Pediatric Autoimmunity Overview - Tiny Troublemakers
- Immune system mistakenly targets self-antigens, leading to tissue damage; a failure of "self-tolerance."
- Pediatric onset: Often more aggressive, potentially affecting multiple organ systems.
- Etiology: Multifactorial.
- Genetic susceptibility (e.g., HLA-DR, PTPN22).
- Environmental triggers (infections like EBV, Strep; UV light).
- Hormonal factors (pubertal changes).
- Pathogenesis: Involves T & B cell dysregulation, autoantibody production, molecular mimicry.
- Common examples: JIA, SLE, Type 1 DM, Celiac disease, Autoimmune hepatitis.
⭐ Antinuclear Antibody (ANA) is a frequently positive screening test in pediatric rheumatology, but its presence alone is not diagnostic and requires careful clinical correlation.
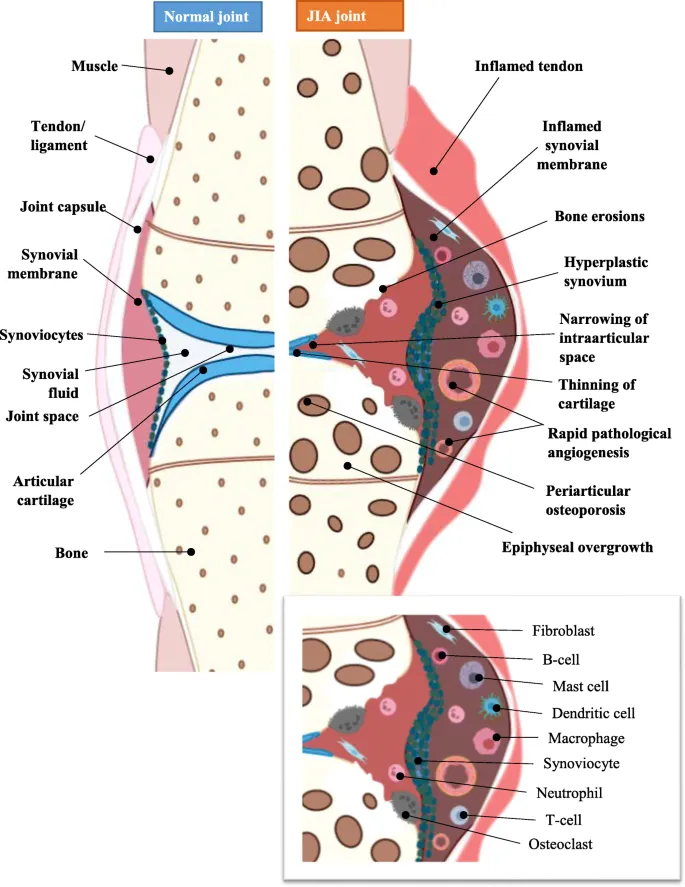
Juvenile Idiopathic Arthritis (JIA) - Joint Jamboree
- Chronic arthritis (> 6 weeks) in children < 16 years; diagnosis of exclusion. 📌 JIA = Juvenile Inflammation of Articulations.
- Key Subtypes (ILAR):
- Oligoarticular: ≤4 joints. Most common. High uveitis risk if ANA+.
- Polyarticular (RF- & RF+): ≥5 joints. Symmetric involvement common.
- Systemic (Still's Disease): Arthritis, quotidian fever (spikes daily), evanescent "salmon-pink" rash.
- Enthesitis-related: Arthritis & enthesitis (e.g., heel pain). HLA-B27 often +.
- Psoriatic: Arthritis & psoriasis (or family history).
- Complications: Uveitis (screen!), growth disturbances, Macrophage Activation Syndrome (MAS) in Systemic JIA.
- Rx: NSAIDs, DMARDs (Methotrexate), Biologics (e.g., anti-TNF), Corticosteroids.
⭐ Oligoarticular JIA, ANA-positive, has highest risk of chronic anterior uveitis; regular eye exams crucial.
Pediatric SLE & JDM - Systemic Storms
- Pediatric Systemic Lupus Erythematosus (SLE)
- Multisystem autoimmune; F:M ratio ~4.5:1 (prepubertal), ↑ to 8:1 (postpubertal).
- 📌 SOAP BRAIN MD criteria (Serositis, Oral ulcers, Arthritis, Photosensitivity, Blood, Renal, ANA, Immunologic, Neurologic, Malar, Discoid).
- Key Abs: ANA (sensitive), Anti-dsDNA (specific, nephritis marker), Anti-Sm (highly specific).
- Tx: Corticosteroids, Hydroxychloroquine (HCQ); severe: Mycophenolate Mofetil (MMF), Cyclophosphamide.
- Juvenile Dermatomyositis (JDM)
- Characteristic rash + proximal muscle weakness.
- Skin: Heliotrope rash (eyelids), Gottron's papules (extensor surfaces), malar rash.
- Muscle: Symmetrical proximal weakness; ↑CK, ↑Aldolase, ↑LDH.
- Key Abs: Anti-Mi-2 (classic), Anti-MDA5 (ulceration, ILD), Anti-NXP2 (calcinosis).
- Tx: Corticosteroids, Methotrexate; IVIG for severe/refractory.

- ⭐ > In JDM, Anti-MDA5 antibodies are associated with rapidly progressive interstitial lung disease (RP-ILD) and skin ulcerations.
Pediatric Vasculitides (Kawasaki & HSP) - Vessel Vandals
Kawasaki Disease (KD): Mucocutaneous Lymph Node Syndrome
- Acute febrile illness, medium vessel vasculitis.
- 📌 CRASH & Burn: Fever ≥5 days PLUS ≥4 of:
- Conjunctivitis (bilateral, non-exudative)
- Rash (polymorphous, non-vesicular)
- Adenopathy (cervical, ≥1.5cm, usually unilateral)
- Strawberry tongue, red/cracked lips
- Hand/foot edema, erythema, periungual desquamation
- Complication: Coronary artery aneurysms (CAA). Echo vital.
- Treatment: IVIG (2g/kg) + high-dose Aspirin (ASA) (80-100mg/kg/day initially), then low-dose ASA.
Henoch-Schönlein Purpura (HSP) / IgA Vasculitis
- Most common childhood systemic vasculitis. Small vessels.
- Often post-URI.
- 📌 Classic Tetrad (PAAR):
- Palpable purpura (buttocks, lower limbs; non-thrombocytopenic)
- Arthritis/arthralgia (large joints, esp. ankles/knees)
- Abdominal pain (colicky; risk of intussusception, GI bleed)
- Renal involvement (hematuria/proteinuria; IgA nephropathy)
- Diagnosis: Clinical. Skin biopsy (if atypical): leukocytoclastic vasculitis, IgA deposition.
- Treatment: Supportive (hydration, analgesia). Corticosteroids for severe GI/renal involvement.

⭐ Kawasaki Disease is the leading cause of acquired heart disease in children in developed countries; timely IVIG reduces coronary aneurysm risk from ~25% to <5%.
High‑Yield Points - ⚡ Biggest Takeaways
- JIA: Most common pediatric rheumatic disease; oligoarticular often ANA+, risk of uveitis.
- SLE: Malar rash, nephritis, cytopenias; anti-dsDNA & anti-Sm are specific markers.
- Kawasaki Disease: Fever, conjunctivitis, rash, mucositis; risk of coronary artery aneurysms.
- IgA Vasculitis (HSP): Palpable purpura, arthritis, abdominal pain, nephritis.
- JDM: Proximal muscle weakness with Gottron's papules & heliotrope rash.
- Type 1 DM: Autoimmune destruction of pancreatic β-cells; linked to HLA-DR3/DR4.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

