Intro & Pathophysiology - Itchy Skin Saga
- Chronic, relapsing inflammatory skin disease; hallmark: intense pruritus. Often called "the itch that rashes."
- Prevalence: Affects ~10-20% of children and 1-3% of adults.
- Pathophysiology: Multifactorial interaction.
- Genetic Susceptibility: Mutations in Filaggrin (FLG) gene → impaired epidermal barrier function.
- Immune Dysregulation: Predominantly a Th2-mediated response (↑IL-4, ↑IL-5, ↑IL-13) → ↑IgE production & eosinophilia.
- Epidermal Barrier Dysfunction: ↓Ceramides, ↑Transepidermal Water Loss (TEWL).
- Triggers: Allergens (food, aeroallergens), irritants, microbial factors (e.g., Staphylococcus aureus colonization).
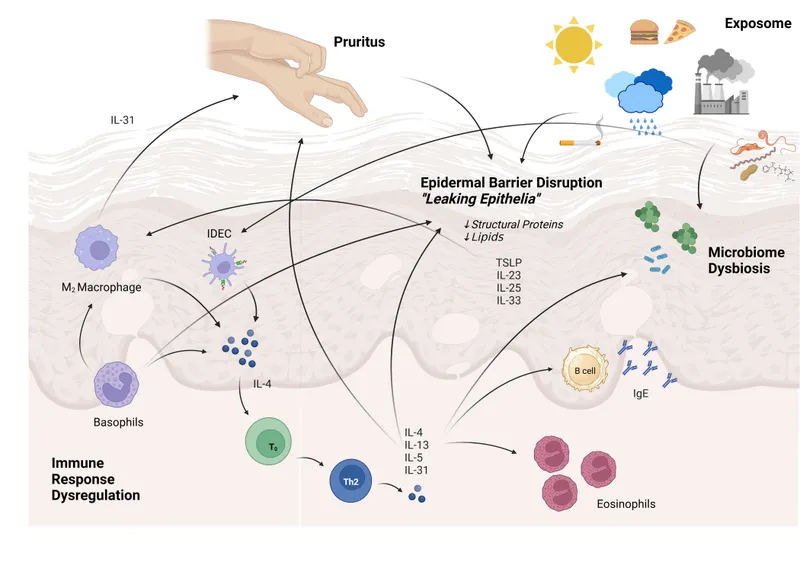
⭐ Atopic dermatitis is classically described as "the itch that rashes," emphasizing that pruritus is the primary symptom that typically precedes the development of visible skin lesions, unlike many other dermatoses where the rash appears first and then itches.
Clinical Picture - Rash & Scratch
- Pruritus: Intense, hallmark symptom; "the itch that rashes." Often disrupts sleep.
- Age-Dependent Rash Patterns:
- Infantile (birth - 2 yrs):
- Acute: Erythematous papules, vesicles, oozing, crusting.
- Distribution: Cheeks, forehead, scalp, extensor surfaces of limbs, trunk.
- 📌 Diaper area typically spared.

- Childhood (2 - 12 yrs):
- Chronic: Lichenification (thickened skin, prominent skin lines), xerosis (dry skin).
- Distribution: Flexural areas (antecubital & popliteal fossae, wrists, ankles, neck).
- Adolescent/Adult (>12 yrs):
- Similar to childhood; flexural lichenification, hand/foot dermatitis, head/neck involvement.
- Infantile (birth - 2 yrs):
- Other Stigmata:
- Dennie-Morgan infraorbital folds.
- Allergic shiners (infraorbital hyperpigmentation).
⭐ Distribution is key: extensor surfaces in infants, flexural surfaces in older children/adults an exam-favourite distinguishing point for different age presentations of Atopic Dermatitis.
Diagnosis & Workup - Spotting the Itch
Error generating content for this concept group: Failed to process successful response
Management & Complications - Soothe & Shield
Management (Soothe):
- Emollients: Cornerstone; liberal, frequent application. Avoid known triggers.
- Topical Corticosteroids (TCS): Potency matched to severity/site (e.g., Hydrocortisone 1% for mild).
- Topical Calcineurin Inhibitors (TCI): Tacrolimus, Pimecrolimus (face, folds; steroid-sparing, no atrophy).
- Antihistamines: For pruritus control (sedating options for sleep).
- Wet Wraps: Acute, severe flares; cooling & hydration.
- Systemic Therapy (refractory): Short-course oral steroids, Cyclosporine, Azathioprine, Dupilumab.
Complications (Shield):
- Skin Infections:
- Bacterial: Staphylococcus aureus (impetiginization, secondary infection).
- Viral: Eczema herpeticum (HSV), Molluscum contagiosum.
- Ocular: Atopic keratoconjunctivitis, anterior subcapsular cataracts.
- Psychosocial: Sleep disturbance, anxiety, ↓QoL.
- Growth Retardation: Chronic severe disease or prolonged systemic steroids.

⭐ Eczema herpeticum: Dermatological emergency (HSV in AD); painful, monomorphic, umbilicated vesicles. Prompt systemic antivirals needed.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic, relapsing inflammatory skin condition, strongly linked to personal/family history of atopy (asthma, allergic rhinitis).
- Intense pruritus ("the itch that rashes") is the hallmark symptom, often preceding skin lesions.
- Characteristic age-dependent lesion distribution: facial/extensor surfaces in infants, flexural areas in older children/adults.
- Key pathogenic factors include skin barrier dysfunction (e.g., filaggrin gene mutations) and immune dysregulation (Th2 predominance).
- Management cornerstones: liberal emollient use, topical corticosteroids, and topical calcineurin inhibitors.
- Patients are prone to secondary bacterial (Staphylococcus aureus) and viral (eczema herpeticum) infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

