephaly: Forebrain cleavage failure. Facial anomalies. Trisomy 13.
- Dandy-Walker Malformation: 4th vent. cystic dilation, cerebellar vermis agenesis.
- Arnold-Chiari Malformation Type II: Cerebellar, brainstem herniation.
⭐ Arnold-Chiari Type II: strong assoc. with myelomeningocele.
- Microcephaly: HC < -2 SD. Causes: TORCH, genetic, FAS.
- Lissencephaly: Smooth brain (agyria). Severe neuro deficit.
Congenital Anomalies: CVS - Heart's Hiccups
- CHD Types:
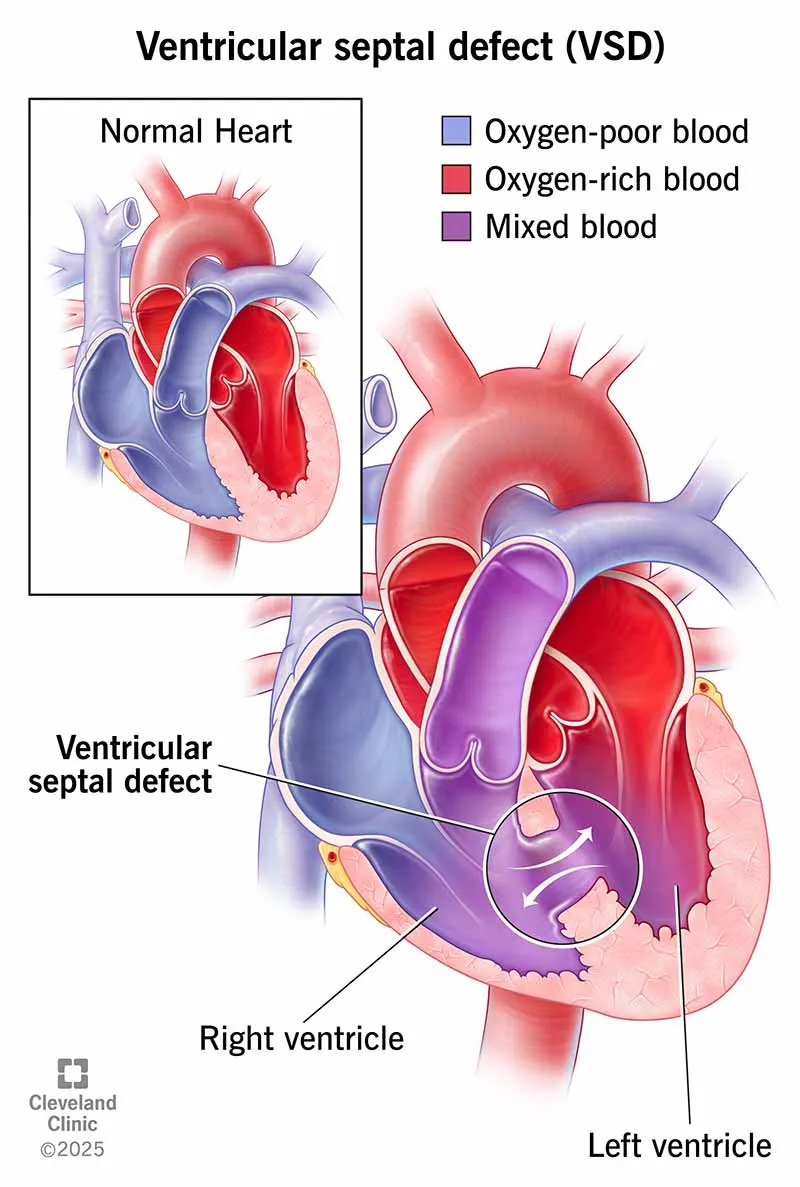
Shunt Type Examples Clinical Clues O2 Test (PaO2) Acyanotic (L→R) VSD, ASD, PDA CHF, ↑Pulm. flow Responds Cyanotic (R→L) TOF, TGA Cyanosis, ↓Syst. O2 No response - VSD (Ventricular Septal Defect): Most common CHD. Harsh pansystolic murmur (L lower sternal border).
- ASD (Atrial Septal Defect): Wide, fixed split S2. Ostium secundum commonest.
- PDA (Patent Ductus Arteriosus): Continuous machinery murmur (L infraclavicular). Close: Indomethacin. Open: Prostaglandin E1 (PGE1) (0.05-0.1 mcg/kg/min).
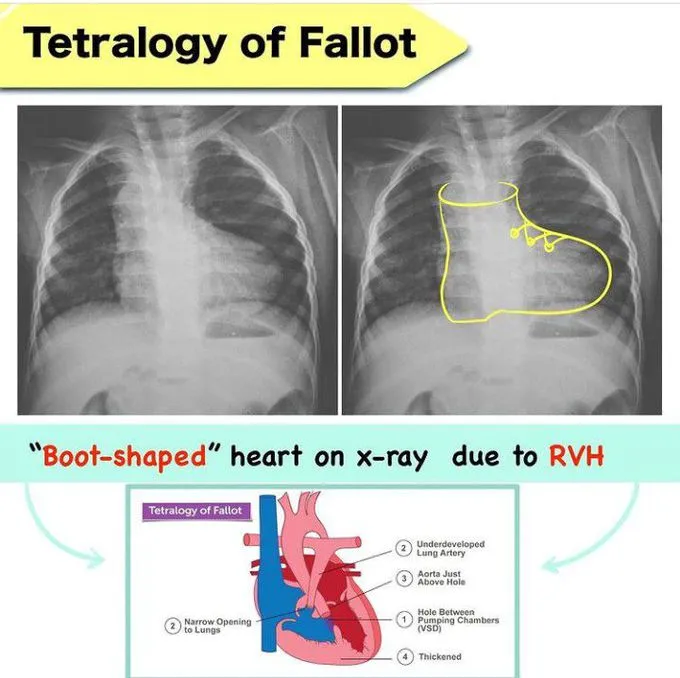
- TOF (Tetralogy of Fallot): 📌 PROVe (Pulmonary Stenosis, RVH, Overriding aorta, VSD). Boot-shaped heart (CXR). Tet spells (knee-chest position).
- TGA (Transposition of Great Arteries): Severe cyanosis at birth. "Egg-on-string" (CXR). PGE1 vital for mixing.
⭐ VSD is the most common congenital heart defect; Bicuspid Aortic Valve is the most common congenital cardiovascular malformation overall.
Congenital Anomalies: GIT & Abdomen - Gut Gaffes & Outies
-
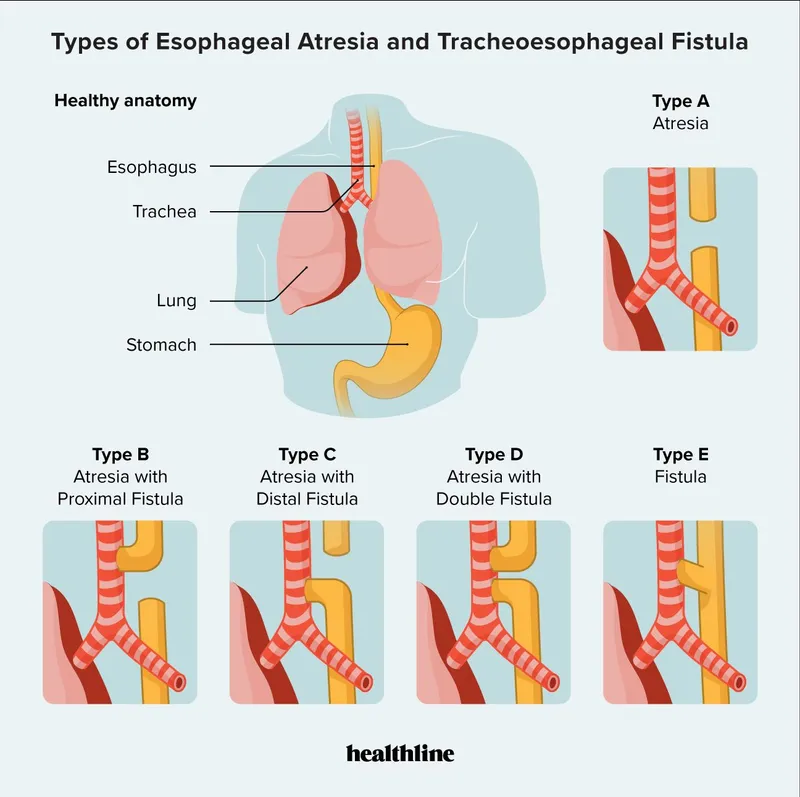
Tracheoesophageal Fistula (TEF) & Esophageal Atresia (EA):
- Most common: Type C (EA + distal TEF, 85%). Polyhydramnios.
- 📌 VACTERL: Vertebral, Anal, Cardiac, TEF, Renal, Limb.
- Dx: NG tube coils in esophageal pouch.
-
Duodenal Atresia:
- "Double bubble" sign on X-ray. Bilious vomiting.
- Associated with Down syndrome (30%).
-
Malrotation with Volvulus:
- Bilious vomiting in neonate = surgical emergency!
- "Corkscrew" sign on upper GI contrast study.
-
Omphalocele vs. Gastroschisis:
Feature Omphalocele Gastroschisis Sac Present (amnion, peritoneum) Absent Location Midline, umbilical cord inserts into sac Right of umbilicus, cord insertion normal Bowel Usually normal Edematous, matted, inflamed Liver in sac Common Rare Associated anom. Common (50-70%, cardiac, chromosomal) Less common (10-15%, e.g., gut atresia) Maternal AFP ↑ ↑↑ 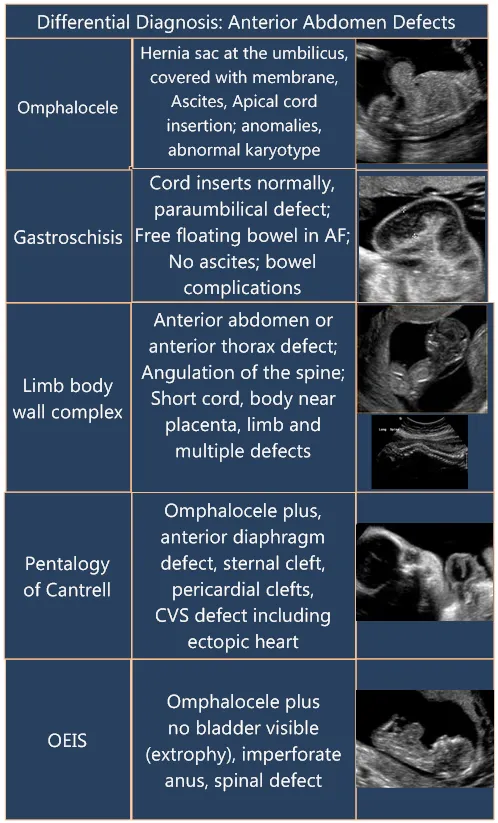
⭐ Gastroschisis: No sac means bowel is exposed to amniotic fluid, leading to chemical peritonitis; often an isolated defect compared to omphalocele which has higher rates of associated anomalies.
High‑Yield Points - ⚡ Biggest Takeaways
- Neural Tube Defects: Folic acid prevents; anencephaly & spina bifida are key types.
- Congenital Heart Defects: Most common; VSD most frequent. Differentiate cyanotic (e.g., TOF) vs. acyanotic (e.g., ASD).
- Down Syndrome (Trisomy 21): Linked to duodenal atresia ("double bubble") and AV canal defects.
- Diaphragmatic Hernia: Usually left-sided (Bochdalek), causes severe pulmonary hypoplasia.
- Esophageal Atresia/TEF: Polyhydramnios, choking with feeds; Type C (distal TEF) is most common.
- Gastroschisis vs. Omphalocele: Gastroschisis (no sac, bowel exposed); Omphalocele (sac present, other anomalies common).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more