Brain: Cerebrovascular Disease - CNS Vascular Crises
- Acute neurological deficit from vascular cause (stroke, TIA).
- Types:
- Ischemic Stroke (~85%): Thrombotic, embolic, lacunar (small vessel disease).
- Patho: Ischemic core & surrounding penumbra.
- Hemorrhagic Stroke (~15%):
- Intracerebral (ICH): e.g., hypertensive bleed (Charcot-Bouchard microaneurysms).
- Subarachnoid (SAH): e.g., ruptured berry aneurysm ("worst headache").
- Transient Ischemic Attack (TIA): Symptoms resolve < 24h (typically < 1h), no acute infarction.
- Ischemic Stroke (~85%): Thrombotic, embolic, lacunar (small vessel disease).
- Key risk factors: Hypertension, Diabetes Mellitus, Smoking, Atrial Fibrillation.
- 📌 Mnemonic: FAST (Face, Arms, Speech, Time) for stroke recognition.
⭐ Hypertensive hemorrhages most commonly affect basal ganglia (putamen), pons, thalamus, and cerebellum due to rupture of Charcot-Bouchard microaneurysms.

Kidneys: Renal Vascular Disease - Kidney Vessel Victims
- Hypertensive Nephrosclerosis:
- Benign: Hyaline arteriolosclerosis (afferent arterioles), fibroelastic hyperplasia (interlobular arteries). Leads to fine, leathery granular cortical surface.
- Malignant: Fibrinoid necrosis of arterioles, hyperplastic arteriolosclerosis ("onion-skinning"). Petechial hemorrhages on surface ("flea-bitten kidney").
- Renal Artery Stenosis (RAS):
- Causes: Atherosclerosis (elderly males, ostial); Fibromuscular Dysplasia (FMD) (younger females, "string of beads" appearance).
- Results in: Renovascular hypertension (↑ renin), ischemic kidney atrophy.
- Thrombotic Microangiopathies (TMAs): e.g., HUS, TTP. Characterized by fibrin thrombi in glomeruli and small vessels.
- Renal Infarcts: Typically wedge-shaped, pale cortical necrosis; usually embolic origin.
⭐ In malignant hypertension, hyperplastic arteriolosclerosis manifests as concentric, laminated thickening of arteriolar walls, often described as "onion-skin" lesions.

Lungs: Pulmonary Vascular Disease - Lung Vessel Logjams
- Pulmonary Embolism (PE): Obstruction of pulmonary arteries.
- Source: >95% from DVT (Deep Vein Thrombosis).
- Risk Factors: Virchow's triad (stasis, hypercoagulability, endothelial injury). 📌 Mnemonic: SHE.
- Types: Saddle (bifurcation), lobar, segmental.
- Effects: ↑Pulmonary vascular resistance, V/Q mismatch, right heart strain. Infarction uncommon (dual supply).
- Diagnosis: CT Pulmonary Angiogram (CTPA).
- Pulmonary Hypertension (PHTN): Mean PAP > 20 mmHg at rest.
- Pathogenesis: Endothelial dysfunction, vasoconstriction, vascular remodeling.
- Consequences: RV hypertrophy → Cor pulmonale.
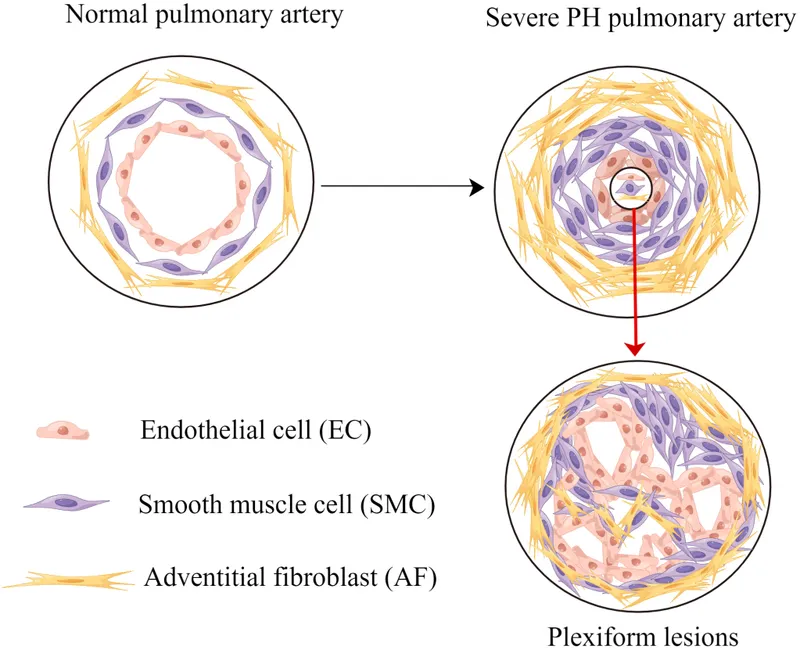
⭐ Plexiform lesions (tufts of capillary formations) are pathognomonic for severe, long-standing pulmonary hypertension, especially Group 1 PAH.
High‑Yield Points - ⚡ Biggest Takeaways
- Brain: Charcot-Bouchard microaneurysms (hypertension) → intracerebral hemorrhage; Berry aneurysms → subarachnoid hemorrhage.
- Kidney: Hyaline arteriolosclerosis (benign nephrosclerosis); hyperplastic "onion-skin" arteriolosclerosis (malignant hypertension).
- Lungs: Pulmonary hypertension shows plexiform lesions; pulmonary emboli typically from DVT.
- Liver: Budd-Chiari syndrome from hepatic vein thrombosis; portal hypertension causes esophageal varices.
- Retina: Hypertensive retinopathy: AV nicking, cotton-wool spots. Diabetic retinopathy: microaneurysms, neovascularization.
- Spleen: Gamna-Gandy bodies indicate portal hypertension and congestive splenomegaly.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

