Pituitary Anatomy & Hormones - Gland Central
- Anatomy: Sella turcica. Lobes:
- Anterior (Adenohypophysis): Rathke's pouch origin.
- Posterior (Neurohypophysis): Neural ectoderm.
- Hypothalamic Control: Via infundibulum.
- Anterior: Portal system (releasing/inhibiting hormones).
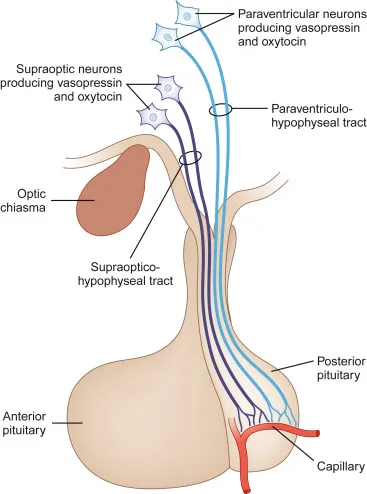
- Posterior: Neural; stores ADH (supraoptic), Oxytocin (paraventricular) made in hypothalamus.
- Hormones (Anterior): GH, PRL, ACTH, TSH, FSH, LH. 📌 (FLAT PEG)
⭐ Craniopharyngioma, from Rathke's pouch remnants, is a common pediatric suprasellar tumor causing visual field defects.
Growth Hormone Disorders - Ups & Downs
Growth Hormone (GH) from anterior pituitary, regulated by GHRH & Somatostatin, is vital for linear growth via IGF-1. Imbalances lead to significant disorders.
GH Deficiency (GHD) vs. GH Excess
| Aspect | GH Deficiency (GHD) | GH Excess (Gigantism/Acromegaly) |
|---|---|---|
| Key Features | ↓Growth velocity, short stature (<-2 SD), delayed bone age | Gigantism (children), Acromegaly (adults), ↑IGF-1 |
| Diagnosis | ↓IGF-1; GH stim test: peak GH <7-10 ng/mL | ↑IGF-1; OGTT: GH not suppressed <1 ng/mL |
| Treatment | Recombinant hGH (rhGH) | Surgery, Somatostatin analogues (e.g., Octreotide) |
⭐ Laron Syndrome: GH receptor defect → GH insensitivity. Features: Dwarfism, high GH, low IGF-1. Autosomal Recessive.
📌 Mnemonic for common GH stimulation tests: "CLAG" (Clonidine, L-DOPA, Arginine, Glucagon/Insulin).
Other Anterior Pituitary Issues - Command Crisis
- Panhypopituitarism: Deficiency of ≥1 anterior pituitary hormones.
- Causes: Tumors (craniopharyngioma), Sheehan's syndrome, trauma, radiation, infiltrative disease.
- 📌 Hormone loss sequence: GH → LH/FSH → TSH → ACTH (Mnemonic: "Go Look For The Adenoma").
- Dx: Low basal hormones, dynamic stimulation tests (e.g., Insulin Tolerance Test). Rx: Hormone replacement.
- Cushing's Disease: ACTH-secreting pituitary adenoma → ↑cortisol.
- Features: Central obesity, moon facies, purple striae, hypertension, glucose intolerance.
- Dx: ↑24h UFC, no suppression on LDDST (Low-Dose Dexamethasone Suppression Test), suppression on HDDST (High-Dose Dexamethasone Suppression Test), ↑ACTH.
- Rx: Transsphenoidal surgery.

⭐ Nelson's Syndrome: Pituitary adenoma growth, ↑ACTH & hyperpigmentation post-bilateral adrenalectomy for Cushing's disease treatment.
Posterior Pituitary Disorders - Water Works
- Diabetes Insipidus (DI): "Dry Inside" - ↓ADH action.
- Symptoms: Polyuria (often > 3L/day), polydipsia, dilute urine (Osm < 200 mOsm/kg, SG < 1.005), potential hypernatremia.
- Central DI: ↓ADH secretion. Dx: Water deprivation test followed by Desmopressin (Urine Osm ↑ by >50%). Tx: Desmopressin.
- Nephrogenic DI: Kidney unresponsive to ADH. Dx: No/minimal Urine Osm response to Desmopressin. Tx: Thiazides, Amiloride.
- SIADH (Syndrome of Inappropriate ADH): "Soaked Inside" - Excessive ADH effect. 📌 Soaked Inside.
- Symptoms: Euvolemic hyponatremia (Na+ < 135 mEq/L), inappropriately concentrated urine (Osm > 100 mOsm/kg & often > serum Osm), ↓serum Osm (< 275 mOsm/kg).
- Tx: Fluid restriction, demeclocycline, vaptans. Correct Na+ slowly.
| Feature | Central DI | SIADH |
|---|---|---|
| Serum Na+ | ↑ or Normal | ↓ ( <135 mEq/L) |
| Serum Osmolality | ↑ ( >295 mOsm/kg) | ↓ ( <275 mOsm/kg) |
| Urine Osmolality | ↓ ( <200 mOsm/kg) | ↑ ( >100 mOsm/kg, often > serum Osm) |
⭐ In SIADH, urine sodium is typically elevated (e.g., > 40 mEq/L) despite hyponatremia, reflecting euvolemic or slightly hypervolemic state with ongoing natriuresis.
High‑Yield Points - ⚡ Biggest Takeaways
- Craniopharyngioma: Most common pediatric suprasellar tumor; causes growth failure, bitemporal hemianopia.
- GH Deficiency: Presents as short stature, delayed bone age; GH stimulation tests are diagnostic.
- Central Diabetes Insipidus: Features polyuria, polydipsia, hypernatremia; use water deprivation test.
- SIADH: Causes euvolemic/hypervolemic hyponatremia and concentrated urine.
- Cushing's Disease: Leads to growth failure, central obesity, hypertension from pituitary ACTH.
- Congenital Hypopituitarism: Neonatal signs include hypoglycemia, micropenis, prolonged jaundice.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

