Definitions & Types - The Runs Rundown
- Duration Classifications:
- Acute Diarrhea: Lasts <14 days.
- Persistent Diarrhea: Lasts 14-29 days.
- Chronic Diarrhea: Lasts ≥30 days.
- Major Pathophysiological Types: Osmotic, Secretory, Inflammatory, Dysenteric (📌 OSID).
- Stool Osmotic Gap (SOG): $290 - 2 \times (Stool\ Na^+ + Stool\ K^+)$.
- Osmotic: SOG > 100 mOsm/kg.
- Secretory: SOG < 50 mOsm/kg.
⭐ In India, Rotavirus is the most common cause of severe dehydrating diarrhea in children <2 years.
Acute Diarrhea: Causes & Signs - Bugs & Bellyaches
Common Pathogens & Features:
| Category | Pathogen | Stool | Key Features |
|---|---|---|---|
| Viral | Rota, Noro | Watery | Vomiting, fever |
| Bacterial | ETEC, EPEC | Watery | 📌 ETEC: Trav; EPEC: Peds |
| EHEC, EIEC | Bloody | 📌 EHEC: HUS; EIEC: Inv | |
| V. cholerae | Watery | Profuse, rice-water, painless | |
| Shigella | Bloody | Mucoid, fever, tenesmus | |
| Salmonella | Bloody/W | Fever | |
| Campylobacter | Bloody | Fever, abd pain | |
| Parasitic | Giardia | Watery | Foul, malabsorption |
| Cryptosporidium | Watery | Prolonged (imm.comp.) | |
| E. histolytica | Bloody | Flask ulcers |
WHO Dehydration Assessment:
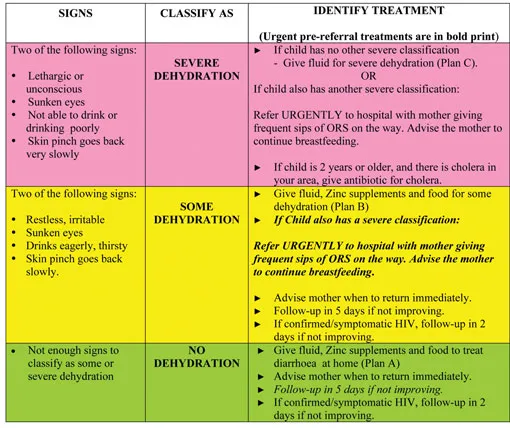
- No Dehydration: <5% wt loss. Alert, drinks normally.
- Some Dehydration: 5-10% wt loss. Restless, irritable, drinks eagerly.
- Severe Dehydration: >10% wt loss. Lethargic, sunken eyes, drinks poorly/unable.
Red Flags:
- Persistent vomiting
- Severe dehydration signs
- Bloody stools
- High fever
- No improvement >48h
Etiological Approach:
Acute Diarrhea: Management - Quenching The Thirst
Primary goal: Rehydration using Oral Rehydration Solution (ORS). WHO-ORS Composition (mOsm/L):
| Component | Standard | Low Osmolarity |
|---|---|---|
| Sodium (Na) | 90 | 75 |
| Potassium (K) | 20 | 20 |
| Chloride (Cl) | 80 | 65 |
| Citrate | 10 | 10 |
| Glucose | 111 | 75 |
| Total Osmolarity | 311 | 245 |
Dehydration Management Plan:
- Zinc: Supplement 10mg daily (<6mo) or 20mg daily (>6mo) for 14 days.
- Antibiotics: Indicated for dysentery (shigellosis), suspected cholera, or specific pathogen.
- Avoid: Antidiarrheals (e.g., loperamide) and antiemetics are generally not recommended.
- Nutrition: Continue breastfeeding/age-appropriate diet; avoid BRAT diet.
- Prevention: Hand hygiene, safe water, Rotavirus vaccination.
⭐ Zinc supplementation in acute diarrhea reduces duration and severity of the episode and prevents future episodes.
Chronic Diarrhea: Etiology - The Long Haul
Defined as diarrhea lasting ≥30 days.
Common Causes & Stool Characteristics in Indian Children:
| Etiology | Key Features | Stool Type |
|---|---|---|
| Toddler's Diarrhea | Thriving child, undigested food particles | Watery, loose |
| Post-infectious | Follows acute GE, persistent mucosal damage | Watery |
| Lactose Intolerance | Bloating, cramps, resolves with lactose removal | Watery, frothy |
| Celiac Disease | FTT, villous atrophy, gluten-sensitive | Fatty, bulky |
| Cow's Milk Protein Allergy | Vomiting, eczema, blood in stool (infants) | Watery, bloody |
| IBD (Crohn's, UC) | Abdominal pain, weight loss, bloody stools | Bloody, mucoid |
| Cystic Fibrosis | FTT, respiratory sx, ↓ fecal elastase | Fatty, foul |
| Immunodeficiency | Recurrent infections, opportunistic pathogens | Variable |
- Celiac disease
- H (H.pylori - not a cause, but a common GI differential)
- Rotavirus (post-infectious)
- Other (Cystic Fibrosis, IBD)
- Nutrition (Toddler's diarrhea)
- Intolerance (Lactose)
- Cow's milk protein allergy

⭐ Toddler’s diarrhea is characterized by painless passage of loose stools with undigested food particles in a thriving child.
Chronic Diarrhea: Investigation - Detective Work
⭐ Elevated IgA anti-tissue transglutaminase (anti-tTG) antibodies are highly specific for Celiac Disease screening.
High‑Yield Points - ⚡ Biggest Takeaways
- Acute diarrhea: most commonly viral (e.g., Rotavirus); Oral Rehydration Solution (ORS) is the cornerstone of management.
- Persistent diarrhea lasts >14 days; requires investigation for secondary infections or malabsorption.
- Chronic diarrhea lasts >4 weeks; consider Celiac disease, lactose intolerance, or Inflammatory Bowel Disease (IBD).
- Red flag signs in diarrhea include blood or mucus in stool, severe dehydration, persistent vomiting, and failure to thrive.
- Celiac disease screening involves IgA anti-tissue transglutaminase (anti-tTG) antibodies; diagnosis confirmed by duodenal biopsy.
- Lactose intolerance can be diagnosed by a hydrogen breath test or clinical improvement with lactose elimination.
- Toddler's diarrhea (chronic non-specific diarrhea) is typically benign, often linked to excessive fruit juice intake or a low-fat, high-fiber diet.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

