Pulmonary Embolism - Clot Commotion
Obstruction of pulmonary artery/branches, often by dislodged thrombus from deep veins (DVT).
-
Risk Factors: 📌 Virchow's Triad: SHE
- Stasis (e.g., immobilization, surgery)
- Hypercoagulability (e.g., OCPs, malignancy, genetic)
- Endothelial injury (e.g., trauma, surgery)
-
Types of Emboli: Thrombus (>95%), fat, air, amniotic fluid, tumor cells, septic emboli.
-
Pathophysiology: ↑Dead space → V/Q mismatch; hypoxemia; ↑Pulmonary Vascular Resistance (PVR) → right ventricular strain.
-
Clinical Features: Sudden onset dyspnea, pleuritic chest pain, hemoptysis, tachypnea, tachycardia, syncope (massive PE).
-
Diagnosis:
- Clinical probability: Wells score, PERC rule.
- D-dimer: High sensitivity, low specificity.
- CT Pulmonary Angiography (CTPA): Gold standard.
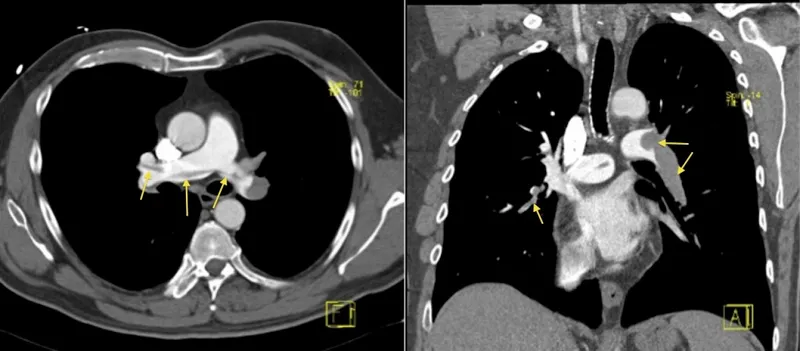
- V/Q Scan: If CTPA contraindicated/inconclusive.
- ECG: S1Q3T3 pattern (classic but uncommon), sinus tachycardia, RBBB.
- Echocardiogram: RV dysfunction, McConnell's sign.
-
Management:
- Anticoagulation: LMWH/UFH, then DOACs/Warfarin.
- Thrombolysis (e.g., alteplase): For massive PE (hypotension).
- Embolectomy (catheter/surgical): For massive PE if thrombolysis fails/contraindicated.
-
Complications: Chronic Thromboembolic Pulmonary Hypertension (CTEPH), right heart failure, death.
⭐ A normal D-dimer has a high negative predictive value to rule out PE in low-probability patients.
Pulmonary Hypertension - Pressure Overload
- Definition: Mean Pulmonary Arterial Pressure (mPAP) >20 mmHg at rest (2022 ESC/ERS).
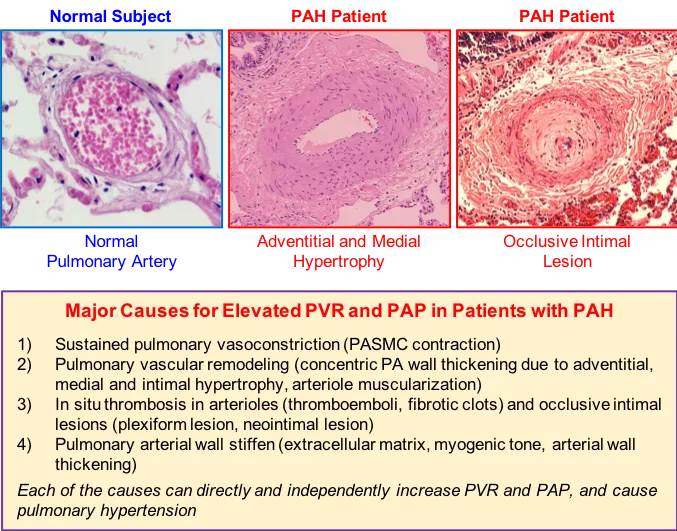
- Pathophysiology: Vasoconstriction, vascular remodeling (e.g., intimal fibrosis, medial hypertrophy, plexiform lesions), microthrombosis, inflammation.
- WHO Classification (📌 Mnemonic: PAH, Left heart, Lung disease, CTEPH, Others - PLLCO)
Group Type Examples 1 PAH Idiopathic, heritable, drug, CTD 2 PH due to Left Heart Disease LHD (LV dysfxn, valvular) 3 PH due to Lung Diseases/Hypoxia Lung disease/hypoxia (COPD, ILD, sleep apnea) 4 CTEPH CTEPH 5 PH with Unclear Multifactorial Mechanisms Unclear (hematologic, systemic, metabolic) - Clinical Features: Dyspnea, fatigue, chest pain, syncope; RHF signs (edema, JVD, loud P2, RV heave).
- Investigations:
- Echocardiography: Initial screening (estimates PASP, RV size/function).
- Right Heart Catheterization (RHC): Gold standard (diagnosis, severity: mPAP, PVR >3 Wood units for pre-capillary PH; vasoreactivity testing).
- Management Principles:
- Treat underlying cause.
- General measures: Diuretics, oxygen, anticoagulation (select groups).
- Targeted (Group 1 PAH): Prostanoids (epoprostenol), ERAs (bosentan), PDE5 inhibitors (sildenafil), sGC stimulators (riociguat).
⭐ Plexiform lesions are characteristic histopathological findings in advanced Group 1 Pulmonary Arterial Hypertension (PAH), indicating severe vascular remodeling.
Pulmonary Edema - Fluid Fiasco
- Definition: Abnormal accumulation of excess extravascular fluid in lung interstitium & alveoli.
- Pathophysiology: Imbalance in Starling forces: $J_v = L_p S ([P_c - P_i] - \sigma[\pi_c - \pi_i])$.
- Clinical Features: Dyspnea, orthopnea (esp. cardiogenic), pink frothy sputum.
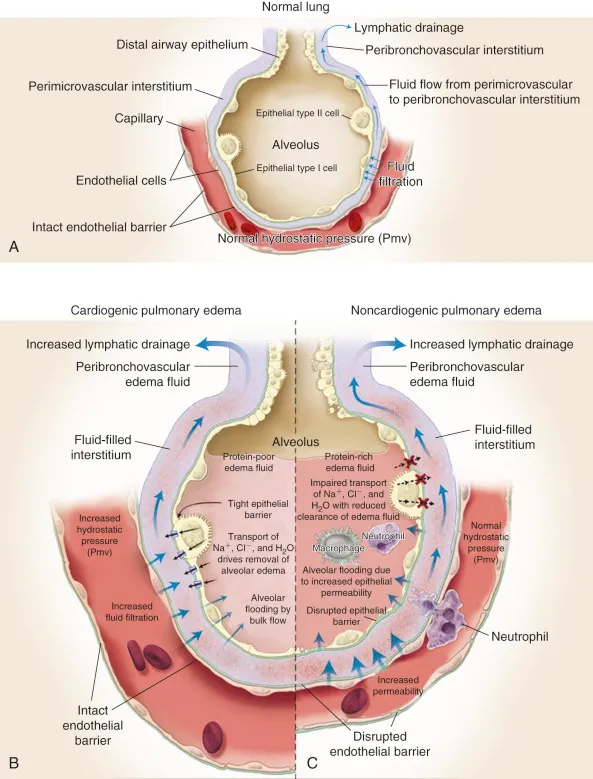
| Feature | Cardiogenic Edema | Non-cardiogenic Edema |
|---|---|---|
| Primary Defect | ↑ $P_c$ (Pulm. Cap. Hydrostatic Pressure) | ↑ Capillary Permeability / ↓ $\pi_c$ (Plasma Oncotic Pressure) / Lymphatic Obstruction |
| Causes | LV failure, mitral stenosis | ARDS, sepsis, trauma, pancreatitis, drug reactions, HAPE (📌 Think ALI causes) |
| PCWP | >18 mmHg (↑) | Normal / Low |
| Edema Fluid | Low protein | High protein (due to ↑ permeability) |
| Chest X-ray | Batwing, Kerley B lines, cardiomegaly, pleural effusion | Patchy/diffuse infiltrates, normal heart size (initially) |
High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary embolism (PE): Most commonly from DVT; Lines of Zahn indicate pre-mortem clot formation.
- Pulmonary hypertension (PHTN): Defined as mean pulmonary arterial pressure >20 mmHg; BMPR2 gene mutation is often implicated in primary PHTN.
- Common causes of secondary PHTN include COPD, mitral stenosis, recurrent PEs, and connective tissue diseases.
- Plexiform lesions in pulmonary arteries are pathognomonic for severe, irreversible PHTN.
- Fat embolism syndrome: Classic triad of respiratory distress, neurological symptoms, and petechial rash, typically after long bone fractures.
- Amniotic fluid embolism: Characterized by sudden DIC, profound shock, and severe hypoxia during or immediately post-delivery; high mortality rate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

