Blood Basics & Typing - Tiny Titans' Type
- ABO/Rh System:
- Neonates: May lack isohemagglutinins (develop by 3-6 months). Maternal IgG anti-A/B can cross placenta.
- Rh(D) typing critical: Prevents Hemolytic Disease of Newborn (HDN).
- Cross-matching:
- Major: Donor RBCs vs Recipient Serum (Primary).
- Minor: Donor Serum vs Recipient RBCs.
- Indications: Symptomatic anemia, active bleeding, coagulopathy.
⭐ Universal donor (RBCs): O Rh-negative. Universal donor (Plasma): AB. 📌 O-Negative: Oh! No antigens!
Red Cell Rhapsody - Ruby Rescuers
- Packed Red Blood Cells (PRBCs)
- Indications: Symptomatic anemia, acute blood loss (Hb <7 g/dL in stable patients; higher thresholds for cyanotic heart disease, severe hypoxemia).
- Dose: 10-15 mL/kg over 2-4 hours.
- Expected rise: Hb by 2-3 g/dL.
- Special Preparations:
- Leukoreduced: Prevents CMV transmission, reduces Febrile Non-Hemolytic Transfusion Reactions (FNHTR).
- Irradiated: Prevents Transfusion-Associated Graft-versus-Host Disease (TA-GVHD) in immunocompromised patients.
- Washed: For IgA deficiency, history of recurrent severe allergic reactions.
⭐ One unit of PRBCs (or 10-15 mL/kg) is expected to raise hemoglobin by approximately 2-3 g/dL or hematocrit by 6-9%.
Platelet Power-Up - Clotting Crusaders
- Indications:
- Prophylactic: Count <10,000-20,000/µL (stable aplastic anemia/chemo).
- Therapeutic: Active bleeding + low platelets; Pre-procedure if count <50,000/µL.
- Neonatal thresholds differ.
- Dose: 1 RDP unit/10 kg or 1 SDP unit (apheresis).
- Expected Increment: ↑30,000-50,000/µL per SDP (or 4-6 RDPs); adjust for peds.
- Platelet Refractoriness: Poor increment.
- Causes: Immune (HLA/HPA alloimmunization); Non-immune (sepsis, splenomegaly, DIC, drugs).
⭐ For HLA alloimmunization-induced refractoriness, use HLA-matched or crossmatch-compatible platelets.
Plasma & Cryo Crew - Coagulation Champions
- Fresh Frozen Plasma (FFP)
- Contents: All coagulation factors, plasma proteins (albumin, globulins).
- Indications: Active bleeding with multiple coagulation factor deficiencies (e.g., liver disease, DIC), urgent warfarin reversal.
- Dose: 10-20 mL/kg.
- Cryoprecipitate
- Contents: Fibrinogen, Factor VIII (FVIII), Factor XIII (FXIII), von Willebrand Factor (vWF), fibronectin. 📌 Cryo is RICH in Fibrinogen, Factor 8, Factor 13, vWF.
- Indications: Hypofibrinogenemia (e.g., DIC, massive transfusion), Factor XIII deficiency, von Willebrand Disease (vWD) if specific factor concentrates are unavailable.
- Dose: 1-2 units/10 kg.
- ⭐
Cryoprecipitate is the most concentrated source of fibrinogen.

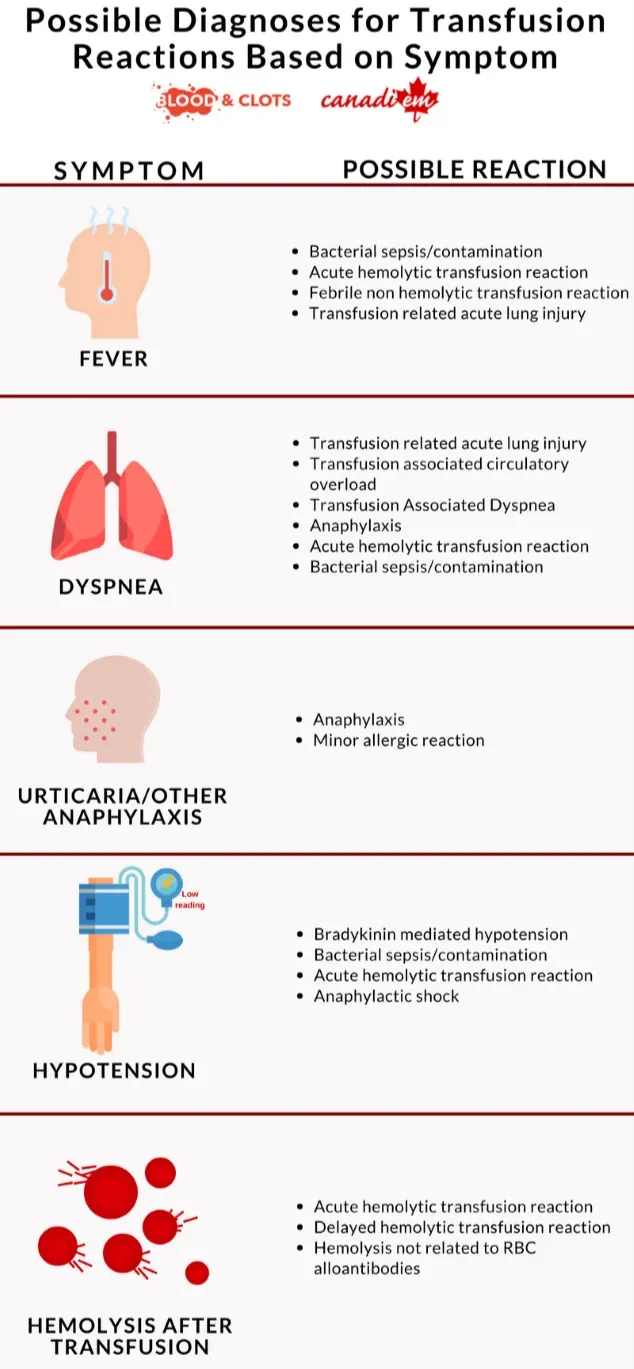
Transfusion Troubles - Reaction Rescue
- Acute Reactions (STOP Transfusion First!)
- Allergic/Anaphylactic: Urticaria, wheeze. Rx: Antihistamines, epinephrine.
- AHTR: Fever, hemoglobinuria, shock. Rx: IV fluids, support.
- FNHTR: Fever, chills. Rx: Antipyretics. Prevent: Leukoreduction.
- TRALI: Dyspnea, hypoxia, infiltrates (within 6h). Rx: O2, ventilation.
- TACO: Dyspnea, ↑JVP, edema. Rx: Diuretics, O2.
- Delayed Reactions
- DHTR: Jaundice, ↓Hb (5-10d).
- TA-GVHD: Rash, pancytopenia. Prevent: Irradiation.
- Post-transfusion Purpura: ↓Platelets (~7d).
- Iron Overload: Chronic. Rx: Chelation.
⭐ TRALI: Leading cause of transfusion mortality. Acute respiratory distress, bilateral pulmonary infiltrates within 6 hrs post-transfusion, not due to circulatory overload.
High‑Yield Points - ⚡ Biggest Takeaways
- PRBCs indicated for symptomatic anemia or Hb < 7 g/dL in stable children.
- Platelets for active bleeding with thrombocytopenia or prophylactically if counts < 10,000-20,000/µL.
- FFP replaces multiple coagulation factors; used in DIC, liver disease, warfarin reversal.
- Cryoprecipitate provides fibrinogen, Factor VIII, vWF; for hypofibrinogenemia, hemophilia A.
- Irradiation of blood products prevents TA-GVHD in immunocompromised individuals.
- Leukoreduction reduces risks of FNHTR, CMV transmission, and HLA alloimmunization.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

