Definition & Classification - Anemia ABCs
- Definition: Hemoglobin (Hb) or Hematocrit (Hct) concentration >2 Standard Deviations (SD) below the mean for age and sex.
- WHO Hb Cutoffs (g/dL):
- 6 months - 5 years: <11
- 5 - 11 years: <11.5
- 12 - 14 years: <12
⭐ The most common type of anemia globally and in children is Iron Deficiency Anemia.
Iron Deficiency Anemia - Rusty Pipes Puzzles
- Etiology: Inadequate intake (exclusive breastfeeding >6 months, cow's milk), prematurity, chronic blood loss (hookworm), malabsorption.
- Clinical Features: Pallor, fatigue, irritability, pica. Koilonychia (spoon nails), glossitis.
- Investigations:
- CBC: ↓Hb, ↓MCV (<80 fL), ↓MCH, ↓MCHC, ↑RDW (>15%).
- Iron Profile: ↓S. Ferritin (<15 ng/mL or <30 ng/mL with inflammation), ↓S. Iron, ↑TIBC, ↓Transferrin saturation (<16%). 📌 TIBC ↑, Ferritin ↓.
- Management:
- Oral elemental iron: 3-6 mg/kg/day.
- Continue for 2-3 months after Hb normalizes.
⭐ Exclusive breastfeeding beyond 6 months without iron supplementation is a major risk factor for IDA in infants.
Megaloblastic Anemias - Big Cell Conundrums
Impaired DNA synthesis. MCV > 100 fL. Smear: macro-ovalocytes, hypersegmented neutrophils (>5% with 5 lobes or any with 6 lobes).
| Feature | Vit B12 Deficiency | Folate Deficiency |
|---|---|---|
| Causes | Pernicious anemia, gastrectomy, vegan, D. latum | Goat's milk, poor diet, MTX, phenytoin, ↑demand |
| Neuro Sx | YES (SCD) | NO |
| Labs | ↓B12, ↑MMA, ↑Homocysteine | ↓Folate, N MMA, ↑Homocysteine |
⭐ Goat's milk (folate-deficient) → megaloblastic anemia in infants if primary feed, unsupplemented.
Hemolytic Anemias - Red Cell Rampage
- Increased RBC destruction. Key signs: ↑Reticulocytes, ↑Indirect Bilirubin, ↓Haptoglobin, Splenomegaly.
- Diagnostic Approach:
-
Common Hereditary Hemolytic Anemias:
Feature Thalassemia Major (β-thal) Sickle Cell Anemia (SCA) Hereditary Spherocytosis (HS) Defect ↓/absent β-globin chains Abnormal β-globin (HbS) RBC membrane protein defect (e.g., spectrin) Smear Target cells, microcytic, hypochromic, NRBCs Sickled cells, Howell-Jolly bodies Spherocytes, ↑MCHC Hb Electrophoresis ↑HbF, ↑HbA2 (>3.5% for trait), ↓/absent HbA HbS predominant, HbF variable, no HbA Normal (usually) Specific Test Hb electrophoresis Sickling test, Hb electrophoresis Osmotic fragility test, EMA binding -
📌 SCA Crisis Triggers (FAT RBC): Fever, Acidosis, Temperature changes, Reduced O2, Dehydration, Exertion, Stress.
-

⭐ Hydroxyurea increases HbF levels and is used in the management of Sickle Cell Anemia to reduce crisis frequency.
Aplastic & Other Anemias - Marrow Meltdown
-
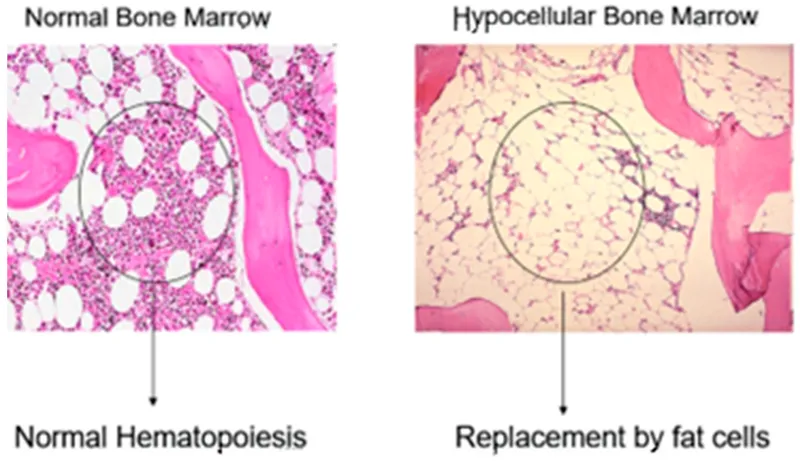
Aplastic Anemia (AA): Pancytopenia, hypocellular marrow. Causes: idiopathic, drugs, viruses.
- Severe: BM <25% + 2 of: ANC <0.5, Plt <20, Retic <20 (x10⁹/L).
- Tx: IST, HSCT.
-
Fanconi Anemia (FA): AR, DNA repair defect → pancytopenia. Café-au-lait, thumb/radial defects. Dx: DEB test.
-
Diamond-Blackfan Anemia (DBA): Congenital PRCA. Macrocytic anemia, reticulocytopenia. Craniofacial/thumb defects. ↑eADA.
⭐ Diamond-Blackfan Anemia is a congenital pure red cell aplasia often associated with craniofacial and thumb abnormalities, and elevated erythrocyte adenosine deaminase (eADA).
-
Transient Erythroblastopenia of Childhood (TEC): Acquired PRCA (1-4y), post-viral. Spontaneous recovery.
High‑Yield Points - ⚡ Biggest Takeaways
- Iron Deficiency Anemia (IDA): Most common; screen at 9-12 months; microcytic, hypochromic.
- Thalassemia Major: Severe anemia at 6-9 months, hepatosplenomegaly, requires lifelong transfusions.
- Sickle Cell Anemia: Crisis by hypoxia, infection, dehydration; hydroxyurea ↑ HbF.
- G6PD Deficiency: Hemolysis with oxidant drugs (e.g., primaquine) or fava beans.
- Hereditary Spherocytosis: Microspherocytes, ↑ MCHC, osmotic fragility; splenectomy is curative.
- Aplastic Anemia: Pancytopenia with hypocellular bone marrow.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


