Sexual Maturation - Growing Up Guide
- Tanner Staging (SMR): Classifies puberty (stages I-V).
- Girls: Breast (Thelarche), Pubic hair (Pubarche).
- Boys: Genital development, Pubic hair (Pubarche).
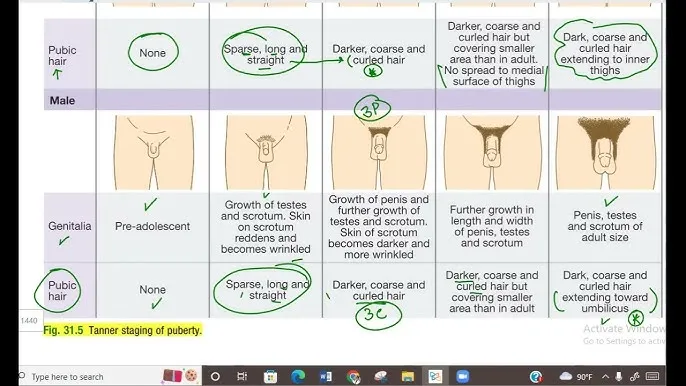
- Female Puberty (onset avg. 10-11 yrs):
- Thelarche (breast): 8-13 yrs. First sign.
- Pubarche (pubic hair): Follows/coincides.
- Peak Height Velocity (PHV): Before menarche.
- Menarche: 10-16 yrs (avg. 12.5); 2-2.5 yrs post-thelarche.
- Male Puberty (onset avg. 11-12 yrs):
- Testicular enlargement (≥4ml or >2.5cm): 9-14 yrs. First sign.
- Pubarche (pubic hair): Follows.
- Penile growth, voice deepening.
- PHV.
- Spermarche: Mid-puberty.
⭐ Sequence in girls: Thelarche → Pubarche → Peak Height Velocity → Menarche.
Adolescent Contraception - Plan Smart, Live Free
- Key Principles: Confidential, patient-centered counseling. Emphasize dual protection (contraception + STI prevention).
| Method | How it Works | Efficacy (Typical) | Adolescent Focus |
|---|---|---|---|
| LARC (IUD/Implant) | Prevents fertilization/implantation; inhibits ovulation (implant) | >99% | First-line; "fit & forget". Cu-IUD for EC. |
| OCPs | Suppress ovulation | 93% | Daily adherence crucial. Screen for contraindications (e.g., VTE, migraine with aura). |
| Condoms | Barrier; STI protection | 87% | Essential for dual protection. Counsel on consistent/correct use. |
| ECP | Delays ovulation; use ASAP (up to 72-120 hrs) | Variable | Backup, not primary. LNG or UPA (UPA more effective up to 120 hrs). |
Adolescent STIs - Dodge The Dots
Adolescents: ↑ STI risk. Confidential screening, partner notification & comprehensive care vital. Early Dx/Tx prevents PID, infertility, ectopic pregnancy.
- Screening: Sexual history-based (annual CT/GC for females ≤25y).
- Counseling: Safe sex, contraception, HPV vaccine.
- Partner Management: Expedited Partner Therapy (EPT).
Common STIs in Adolescents:
| STI | Organism | Key Symptoms | Dx | First-Line Treatment (Adolescent) |
|---|---|---|---|---|
| Chlamydia | C. trachomatis | Often Asymptomatic; discharge, dysuria | NAAT | Azithromycin 1g PO / Doxycycline 100mg BID x7d |
| Gonorrhea | N. gonorrhoeae | Purulent discharge, dysuria | NAAT | Ceftriaxone 500mg IM |
| Syphilis | T. pallidum | Chancre (1°), Rash (2°) | Serology | Benzathine Penicillin G 2.4MU IM |
| HPV | Human Papillomavirus | Warts, Cervical changes | Clinical | Topical, Cryotherapy; Vaccination |
| Trichomoniasis | T. vaginalis | Frothy yellow-green discharge, pruritus | Wet Mount | Metronidazole 2g PO single dose |
⭐ Asymptomatic Chlamydia infection is common in adolescents; annual screening for all sexually active females ≤25 years is crucial.
Psychosocial & Legal - Consent & Care
- Consent (India):
- Age of consent: 18 years. Below 18, parental/guardian consent needed.
- Exceptions: Emergencies. Mature minor concept limited.
- Confidentiality:
- Maintain unless risk of harm (self/others), abuse (POCSO), or legal order.
- Key Laws:
- POCSO Act, 2012:
- Sexual activity < 18 years = offense, consent irrelevant.
- Mandatory reporting of abuse by doctors.
- MTP Act (amended):
- < 18 years: Guardian consent for MTP.
- ≥ 18 years: Self-consent. Gestational limits (20/24 weeks).
- POCSO Act, 2012:
⭐ POCSO Act, 2012: Sexual activity < 18 years is an offense, regardless of consent; mandatory medical reporting.
High‑Yield Points - ⚡ Biggest Takeaways
- Tanner staging: key for assessing pubertal milestones, sexual maturity.
- Strict confidentiality & informed consent: crucial for adolescent sexual health services.
- Screen for prevalent STIs (e.g., HPV, Chlamydia, Gonorrhea) based on risk factors.
- Provide comprehensive contraception counseling, including emergency contraception.
- Address psychosocial aspects: body image, peer influence, and SOGI awareness.
- POCSO Act: know provisions on age of consent, mandatory reporting.
- Investigate menstrual disorders (e.g., amenorrhea, menorrhagia) promptly.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

