Aneurysms Basics - Ballooning Blood Vessels
- Definition: Permanent, localized abnormal dilation of blood vessel or heart.
- Classification:
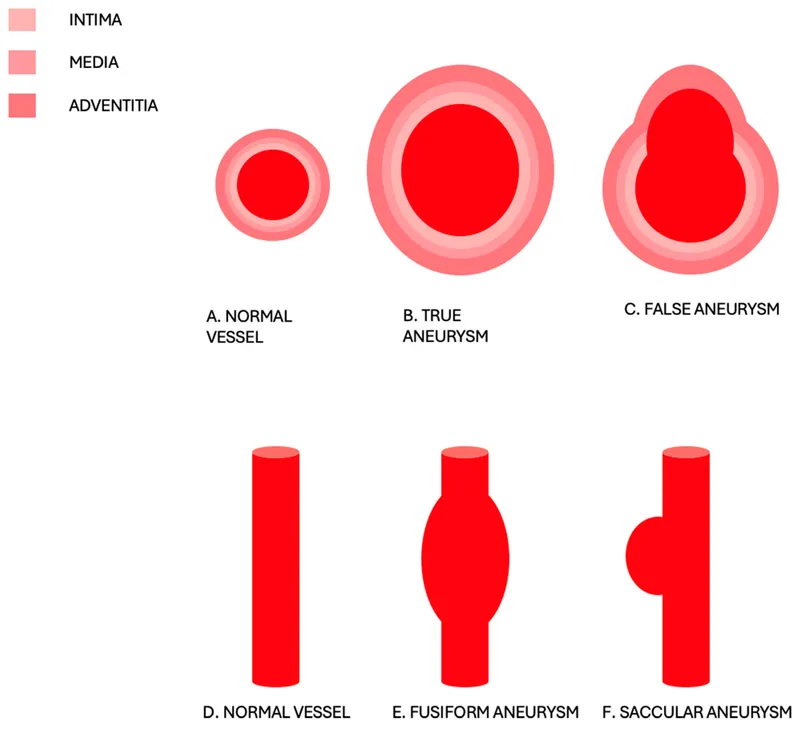
- True: All 3 wall layers (intima, media, adventitia) or thinned heart wall involved.
- E.g., Atherosclerotic, congenital, syphilitic, ventricular.
- False (Pseudoaneurysm): Wall defect → extravascular hematoma; outer wall is compressed perivascular tissue.
- E.g., Post-MI rupture (contained), anastomotic site leak.
- True: All 3 wall layers (intima, media, adventitia) or thinned heart wall involved.
- Shapes:
- Saccular: Spherical outpouching (e.g., berry).
- Fusiform: Diffuse, circumferential dilation.
- Pathogenesis: Weakened wall + ↑stress.
- Intrinsic: Marfan (FBN1), Loeys-Dietz (TGF-βR), Ehlers-Danlos (collagen).
- Acquired: Atherosclerosis (commonest), HTN, syphilis, trauma, mycotic infections.
⭐ Laplace’s Law ($T \propto P \times r / w$): ↑radius ($r$) → ↑wall tension ($T$) → ↑rupture risk.
Key Aneurysm Types - Notable Nasty Nebulae
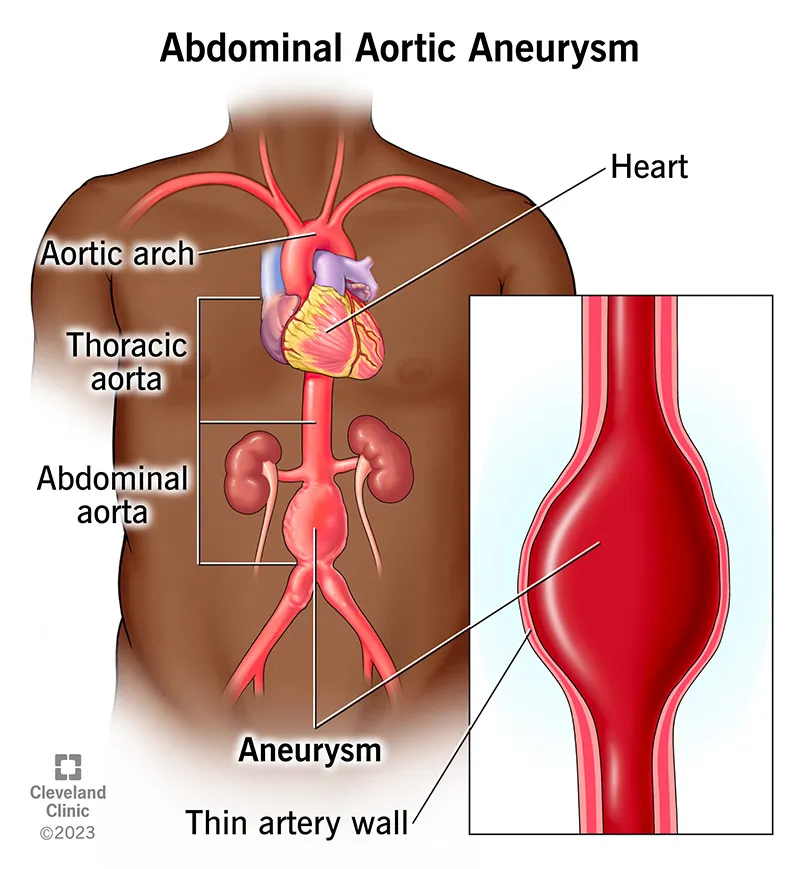
- Abdominal Aortic Aneurysm (AAA)
- Location: Infrarenal aorta (most common).
- Etiology: Atherosclerosis. Risks: Smoking, male >50y, family Hx, HTN.
- Clinical: Often asymptomatic; pulsatile abdominal mass. Rupture triad: severe pain, hypotension, pulsatile mass.
- Screen: US for men 65-75y (ever smoked). Intervention: >5.5 cm or rapid growth (>0.5 cm/6mo).
- Thoracic Aortic Aneurysm (TAA)
- Etiology: HTN (descending), cystic medial degeneration (ascending; Marfan, Ehlers-Danlos), atherosclerosis, syphilis (obliterative endarteritis → tree-bark aorta).
- Clinical: Chest/back pain, dyspnea, cough, dysphagia, hoarseness (recurrent laryngeal nerve).
- Berry (Saccular) Aneurysm
- Location: Circle of Willis, arterial bifurcations (e.g., AComA). 📌 Berries hang in Circles.
- Assoc: ADPKD, Ehlers-Danlos IV, Marfan syndrome.
- Rupture → Subarachnoid Hemorrhage (SAH) - "thunderclap headache".
⭐ Most common cause of spontaneous (non-traumatic) subarachnoid hemorrhage.
- Mycotic Aneurysm
- Definition: Localized arterial dilation from vessel wall infection (bacterial/fungal).
- Pathogenesis: Septic emboli (e.g., Infective Endocarditis), Salmonella in atheromatous plaques.
Aortic Dissection - The Great Divide
- Patho: Intimal tear → blood dissects into aortic media → false lumen formation.
- Risks: Hypertension (>70%, primary), Marfan/Ehlers-Danlos syndromes, bicuspid aortic valve, cocaine, trauma, pregnancy.
- Clinical: Sudden, severe "tearing" or "ripping" chest/back pain (often interscapular). Asymmetric BP/pulses. Neurological deficits.
- Dx: CT Angiography (CTA) is gold standard. CXR may show widened mediastinum.

- Rx:
- Immediate BP & HR control (IV β-blockers: e.g., labetalol, esmolol; target SBP 100-120 mmHg, HR <60 bpm).
- Vasodilators (e.g., nitroprusside) after β-blockade if SBP remains high.
⭐ Hypertension is the single most important modifiable risk factor for aortic dissection.
- Classification (Stanford):
- Type A: Involves ascending aorta. Surgical emergency.
- Type B: Descending aorta only. Medical management if uncomplicated.
- (DeBakey Classification):
- Type I: Ascending aorta, arch, & descending.
- Type II: Ascending aorta only.
- Type III: Descending aorta only (IIIa thoracic, IIIb thoracoabdominal).
Clinical Approach - Spot, Sort, Solve
- Spot (Suspect):
- Aneurysm: Often silent; pulsatile abdominal mass (AAA); rupture → severe pain, shock.
- Dissection: Sudden, severe tearing chest/back pain; unequal pulses/BP; neuro deficits.
- Sort (Diagnose):
- Imaging: CTA (gold standard for both); US (AAA screen); TEE (dissection, if unstable).
- Aneurysm: Size & location critical.
- Dissection: Stanford A (ascending aorta) vs B (descending).
- Solve (Manage):
- Priorities: Airway, Breathing, Circulation (ABCs); IV access.
- General: Aggressive BP control (target SBP 100-120 mmHg in dissection).
- Specifics: See flowchart for key decisions.
⭐ Aortic dissection: Immediate goal is ↓dP/dt & ↓BP; IV beta-blockers (e.g., Labetalol) first-line, target HR <60 bpm.
High‑Yield Points - ⚡ Biggest Takeaways
- AAA, most common, linked to atherosclerosis; typically infrarenal, rupture risk ↑ with size.
- Syphilitic aneurysms: ascending aorta, vasa vasorum damage, "tree barking" appearance.
- Berry aneurysms (Circle of Willis): associated with ADPKD, Ehlers-Danlos; risk SAH.
- Aortic dissection: intimal tear, blood splits media; hypertension is the major risk.
- Marfan & Ehlers-Danlos predispose via cystic medial degeneration (weakened media).
- Stanford Type A (ascending aorta) is surgical emergency; Type B (descending) often medical.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

