Pediatric HIV - Tiny Targets, Big Battle
- Epidemiology (India): Primarily vertical transmission (mother-to-child).
- Accounts for >90% of pediatric cases.
- Risk: 15-45% without intervention; <1-2% with effective ART.
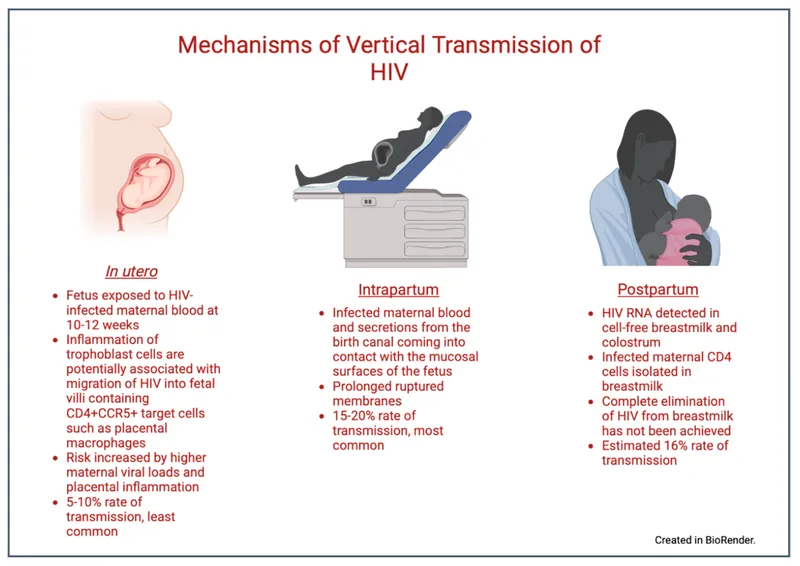
- Transmission Routes:
- Intrauterine (in utero)
- Intrapartum (during delivery)
- Postpartum (breastfeeding)
- Diagnosis:
- Infants <18 months: HIV DNA/RNA PCR (antibody tests unreliable due to maternal Ab).
- Two positive virological tests confirm infection.
- Children >18 months: ELISA/Rapid antibody tests, confirmed by Western Blot (like adults).
- Infants <18 months: HIV DNA/RNA PCR (antibody tests unreliable due to maternal Ab).
⭐ Early diagnosis is critical: Virological testing (HIV DNA PCR) should be done at 4-6 weeks of age for exposed infants.
- Clinical Staging: WHO clinical staging (1-4) adapted for children.
- Prevention of Parent-to-Child Transmission (PPTCT): Key strategy.
- Antiretroviral therapy (ART) for mother & infant.
- Safe delivery practices.
- Safe infant feeding counseling (exclusive breastfeeding with maternal ART or exclusive replacement feeding).
Diagnosis in Kids - Spotting the Shadow
- Age dictates test choice:
- <18 months: Maternal IgG Ab interferes. Use Virological tests.
- >18 months: HIV Antibody tests (similar to adults).
- Virological Tests (Infants <18m):
- HIV DNA PCR: Detects proviral DNA. Preferred.
- HIV RNA PCR (Viral Load): Detects viral RNA.
- Timing: Birth (high-risk), 14-21 days, 1-2 months, 4-6 months.
- Antibody Tests (Children >18m):
- Screening: ELISA / Rapid tests.
- Confirmatory: Western Blot / IFA.
- Maternal Ab usually wanes by 12-18 months.
- Presumptive Diagnosis:
- Symptomatic infant <18 months + 1 positive virological test → early ART.
- Definitive Exclusion (non-breastfed):
- Two negative virological tests (one at ≥1 month, one at ≥4 months).
- OR Negative Ab test at ≥18 months.
- Breastfed infants: Test 6 weeks after breastfeeding cessation.
⭐ For infants <18 months, two positive virological assays (HIV DNA PCR or RNA PCR) on separate blood samples are required for definitive HIV diagnosis.
Clinical Picture & Staging - Symptoms & Signals
- Common Presentations:
- Failure to thrive (FTT), Persistent Generalized Lymphadenopathy (PGL), Hepatosplenomegaly (HSM)
- Recurrent infections (e.g., otitis media, pneumonia, oral thrush)
- Developmental delay
- WHO Clinical Staging (Key Features):
- Stage 1: Asymptomatic, PGL.
- Stage 2: Moderate unexplained malnutrition, recurrent URTIs, popular pruritic eruptions, angular cheilitis.
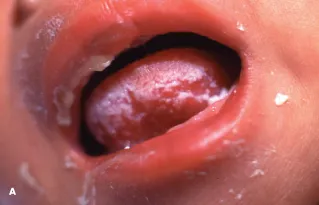
⭐ Persistent oral thrush (post-neonatal) is a key WHO Stage 2/3 indicator.
- Stage 3: Severe unexplained malnutrition, chronic diarrhea/fever (>1mo), persistent oral candidiasis, pulmonary TB, severe bacterial infections.
- Stage 4: HIV wasting syndrome, Pneumocystis jirovecii pneumonia (PJP), esophageal candidiasis, extrapulmonary TB, Kaposi sarcoma, HIV encephalopathy.
- Severe Immunodeficiency (CD4 Thresholds for initiating ART regardless of clinical stage):
- <12 months: <750 cells/mm³ or <15%
- 12-35 months: <500 cells/mm³ or <15%
- 36-59 months: <350 cells/mm³ or <15%
- ≥5 years: <200 cells/mm³ or <15%
ART & Prevention Power-Up - Fighting Back & Future Proofing
- ART Initiation: Treat ALL HIV-infected children immediately, irrespective of CD4/clinical stage.
- ART Goals: Suppress VL, ↑CD4, ↓morbidity/mortality.
- Infants/Young Children (<3yrs or <10kg): ABC + 3TC + LPV/r (or DTG).
- Older Children (≥3yrs & ≥10kg): ABC + 3TC + DTG (or EFV).
- Adolescents (≥10yrs & ≥35kg): TDF + 3TC (or FTC) + DTG.
- PPTCT (Prevention of Parent-to-Child Transmission): Key to an AIDS-free generation.
- Maternal ART is crucial.
- Infant ARV Prophylaxis:
- Low-risk (mom VL suppressed): NVP daily for 6 weeks.
- High-risk (mom high VL/unknown): Triple ARV for 6-12 weeks.
⭐ All infants born to HIV-infected mothers should receive ARV prophylaxis, ideally within 6-12 hours of birth.
- Breastfeeding: Encouraged with maternal ART & infant prophylaxis.

High‑Yield Points - ⚡ Biggest Takeaways
- Vertical transmission (MTCT) is the predominant route of pediatric HIV.
- Early diagnosis via HIV DNA/RNA PCR by 4-6 weeks; antibody tests unreliable early.
- Prophylaxis for Pneumocystis jirovecii pneumonia (PJP) is critical.
- Lifelong Antiretroviral Therapy (ART) should be initiated immediately in all infected children.
- Key clinical features: failure to thrive, recurrent infections, developmental delay.
- ARV prophylaxis for all HIV-exposed infants is essential (e.g., Nevirapine/Zidovudine).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

