DKA - Sugar Storm Saga
Diabetic Ketoacidosis: life-threatening. Pathophysiology: ↓Insulin, ↑counter-regulatory hormones → hyperglycemia, ketogenesis, acidosis. Clinical Features:
- Kussmaul breathing (deep, rapid)
- Dehydration (tachycardia, ↓turgor)
- Abdominal pain, vomiting
- Altered sensorium, fruity breath 📌 Dehydration, Ketones/Kussmaul, Acidosis/Abdominal pain. Diagnostic Criteria:
- Blood glucose >200 mg/dL
- Ketonemia (β-hydroxybutyrate ≥3 mmol/L) / Ketonuria (≥2+)
- Acidosis: Venous pH <7.3 or HCO3 <15 mEq/L Management:
- Fluids: Isotonic saline (0.9% NaCl) 10-20 mL/kg bolus.
- Insulin: IV 0.05-0.1 U/kg/hr (after initial fluids).
- Potassium: Add to IV fluids (once U.O. & K+ <5.5 mEq/L).
Monitoring: Hourly glucose, neuro status. 2-4 hrly electrolytes, VBG.

⭐ Cerebral edema: critical DKA complication. Signs: headache, ↓LOC, bradycardia, HTN. Manage with mannitol (0.5-1 g/kg IV), hypertonic saline, fluid restriction.
Hypoglycemia - Low Sugar Lowdown
- Definition: Glucose: Neonates <45 mg/dL; Infants/Children <50-60 mg/dL.
- Etiology:
- Neonatal: IDM, prematurity, sepsis.
- Childhood: Hyperinsulinism, ketotic hypoglycemia, GH/cortisol↓, IEMs, ingestions.
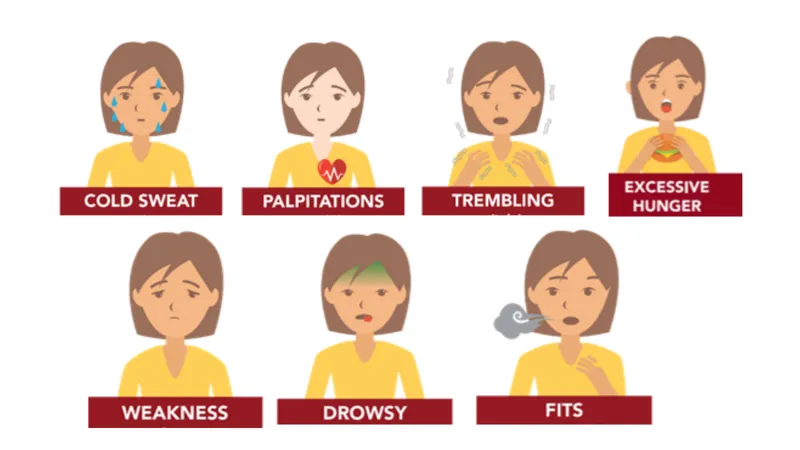
- Clinical:
- Neuroglycopenic: Seizures, lethargy, coma.
- Autonomic: Sweating, tremors, tachycardia.
- Whipple's Triad: Symptoms + Low glucose + Relief with glucose.
- Management:
- Oral glucose (if conscious).
- IV D10W 2 ml/kg bolus; then infusion.
- Glucagon IM/SC (0.03-0.1 mg/kg, max 1mg) if no IV.
- Labs: Critical samples (glucose, insulin, C-peptide, GH, cortisol, ketones, lactate) before glucose.
⭐ Key: Collect critical samples (glucose, insulin, C-peptide, etc.) before giving glucose to find cause.
Adrenal Crisis - Adrenal Alarm!
- Pathophysiology: Acute deficiency of cortisol +/- aldosterone.
- Etiology: Congenital Adrenal Hyperplasia (CAH - esp. salt-wasting), Addison's disease, abrupt steroid withdrawal, pituitary failure, stress in known adrenal insufficiency.
- Clinical Features: Shock (hypotension, tachycardia unresponsive to fluids/pressors), vomiting, abdominal pain, weakness, hypoglycemia, hyponatremia (↓Na), hyperkalemia (↑K). Hyperpigmentation (chronic).
- Diagnosis: Clinical suspicion, low cortisol, high ACTH (primary), electrolyte imbalance. ACTH stimulation test (not in emergency).
- Management: ABCs, IV Hydrocortisone (stress dose: 50-100 $mg/m^2$ or age-based), IV fluids (NS or D5NS for shock & hypoglycemia), correct electrolytes, treat underlying cause.
⭐ Typical Stress Dose of Hydrocortisone (IV/IM):
- Neonates: 25 mg
- Infants (1 month - 2 years): 25-50 mg
- Children (2-12 years): 50-100 mg
- Adolescents (>12 years): 100-150 mg
- Alternative: 50-100 $mg/m^2$ initially, then divided q6h.
Other Critical Conditions - Hormone Havoc
- Thyroid Storm:
- Precipitants: Infection, surgery, trauma (Graves').
- Features: Hyperthermia, tachycardia (out of proportion to fever), CNS agitation/coma, GI upset. Burch-Wartofsky score.
- Rx: PTU/Methimazole, Propranolol, Iodine solution (Lugol's/SSKI after antithyroid drugs), Hydrocortisone.
- Diabetes Insipidus (DI):
- Types: Central (↓ADH) vs. Nephrogenic (renal ADH resistance).
- Clinical: Polyuria, polydipsia, ↑Na+, dehydration.
- Dx: ↑Serum Osm, ↓Urine Osm (<300 mOsm/kg), Water deprivation test.
- Rx: Central: DDAVP. Nephrogenic: Thiazides, Indomethacin.
- Syndrome of Inappropriate ADH (SIADH):
- Etiology: CNS disorders, lung disease, drugs.
- Clinical: Euvolemic/hypervolemic ↓Na+, concentrated urine.
- Dx: ↓Serum Osm, ↑Urine Osm (>100 mOsm/kg), ↑Urine Na+ (>40 mEq/L). Normal renal/adrenal/thyroid function.
- Rx: Fluid restriction. Severe symptomatic ↓Na+: 3% saline. Demeclocycline, vasopressin receptor antagonists.

⭐ In DI, urine osmolality remains low (<300 mOsm/kg) after water deprivation; in psychogenic polydipsia, it increases (>600 mOsm/kg).
High‑Yield Points - ⚡ Biggest Takeaways
- DKA: IV fluids, insulin, K+ monitoring; slow correction prevents cerebral edema.
- Hypoglycemia: IV dextrose (D10W/D25W); glucagon if no IV access.
- Adrenal Crisis: Hypotension, hyponatremia, hyperkalemia; give IV hydrocortisone, fluids.
- CAH Salt-Wasting: Neonatal hyponatremia, hyperkalemia; give hydrocortisone, fludrocortisone.
- Thyroid Storm: Antithyroid drugs, β-blockers, iodine, steroids.
- SIADH: Euvolemic hyponatremia; treat with fluid restriction.
- DI (Central): Hypernatremia, polyuria; treat with desmopressin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

