Stent Pathology - Stent Stories & Setbacks
- Stents: Metallic scaffolds (Bare Metal Stents - BMS) or drug-coated (Drug-Eluting Stents - DES) to maintain vessel patency.
- Key Setbacks & Pathological Responses:
- Stent Thrombosis (ST):
- Acute (<24h), Subacute (1-30 days): Endothelial injury, platelet activation, flow disturbances (e.g., malapposition).
- Late (>30 days), Very Late (>1 year): More common with early-generation DES. Causes include delayed endothelialization, hypersensitivity to polymer/drug, premature dual antiplatelet therapy (DAPT) cessation. 📌 DAPT adherence is critical!
- In-Stent Restenosis (ISR):
- Predominantly with BMS. Characterized by neointimal hyperplasia (smooth muscle cell proliferation & migration, extracellular matrix deposition). Typically peaks 3-12 months post-procedure.
- DES (e.g., sirolimus, paclitaxel) significantly ↓ ISR by inhibiting this process.
- Neoatherosclerosis: Development of new atherosclerotic changes within the stented segment; a late phenomenon.
- Stent Thrombosis (ST):
- Other Issues: Stent fracture, strut malapposition, chronic inflammation, endothelial dysfunction.
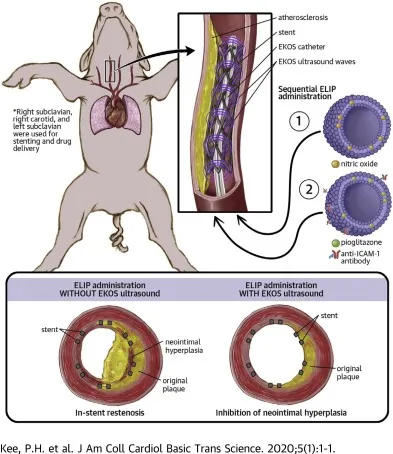
⭐ Drug-eluting stents (DES) markedly reduce in-stent restenosis by inhibiting neointimal hyperplasia but can be associated with delayed arterial healing and an increased risk of late stent thrombosis, especially if dual antiplatelet therapy is discontinued prematurely.
Graft Pathology - Bypass Blues & Boons
- Graft Types:
- Autografts: Saphenous Vein (SVG), Internal Mammary Artery (IMA - best patency).
- Synthetic: PTFE, Dacron (for larger vessels).
- Graft Failure Timeline & Causes (📌 Mnemonic: TI A - Thrombosis, Intimal Hyperplasia, Atherosclerosis):
- Early (<1 month): Thrombosis (most common).
- Causes: Technical error, poor runoff, hypercoagulability.
- Intermediate (1 month - 2 years): Intimal Hyperplasia (IH).
- Smooth Muscle Cell (SMC) proliferation & Extracellular Matrix (ECM) deposition, esp. at anastomoses in vein grafts.
- Pathogenesis: Endothelial injury → growth factors (PDGF, TGF-β) → SMC migration/proliferation.
⭐ Intimal hyperplasia is the primary cause of saphenous vein graft stenosis between 1 month and 2 years post-surgery.
- Late (>2 years): Atherosclerosis (neoatherosclerosis in vein grafts).
- Aneurysmal dilatation (common in synthetic grafts).
- Early (<1 month): Thrombosis (most common).
- Factors Improving Patency (Boons):
- Arterial grafts (IMA > SVG).
- Good distal runoff.
- Antiplatelet therapy.

General Intervention Pathology - Procedure Perils & Pathways
- Initial Insult:
- Endothelial denudation exposes subendothelial matrix.
- Acute Complications (<30 days):
- Thrombosis: Platelet aggregation, fibrin mesh; critical early failure.
- Dissection: Iatrogenic vessel wall tear.
- Embolization: Distal debris (plaque, thrombus).
- Hemorrhage/Hematoma: Access site or rupture.
- Subacute/Chronic Complications (>30 days):
- Neointimal Hyperplasia (NIH): Key to restenosis.
- Smooth muscle cell (SMC) migration/proliferation.
- Extracellular matrix (ECM) deposition.
- Causes luminal narrowing.
- Restenosis: Significant luminal reduction post-procedure.
- Stent Issues:
- Stent thrombosis (late/very late with DES).
- Strut fracture, malapposition.
- Hypersensitivity (DES polymer/drug).
- Aneurysm/Pseudoaneurysm: At injury/anastomotic site.
- Infection: Graft/stent; often indolent.
- Neointimal Hyperplasia (NIH): Key to restenosis.

⭐ Neointimal hyperplasia, involving smooth muscle cell proliferation and matrix deposition, is the main driver of in-stent restenosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Restenosis, primarily due to neointimal hyperplasia (smooth muscle cell proliferation), is the main long-term complication post-angioplasty/stenting.
- Drug-eluting stents (DES) significantly ↓ restenosis by inhibiting neointimal hyperplasia.
- Stent thrombosis, though rare, is life-threatening, often linked to premature antiplatelet therapy discontinuation.
- In-stent restenosis (ISR) with DES can involve neoatherosclerosis as a late mechanism.
- Bypass graft failure mechanisms vary: early thrombosis, intermediate intimal hyperplasia, and late atherosclerosis.
- Endothelial injury during intervention is the key trigger for many adverse vascular responses, including thrombosis and restenosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

