SID Intro - Acquired Immune Gaps
- Secondary Immunodeficiencies (SIDs): Acquired, not congenital, defects in the immune system.
- Far more prevalent than Primary Immunodeficiencies (PIDs).
- Onset typically later in life, resulting from extrinsic factors.
- Key Causes/Mechanisms:
- Infections (e.g., HIV targeting CD4+ T-cells).
- Malnutrition (impaired cell-mediated immunity, phagocyte function).
- Immunosuppressive drugs (e.g., corticosteroids, chemotherapy).
- Chronic diseases (e.g., diabetes, uremia, malignancies).
- Loss of immunoglobulins (e.g., nephrotic syndrome, protein-losing enteropathy).
⭐ Malnutrition is globally the leading cause of secondary immunodeficiency, affecting cell-mediated immunity, antibody production, and phagocytic function.
SID Causes - The Immune Wreckers
📌 MIDAS for common causes:
- Malnutrition:
- Protein-Energy Malnutrition (PEM) - most common global cause, impairs cell-mediated immunity, phagocyte function, antibody synthesis.
- Infections:
- Viral: HIV (progressive ↓CD4+ T-cells), Measles (transient immunosuppression), CMV, EBV.
- Bacterial: Tuberculosis.
- Drugs:
- Immunosuppressants: Corticosteroids (broad effects), Cyclosporine, Tacrolimus.
- Chemotherapy agents (myelosuppression).
- Biologics (e.g., anti-TNF agents).
- Autoimmune/Malignancy:
- Autoimmune diseases: Systemic Lupus Erythematosus (SLE).
- Malignancies: Leukemia, Lymphoma, Multiple Myeloma.
- Systemic/Stress:
- Chronic diseases: Renal failure, Liver disease, Diabetes Mellitus.
- Protein loss: Nephrotic syndrome, protein-losing enteropathy.
- Other: Major burns, Trauma, Post-splenectomy, Extremes of age.
⭐ HIV infection is the most common cause of severe secondary immunodeficiency worldwide, characterized by a profound depletion of CD4+ T-lymphocytes.
Pediatric HIV - Viral Immune Sabotage
- Transmission: Primarily vertical (mother-to-child): in-utero, intrapartum, breastfeeding.
- Pathogenesis: HIV targets CD4+ T-cells → progressive immunodeficiency.
- Diagnosis (<18m): HIV DNA/RNA PCR (maternal Ab interfere with antibody tests). Two positive virologic tests confirm.
- Staging (WHO): Clinical + CD4 counts.
- Severe immunodeficiency: CD4 <25% (<1yr), <20% (1-3yr), <15% (3-5yr), or <200 cells/µL (≥5yr).
- Management: Lifelong Antiretroviral Therapy (ART). OI prophylaxis (e.g., PCP if CD4 <25% or <1500 cells/µL in infants <1yr).
- PMTCT: Maternal ART, infant ARV prophylaxis.
⭐ Early ART (first 12 weeks of life) in HIV-infected infants drastically ↓mortality & ↑neurodevelopmental outcomes.
Other SIDs & Workup - Spotting Trouble
- Key SIDs:
- Malnutrition: Globally most common; impairs CMI, phagocyte function, IgA.
- Drug-induced: Corticosteroids, chemotherapy, immunosuppressants (e.g., biologics).
- Infections: HIV (depletes CD4+ T-cells), Measles (transient suppression).
- Protein loss: Nephrotic syndrome, protein-losing enteropathies (↓immunoglobulins).
- Asplenia/Splenectomy: Increased risk from encapsulated bacteria (Pneumococcus, Hib).
- Spotting Trouble (📌 SPUR infections):
- History: Severe, Persistent, Unusual, Recurrent infections; adverse vaccine reactions; family Hx.
- Exam: Failure to thrive (FTT), lymphadenopathy, hepatosplenomegaly, chronic eczema.
- Initial Labs: CBC with differential (lymphopenia, neutropenia), ESR/CRP.
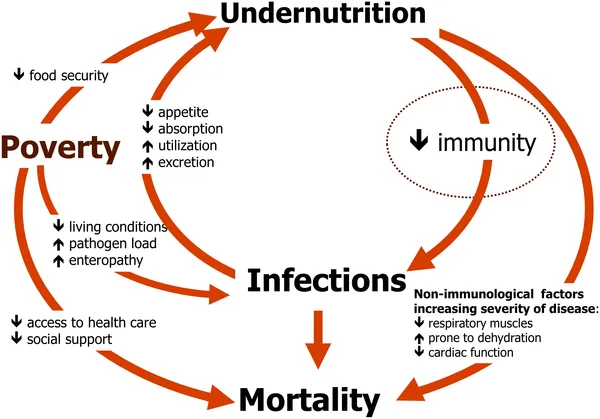
⭐ HIV is the most common infectious cause of secondary immunodeficiency worldwide, primarily targeting CD4+ T-lymphocytes.
High‑Yield Points - ⚡ Biggest Takeaways
- Malnutrition is the leading global cause of secondary immunodeficiency.
- HIV infection causes CD4+ T-cell depletion, a major secondary immunodeficiency.
- Immunosuppressive drugs like corticosteroids and chemotherapy are common iatrogenic causes.
- Hematologic malignancies (e.g., leukemia, lymphoma) frequently lead to immune defects.
- Protein-losing states (e.g., nephrotic syndrome) result in hypogammaglobulinemia.
- Splenectomy ↑ risk of infection by encapsulated organisms.
- Chronic infections (e.g., tuberculosis, measles) can suppress host immunity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

