M&E Intro & Etiology - Brain Under Siege
- Meningitis: Inflammation of meninges (pia, arachnoid, dura).
- Encephalitis: Inflammation of brain parenchyma itself.
- Meningoencephalitis: Concurrent inflammation of both meninges and brain.
Key Etiological Agents:
- Bacteria: Most common cause of pyogenic meningitis.
- Viruses: Common cause of aseptic meningitis and encephalitis.
- Fungi: Typically in immunocompromised individuals (e.g., Cryptococcus).
- TB: Causes chronic granulomatous meningitis.
Common Bacterial Etiology by Age:
| Age Group | Common Bacterial Pathogens |
|---|---|
| Neonates (<1 mo) | Group B Strep (GBS), E. coli, Listeria monocytogenes 📌 GEL |
| Infants (1-23 mo) | S. pneumoniae, N. meningitidis, H. influenzae type b (Hib) |
| Children (≥2 yrs) | S. pneumoniae, N. meningitidis |
M&E Clinical Features - Spotting the Alarms
- General: Fever, headache, irritability, vomiting. Infants: poor feeding, high-pitched cry, lethargy.
- Meningeal Signs:
- Nuchal rigidity.
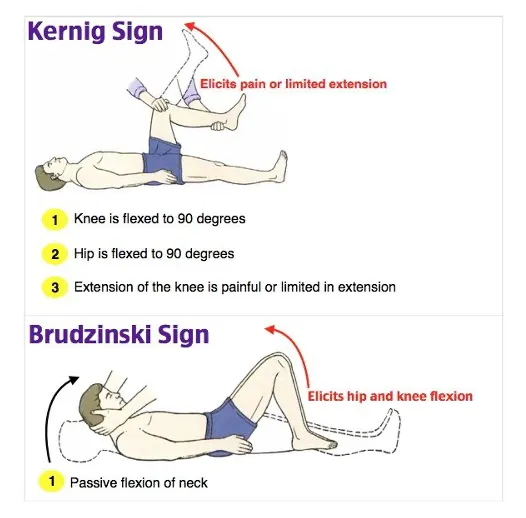
- Kernig's sign: 📌 Knee extension painful with hip flexed.
- Brudzinski's sign: 📌 Bending neck flexes hips/knees.
- Bulging fontanelle (infants).
- Alarm Bells (Red Flags):
- Rapid deterioration.
- Seizures, focal neurological deficits.
- Papilledema.
- Shock.
- Petechial/purpuric rash (⚠️ meningococcemia).
⭐ Classic triad of meningitis: fever, nuchal rigidity, altered mental status (often incomplete, especially in infants).
| Feature | Meningitis | Encephalitis |
|---|---|---|
| Site | Meninges | Brain Parenchyma |
| Key Signs | Severe headache, neck stiffness, photophobia | Altered mental status, seizures, focal deficits |
M&E Diagnosis - Decoding CSF Clues
-
Lumbar Puncture (LP): Key diagnostic. CSF if no contraindications (↑ICP signs, coagulopathy). CT head prior if focal deficits/papilledema.
-
CSF Analysis Table:
Feature Bacterial Viral TB Fungal Appearance Turbid Clear Viscous, cobweb Variable Cells (WBC/µL) >1k PMN 10-500 Lymph 100-500 Lymph <500 Lymph Protein (mg/dL) ↑↑ >100 N/↑ <100 ↑↑ >100 ↑ Glucose (mg/dL) ↓↓ <40 (Ratio <0.4) N (Ratio >0.6) ↓ <45 (Ratio <0.5) ↓ Key Tests Gram, Culture PCR AFB, PCR, ADA India Ink, CrAg
⭐ India Ink for Cryptococcus neoformans (encapsulated yeast) in CSF is classic.
-
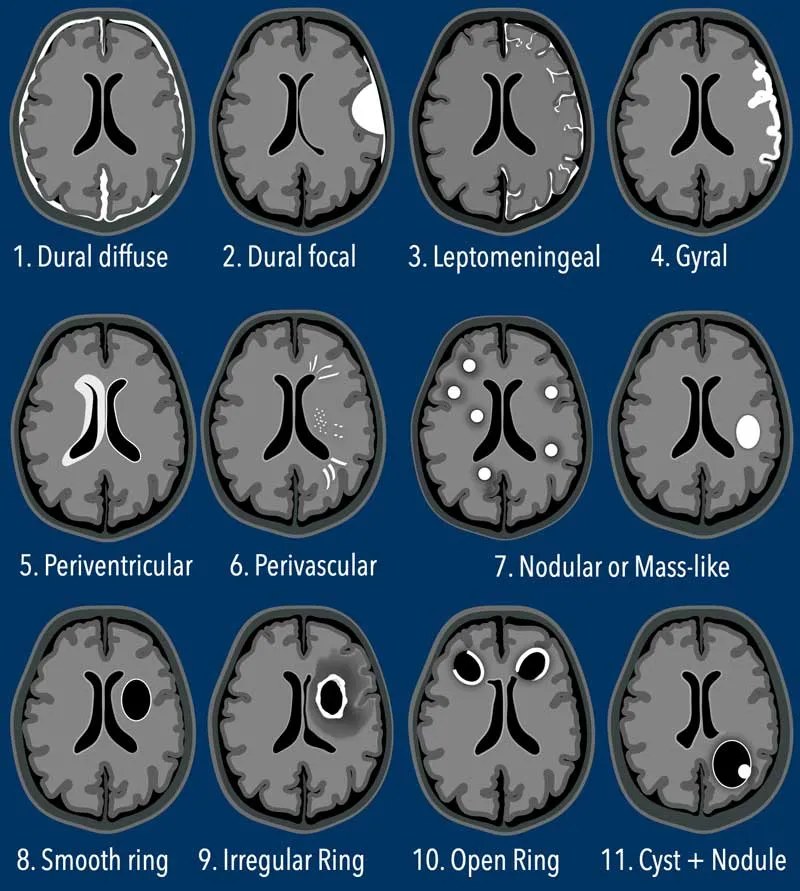
Neuroimaging (CT/MRI):
- Rules out mass/↑ICP pre-LP.
- Shows complications (hydrocephalus), meningeal enhancement.
-
CSF Interpretation Flow:
M&E Management & Prevention - Fighting & Shielding
Empirical Rx by Age:
Pathogens & Rx:
| Age | Pathogens | Rx |
|---|---|---|
| <1 mo | GBS, E.coli, Listeria | Amp + Cefotaxime/Gentamicin |
| 1-3 mo | S.pneumo, N.meni, Hib, GBS | Ceftriaxone + Amp ± Vanco |
| >3 mo | S.pneumo, N.meni, Hib | Ceftriaxone + Vanco |
- ABCs, IV fluids, vitals.
- ICP: Head up, Mannitol (0.25-1 g/kg), 3% saline.
- Seizures: IV Lorazepam, then Phenytoin.
- Dexamethasone: 0.15 mg/kg q6h x2-4d (Hib).
⭐ Dexamethasone reduces hearing loss in Hib meningitis; give with/before 1st antibiotic dose.
Prevention:
- Vaccines: Hib, PCV, MenC, MMR, Varicella.
- Chemoprophylaxis (contacts): Rifampicin.
High‑Yield Points - ⚡ Biggest Takeaways
- Bacterial meningitis pathogens by age: Neonates (GBS, E.coli, Listeria); Children (S.pneumoniae, N.meningitidis).
- CSF in bacterial meningitis: ↑Protein, ↓Glucose, ↑Neutrophils, ↑Pressure. Viral: Normal Glucose, ↑Lymphocytes.
- Kernig's and Brudzinski's signs indicate meningeal irritation.
- Empirical antibiotics: Neonates (Ampicillin + Gentamicin/Cefotaxime); Older children (Ceftriaxone + Vancomycin).
- HSV encephalitis: Temporal lobe involvement is characteristic; treat promptly with Acyclovir.
- Most common meningitis sequela: Sensorineural hearing loss.
- Lumbar Puncture (LP) contraindications: Signs of markedly ↑ICP, shock, severe coagulopathy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

