STI Intro & Epidemiology - Adolescent Hotspots
- Sexually Transmitted Infections (STIs): Primarily spread via sexual contact; significant global health concern, especially among youth.
- Common Pathogens in Adolescents:
- Viral: Human Papillomavirus (HPV), Herpes Simplex Virus (HSV), HIV, Hepatitis B.
- Bacterial: Chlamydia trachomatis, Neisseria gonorrhoeae, Treponema pallidum (Syphilis).
- Protozoal: Trichomonas vaginalis.
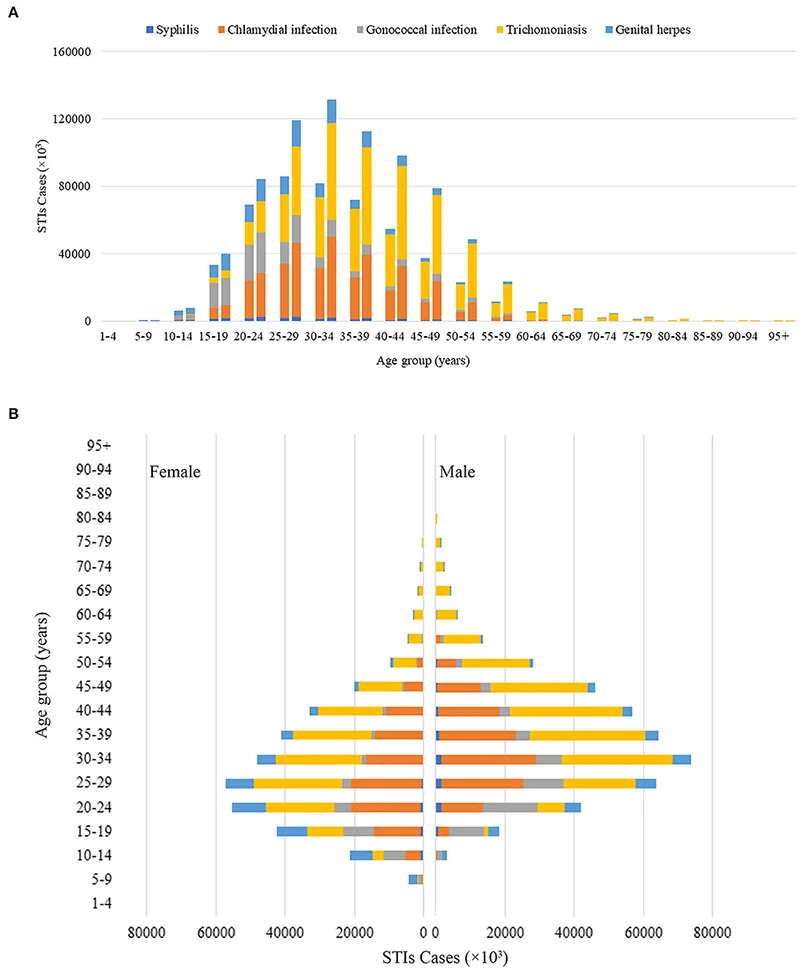
- Adolescents (15-24 years) as 'Hotspots': Experience a disproportionate burden of STIs.
- Key Risk Factors:
- Biological: Cervical ectopy in females, pubertal immune system changes.
- Behavioral: Early sexual debut, multiple/concurrent partners, inconsistent condom use, substance abuse influencing risky behavior.
- Socio-cultural: Limited access to comprehensive sexuality education & youth-friendly health services, stigma, peer pressure.
- Key Risk Factors:
⭐ Young people aged 15-24 years account for almost half of all new STIs diagnosed each year.
Genital Ulcer STIs - Painful Problems
Key causes: Herpes Genitalis & Chancroid.
-
Herpes Genitalis (HSV)
- Agent: HSV-2 > HSV-1.
- Clinical: Grouped vesicles → painful, shallow ulcers. Recurrent. Prodrome common.
- Dx: PCR (gold std), Tzanck smear (multinucleated giant cells).
- Rx: Acyclovir, Valacyclovir, Famciclovir. E.g., Acyclovir 400mg TID.
-
Chancroid (H. ducreyi)
- Agent: Haemophilus ducreyi (Gram-neg coccobacillus).
- Clinical: Soft, tender ulcer(s); ragged, undermined edges. Painful inguinal bubo (may suppurate). 📌 "Soft chancre, soft bubo".
- Dx: Gram stain ('school of fish'), culture (difficult), PCR.
- Rx: Azithromycin 1g PO (single) OR Ceftriaxone 250mg IM (single).
⭐ In Chancroid, auto-inoculation can lead to "kissing ulcers" (ulcers on opposing skin surfaces).
Discharge-Causing STIs - Drip Doctors
📌 Mnemonic: GCT (Gonorrhea, Chlamydia, Trichomoniasis)
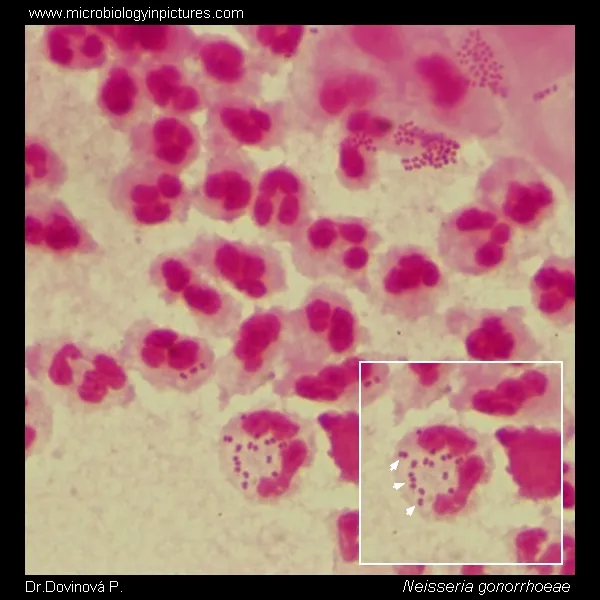
- Gonorrhea ("The Clap"):
- Agent: N. gonorrhoeae (G- diplococci).
- Sx: Men (purulent discharge, dysuria), Women (mucopurulent cervicitis, often asymptomatic).
- Tx: Ceftriaxone 500mg IM + Doxycycline.
- Chlamydia:
- Agent: C. trachomatis.
- Sx: Men (mucoid/watery discharge), Women (asymptomatic cervicitis common).
- Tx: Doxycycline OR Azithromycin 1g PO single dose.
- Trichomoniasis ("Trich"):
- Agent: T. vaginalis (protozoan).
- Sx: Women (frothy, yellow-green, malodorous discharge; "strawberry cervix"), Men (often asymptomatic).
- Tx: Metronidazole 2g PO single dose (treat partners).
- Pelvic Inflammatory Disease (PID):
- Cause: Ascending GC/CT infection.
- Sx: Lower abd pain, Cervical Motion Tenderness (CMT), adnexal tenderness.
- Complications: Infertility, ectopic pregnancy, Fitz-Hugh-Curtis syndrome.
⭐ "Strawberry cervix" (colpitis macularis) is a classic, though not always present, sign of Trichomoniasis.
Key Viral STIs & Prophylaxis - Long-Term Lurkers
- HPV (Human Papillomavirus): Oncogenic (cervical, anogenital, oropharyngeal cancers). Causes condylomata acuminata (genital warts).
- Prophylaxis: HPV vaccination (e.g., Gardasil 9, Cervarix) ideally before sexual debut (9-14 years).
- HSV (Herpes Simplex Virus): Recurrent, painful vesicles (oral/genital). Establishes lifelong latency in nerve ganglia.
- Management: Acyclovir, valacyclovir for acute episodes or suppression. No cure.
- HIV (Human Immunodeficiency Virus): Retrovirus targeting CD4+ T-lymphocytes, leading to AIDS.
- Prophylaxis: PrEP (Pre-Exposure Prophylaxis), PEP (Post-Exposure Prophylaxis), safe sex. Lifelong Antiretroviral Therapy (ART) for infected individuals.
⭐ Vertical transmission of HIV (mother-to-child) can be significantly reduced to <1% with timely maternal ART and infant prophylaxis.
- HBV (Hepatitis B Virus): Can cause acute/chronic hepatitis, cirrhosis, and Hepatocellular Carcinoma (HCC).
- Prophylaxis: HBV vaccination (universal immunization programs). Hepatitis B Immune Globulin (HBIG) + vaccine for post-exposure prophylaxis.
High‑Yield Points - ⚡ Biggest Takeaways
- Chlamydia trachomatis: Most common bacterial STI; often asymptomatic, screen sexually active females ≤25 yrs annually.
- Gonorrhea & Chlamydia: Untreated can lead to Pelvic Inflammatory Disease (PID), risking infertility and ectopic pregnancy.
- Syphilis: Characterized by painless chancre (primary); screen with VDRL/RPR, confirm with TPHA/FTA-ABS.
- Human Papillomavirus (HPV): Major cause of cervical cancer & genital warts; vaccination is crucial for prevention.
- Trichomoniasis: Presents with frothy yellow-green discharge, strawberry cervix; treat with Metronidazole (patient and partner).
- Herpes Simplex Virus (HSV-2 > HSV-1): Causes recurrent, painful genital vesicles/ulcers; managed with Acyclovir.
- Adolescent consent (usually sufficient for STI testing/treatment) and confidentiality are paramount in STI management; partner notification is key public health measure (e.g., Section 377 IPC decriminalization impact).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more