RHD Pathogenesis - Strep's Delayed Attack
- Trigger: Group A β-hemolytic Streptococcus (GAS) pharyngitis (untreated/inadequately treated).
- Mechanism: Molecular mimicry.
- Bacterial M protein & carbohydrates (e.g., N-acetylglucosamine) share antigenic similarity with host tissues.
- Host antibodies produced against GAS (e.g., anti-streptolysin O, anti-DNase B) cross-react with cardiac myosin, valvular endothelium, synovium, and brain antigens.
- Timeline: Delayed, non-suppurative autoimmune sequela, typically 2-4 weeks after acute GAS infection.
- Key Pathology:
- Pancarditis: Inflammation affecting endocardium, myocardium, and pericardium.
- Aschoff bodies: Pathognomonic granulomatous lesions in myocardium; collections of lymphocytes, plasma cells, and characteristic Anitschkow cells (macrophages with caterpillar-like nuclei).

⭐ Aschoff bodies are pathognomonic for rheumatic carditis.
- Genetic predisposition influences susceptibility (certain HLA types, e.g., HLA-DR4, DR2).
Jones Criteria - Diagnostic Checklist
Diagnosis (mod/high-risk populations): 2 Major OR 1 Major + 2 Minor criteria, PLUS evidence of recent Group A Strep (GAS) infection.
- Major Criteria (📌 JONES):
- Joints: Polyarthritis (migratory)
- O (♥): Carditis (clinical/subclinical)
- Nodules: Subcutaneous (painless)
- Erythema Marginatum
- Sydenham's Chorea
- Minor Criteria (mod/high-risk):
- Monoarthralgia
- Fever (≥ 38°C)
- ↑ESR (≥30 mm/hr) OR ↑CRP (≥3.0 mg/dL)
- Prolonged PR interval (ECG)
- Essential: Evidence of Preceding GAS Infection:
- ↑ASO or Anti-DNase B titers
- Positive GAS throat culture or Rapid Antigen Detection Test (RADT)
- Recent scarlet fever (if documented)
⭐ Carditis is the most serious manifestation of acute rheumatic fever and the only one causing permanent damage.
Investigations & Valvular Lesions - Heart's Echoes
- Key Investigations:
- ↑ ASO titre, ↑ ESR/CRP (inflammation markers).
- ECG: PR prolongation, chamber enlargement signs.
- Chest X-ray: Cardiomegaly, pulmonary congestion.
- Echocardiography (2D Echo & Doppler): Gold standard. Confirms diagnosis, assesses valve damage & function.
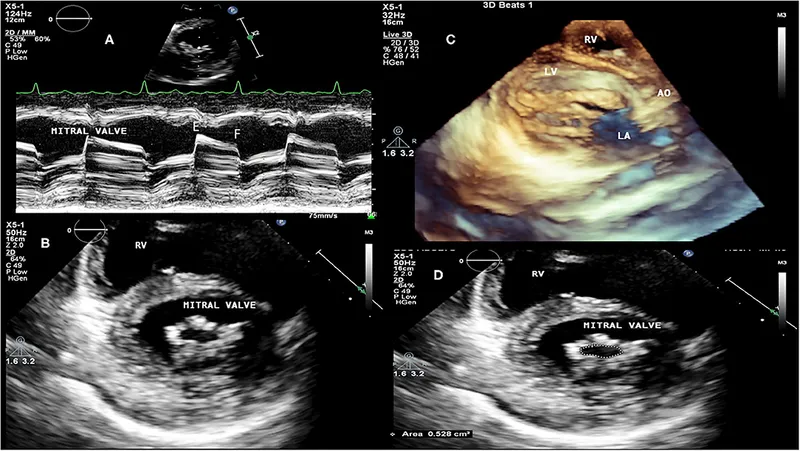
- Common Valvular Lesions (Echo findings):
- Acute Phase:
- Mitral Regurgitation (MR): Most common (📌 Carey Coombs murmur).
- Aortic Regurgitation (AR).
- Valvulitis: Annular dilatation, leaflet edema, prolapse, chordal elongation.
- Chronic Phase:
- Mitral Stenosis (MS): Most frequent. "Fish-mouth" valve.
- MR, AR, Aortic Stenosis (AS).
- Thickened, fibrosed, calcified leaflets; chordal fusion.
- Acute Phase:
⭐ Mitral valve is the most commonly affected valve in chronic RHD, typically leading to mitral stenosis.
Management & Prophylaxis - Shielding the Heart
Acute Rheumatic Fever (ARF) Management:
- Goals: Control inflammation, eradicate GAS, manage complications.
- Bed rest; Aspirin (arthritis/fever); Prednisolone (carditis).
- Eradicate GAS: Benzathine Penicillin G 1.2 MU IM (single dose, 0.6 MU if <27kg) or oral Penicillin V (10 days).
Secondary Prophylaxis (Prevent Recurrence & RHD Progression):
⭐ Secondary prophylaxis with Benzathine Penicillin G is the cornerstone of preventing RHD progression and recurrence.
- Primary: Benzathine Penicillin G 1.2 MU IM every 3-4 weeks (📌 Benzathine Prevents Going back).
- Every 3 weeks for high-risk/severe carditis.
- Alternatives (penicillin allergy): Sulfadiazine, Erythromycin.
- Duration guided by RHD severity (see flowchart).
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause of acquired heart disease in children worldwide.
- Follows Group A Streptococcal (GAS) pharyngitis; an autoimmune reaction.
- Revised Jones Criteria (major/minor) for diagnosis, needs prior GAS infection evidence.
- Pancarditis is common; mitral valve most affected (initially MR, later MS).
- Aschoff bodies (myocardial granulomas) are pathognomonic.
- Sydenham's chorea is a late, specific major neurological sign.
- Long-term penicillin prophylaxis prevents recurrence and valvular damage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

