Definition & Thresholds - Hypertensive Hurdles
- Hypertension: BP ≥95th percentile for age, sex, height (on ≥3 occasions).
- BP Categories:
- Normal: <90th percentile.
- Prehypertension: 90th to <95th percentile OR BP >120/80 mmHg.
- Stage 1 HTN: ≥95th percentile to ≤(99th percentile + 5 mmHg).
- Stage 2 HTN: >(99th percentile + 5 mmHg).
⭐ Children <6 yrs or Stage 2 HTN: suspect secondary causes.
- Accurate Measurement:
- Correct cuff: bladder width ~40% arm circumference, length 80-100%.
- Calm child; average ≥3 readings on separate occasions.

Etiology & Red Flags - Root Cause Roundup
Primary (Essential) HTN: Prevalence ↑ with age; common in adolescents. Secondary HTN: More common in younger children, especially <6-10 years.
Common Causes of Secondary HTN:
- Renal (Most common overall): Parenchymal disease (e.g., glomerulonephritis, reflux nephropathy), renovascular disease.
- Coarctation of Aorta.
- Endocrine: Pheochromocytoma, CAH, hyperthyroidism, Cushing's syndrome.
- Drugs: Corticosteroids, NSAIDs, OCPs, sympathomimetics.
- Neurologic (e.g., ↑ICP), Genetic syndromes (e.g., Turner, Williams).
Common Causes by Age Group:
| Age Group | Common Causes |
|---|---|
| Neonate | Renal artery/vein thrombosis/stenosis, Coarctation, BPD |
| Infant | Renal (parenchymal/artery disease), Coarctation |
| Child (1-10y) | Renal (parenchymal/renovascular), Coarctation |
| Adolescent | Primary HTN, Renal (parenchymal disease), Drugs (OCPs) |
- Age <6 years (especially <3 years).
- Stage 2 HTN, symptomatic HTN, or acute severe rise.
- Electrolyte imbalance (e.g., hypokalemia).
- Physical findings suggestive of underlying cause (e.g., abdominal bruit, delayed femoral pulses, virilization, café-au-lait spots).
- Poor response to standard antihypertensive therapy.
⭐ Renal parenchymal disease is the single most common identifiable cause of secondary hypertension in children.
Evaluation & Workup - Detective Diagnosis
- History Taking:
- Perinatal: UAC, prematurity.
- Family Hx: HTN, renal/endocrine disease.
- Meds: Steroids, NSAIDs, sympathomimetics.
- Symptoms: Headache, visual changes, epistaxis, palpitations, FTT, seizures.
- Physical Examination:
- Accurate BP: Correct cuff, 4-limb BP.
- Fundoscopy: Retinopathy.
- Palpation: Kidneys, abdominal bruits, radio-femoral delay.
- Syndromic/Endocrine features (Turner, NF1, Cushingoid).
- Initial Investigations:
- Urinalysis (proteinuria, hematuria), Culture.
- Serum: Electrolytes (K+), BUN, Creatinine, Uric acid.
- Lipid profile, Fasting glucose. TSH.
- Further Investigations (Targeted):
- Renal USG + Doppler, DMSA. Echo (LVH, coarctation).
- Endocrine: PRA, Aldosterone, Catecholamines, Cortisol. Genetic tests.
- Ambulatory BP Monitoring (ABPM):
- Indications: White coat HTN, masked HTN, nocturnal dip, drug efficacy.
⭐ A significant BP difference (>10-20 mmHg) between upper and lower limbs suggests Coarctation of the Aorta.
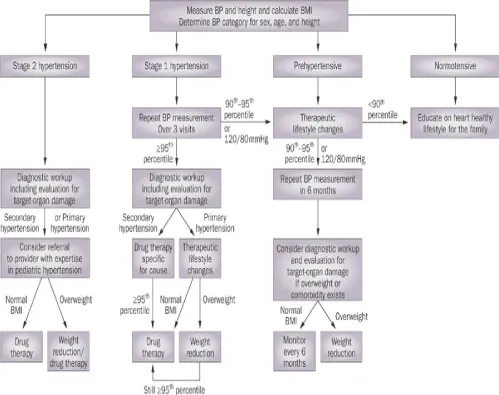
Management & Meds - Pressure Protocol
- Non-Pharmacological: Lifestyle: DASH diet, weight management, regular physical activity, salt restriction.
- Pharmacotherapy Indications: Symptomatic HTN, Stage 2 HTN, Stage 1 HTN unresponsive to LSM or with End-Organ Damage (EOD), secondary HTN, Diabetes (DM), Chronic Kidney Disease (CKD).
- Choice of Antihypertensives:
- ACE inhibitors (e.g., Enalapril; SE: cough, hyperK, angioedema)
- ARBs (e.g., Losartan; SE: similar to ACEi, less cough)
- Long-acting Calcium Channel Blockers (e.g., Amlodipine; SE: edema, flushing)
- Diuretics (e.g., Hydrochlorothiazide/HCTZ; SE: hypoK, hypoNa)
- (Beta-blockers less preferred first-line unless specific indication e.g. coarctation)
- Hypertensive Urgency/Emergency:
- Urgency: Severe HTN, no acute EOD. Emergency: Severe HTN + acute EOD.
⭐ For hypertensive emergencies, BP should be lowered gradually to avoid cerebral hypoperfusion; aim for a 25% reduction in the first 8 hours, then normalize over 24-48h.
- IV Meds (Emergency): Labetalol, Nicardipine, Sodium Nitroprusside.
High‑Yield Points - ⚡ Biggest Takeaways
- Definition: BP > 95th percentile for age, sex, height on ≥3 occasions.
- Secondary HTN: Renal parenchymal disease (most common); Coarctation of Aorta (cardiac).
- Screening: Annually from 3 years of age.
- ABPM: Gold standard to confirm diagnosis, rules out white-coat HTN.
- LVH: Most common target organ damage.
- Treatment: Lifestyle changes; ACEIs/ARBs preferred if drugs needed.
- Hypertensive Emergency: IV Labetalol or Nicardipine for rapid control.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

