Legal Framework & Initial Response - Justice for Juniors
- Key Laws & Duties:
- POCSO Act, 2012 (Sec 19): Mandatory reporting to police/Special Juvenile Police Unit (SJPU) within 24 hours. Non-reporting is punishable.
- IPC Sections: Address physical/sexual assault (e.g., 323, 325, 307, 376).
- Consent:
- Child < 18 yrs: Guardian. Emergency: Implied for life-saving measures.
- Child Welfare Committee (CWC): Inform for child's care & protection.
- 📌 CARE Mnemonic: Consent, Assess & stabilize, Report, Evidence collection.
⭐ Mandatory reporting of child sexual abuse by medical professionals under Section 19 of the POCSO Act, 2012, within 24 hours of suspicion is legally binding.
Forensic History & Clinical Exam - Uncovering Truths
- Forensic History:
- Child Interview (age-appropriate):
- Use simple, open-ended, non-leading questions (e.g., "Tell me more").
- Child-friendly, private, non-suggestive environment.
- Caregiver History:
- Interview separately. Note inconsistencies, blaming, or delayed care.
- Detailed injury mechanism and timeline.
⭐ Inconsistent or changing history provided by caregivers regarding the child's injuries is a significant red flag for non-accidental trauma.
- Child Interview (age-appropriate):
- Clinical Examination (Head-to-Toe):
- General: Assess nutritional status (failure to thrive), hygiene, emotional state, child-caregiver interaction.
- Specific Signs:
- Physical Abuse: Patterned bruises/burns, specific fractures (metaphyseal, posterior rib), injuries in varied healing stages.
- Sexual Abuse: Genital/anal trauma (tears, bruising, discharge), STIs, behavioral changes.
- Neglect: Poor growth, severe diaper rash, untreated conditions, dental caries, developmental delay. 📌 Mnemonic (adapted): History (child & caregiver, separate), Examine (head-to-toe).
Injury Patterns & Documentation - Evidence Exposed
- Bruises:
- Patterns: Grab (oval), implement (belt/loop), patterned.
- 📌 TEN-4 FACES-P: Torso, Ears, Neck in <4yo; Frenulum, Angle of jaw, Cheek, Eyelid, Subconjunctival hemorrhage; Patterned bruising.
- Burns:
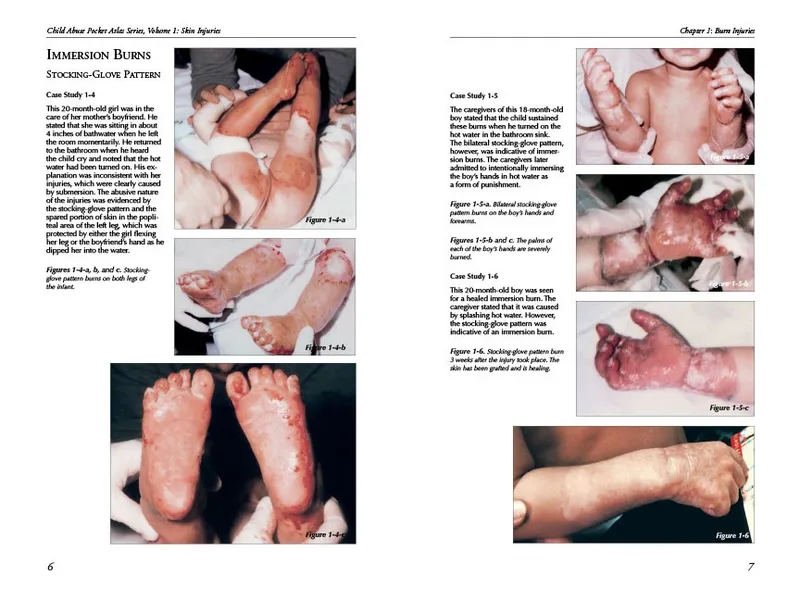
- Immersion: Stocking-glove, sharp borders.
- Cigarette: Circular, punched out.
- Splash: Irregular, drips.
- Fractures (High Specificity):
- Metaphyseal (bucket-handle/corner).
- Posterior rib fractures.
- Multiple, varied healing stages.
- Spiral in non-ambulatory infants.
- Head Injuries:
- Shaken Baby: Subdural hematoma, retinal hemorrhages.
- Bite Marks:
- Human: Oval/crescent; intercanine >3 cm (adult).
- Documentation:
- Notes, diagrams, photos (scale, light, consent).
- Notes, diagrams, photos (scale, light, consent).
⭐ Metaphyseal fractures (bucket-handle or corner fractures) and posterior rib fractures are highly specific for non-accidental injury in infants.
Specimen Collection & Chain of Custody - Securing Samples
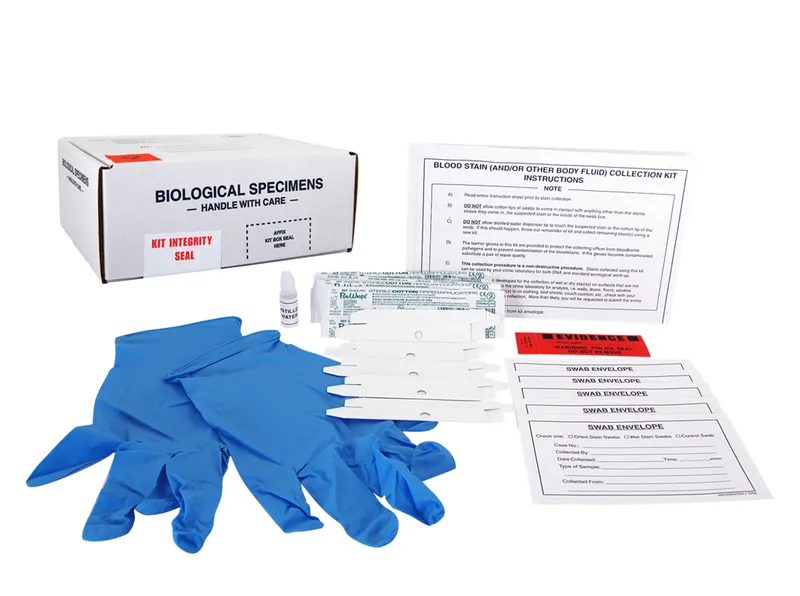
Collect samples ASAP using a POCSO kit. Maintain strict protocols for legal validity.
- Key Samples & Initial Handling:
- Blood (EDTA tubes), urine, saliva.
- Hair: Plucked, not cut, to include roots.
- Swabs: Oral, genital (vaginal sperm motility up to 72 hours), anal, bite marks (use saline-moistened swabs for DNA on skin).
- Clothing & fabrics: Air-dry thoroughly before packaging in paper bags.
- Fingernail scrapings/clippings.
- Labeling: Each sample must be meticulously labeled with: patient name/UID, date, exact time of collection, anatomical site, and collector's name/signature.
- Preservation: Generally, refrigerate (do not freeze) biological samples. Use specific transport media as per kit instructions.
- Chain of Custody: An unbroken, documented record of every individual handling the evidence from collection to lab analysis. 📌 SEALED: Samples collected, Ensure correct labeling, Authority informed, Log maintained, Evidence secured, Delivered to lab.
⭐ Maintaining an unbroken and meticulously documented chain of custody is paramount for the legal admissibility of forensic evidence in court proceedings related to child abuse and neglect cases under Indian law (e.g., POCSO Act).
High-Yield Points - ⚡ Biggest Takeaways
- Maintain meticulous chain of custody for all forensic evidence.
- Photographic evidence: Use overall, midrange, close-up views with a scale.
- Skeletal survey is key for suspected abuse in children < 2 years.
- Use POCSO kits for sexual assault; note swab collection times (e.g., 72-120 hours).
- Ensure detailed, objective documentation with body diagrams; avoid biased language.
- Bruise dating is unreliable; describe appearance, not age.
- Mandatory reporting under POCSO Act is essential for suspected abuse.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

