Thrombocytopenia - Platelet Plunge Primer
- Definition: Platelet count < 150,000/μL.
- Broad Etiologies:
- Decreased Production:
- Bone marrow disorders (aplastic anemia, leukemia, MDS).
- Drugs (chemotherapy), infections (HIV, HCV).
- Nutritional deficiencies (B12, folate).
- Increased Destruction:
- Immune: ITP, drug-induced (e.g., heparin - HIT), SLE.
- Non-immune: DIC, TTP, HUS, HELLP syndrome.
- Sequestration: Hypersplenism (e.g., cirrhosis, portal hypertension).
- Dilutional: Massive transfusions.
- Decreased Production:
⭐ Immune Thrombocytopenic Purpura (ITP) is often triggered by a preceding viral infection, especially in children, and involves autoantibodies against platelet glycoproteins like GPIIb/IIIa or GPIb-IX.
Etiology - The Platelet Pilferers
- Decreased Production (Marrow Aplasia/Infiltration/Suppression)
- Congenital: Fanconi anemia, TAR syndrome, WAS, Amegakaryocytic thrombocytopenia.
- Acquired: Aplastic anemia, Leukemia/Lymphoma, Myelodysplasia, Viral (HIV, CMV, EBV, Parvo B19), Drugs (chemo, valproate, linezolid), Nutritional (B12/Folate).
- Increased Destruction (Peripheral Consumption)
- Immune-Mediated:
- ITP (Immune Thrombocytopenic Purpura): Most common in children.
⭐ ITP is the most common cause of isolated thrombocytopenia in an otherwise healthy child, typically occurring 1-4 weeks after a viral infection.
- NAIT (Neonatal Alloimmune Thrombocytopenia): Maternal IgG vs fetal platelets.
- Autoimmune (SLE, Evans Syndrome).
- Drug-Induced (heparin, quinine, sulfonamides, vancomycin).
- Non-Immune Mediated:
- DIC (Disseminated Intravascular Coagulation).
- HUS (Hemolytic Uremic Syndrome)/TTP (Thrombotic Thrombocytopenic Purpura).
- Kasabach-Merritt Syndrome.
- Immune-Mediated:
- Sequestration: Hypersplenism.
- Dilutional: Massive transfusions.
Clinical Clues & Dx - Spotting the Shortage
- Clinical Signs: Often asymptomatic. Mucocutaneous bleeding: petechiae, purpura, ecchymoses. Epistaxis, gingival, GI/GU bleeding. Severe: ICH risk. Splenomegaly? (sequestration/destruction). No lymphadenopathy/fever in isolated ITP.
- Key Investigations:
- CBC & Peripheral Smear (PBS): Confirms true thrombocytopenia (platelets <150,000/µL), rules out pseudothrombocytopenia (EDTA clumps). Platelet morphology: large (ITP), small (WAS). Schistocytes? (TTP/HUS). Blasts? (Leukemia).
- Coagulation: PT/aPTT normal in isolated thrombocytopenia.
- Bone Marrow Exam (BME): Not routine. For atypical cases, other cytopenias, failed therapy, pre-splenectomy. ITP: normal/↑ megakaryocytes.
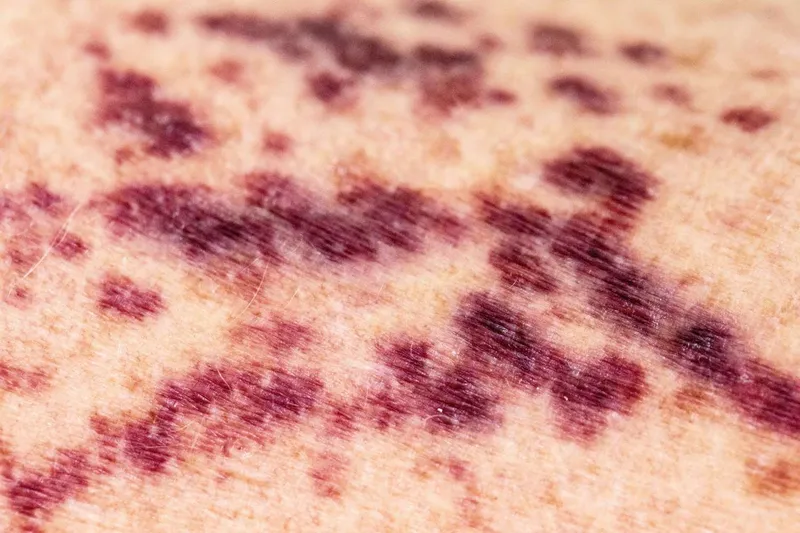
⭐ Petechiae (pinpoint, non-blanching spots) are hallmark of thrombocytopenia; large bruises/joint bleeds suggest coagulopathy.
Key Syndromes - Syndrome Showdown: ITP, HUS, NAIT
-
Immune Thrombocytopenic Purpura (ITP)
- Patho: Anti-GpIIb/IIIa IgG autoantibodies.
- Onset: Acute (children, post-viral), Chronic (adults).
- Features: Isolated thrombocytopenia, mucocutaneous bleeding. Normal spleen.
- Labs: ↓ Platelets, giant platelets. Marrow: ↑ megakaryocytes.
- Rx: Observation, Steroids, IVIG.
-
Hemolytic Uremic Syndrome (HUS)
- Patho: Endothelial damage by Shiga toxin (E.coli O157:H7) or complement dysregulation (atypical).
- Onset: Children <5 yrs (typical).
- Features: Triad: MAHA, Thrombocytopenia, AKI. Often post-bloody diarrhea.
- Labs: ↓ Platelets, schistocytes, ↑LDH, ↑Creatinine.
- Rx: Supportive. Plasma exchange (atypical).
⭐ HUS: Avoid antibiotics for E.coli O157:H7 gastroenteritis; may ↑ toxin release & HUS risk.
-
Neonatal Alloimmune Thrombocytopenia (NAIT)
- Patho: Maternal IgG anti-HPA-1a (common) vs fetal platelets.
- Onset: Neonates (hours post-birth).
- Features: Severe thrombocytopenia; petechiae, purpura. ICH risk ~10-20%.
- Labs: ↓ Neonatal platelets, normal maternal count.
- Rx: IVIG, HPA-matched/washed maternal platelets.
High‑Yield Points - ⚡ Biggest Takeaways
- Immune Thrombocytopenia (ITP): Most common acquired cause in children, often post-viral, usually self-limiting; observe or treat if severe.
- Wiskott-Aldrich Syndrome (X-linked): Microthrombocytopenia (small platelets), eczema, recurrent infections.
- Bernard-Soulier Syndrome: Giant platelets, defective adhesion (GP Ib/IX/V deficiency), AR inheritance.
- Glanzmann Thrombasthenia: Normal platelet count, defective aggregation (GP IIb/IIIa deficiency), AR inheritance.
- Neonatal Alloimmune Thrombocytopenia (NAIT): Maternal IgG anti-platelet antibodies (e.g., anti-HPA-1a) crossing placenta, risk of intracranial hemorrhage.
- Kasabach-Merritt Syndrome: Consumptive thrombocytopenia associated with large vascular tumors (e.g., kaposiform hemangioendothelioma).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

