ILD Basics - The Lung's Labyrinth
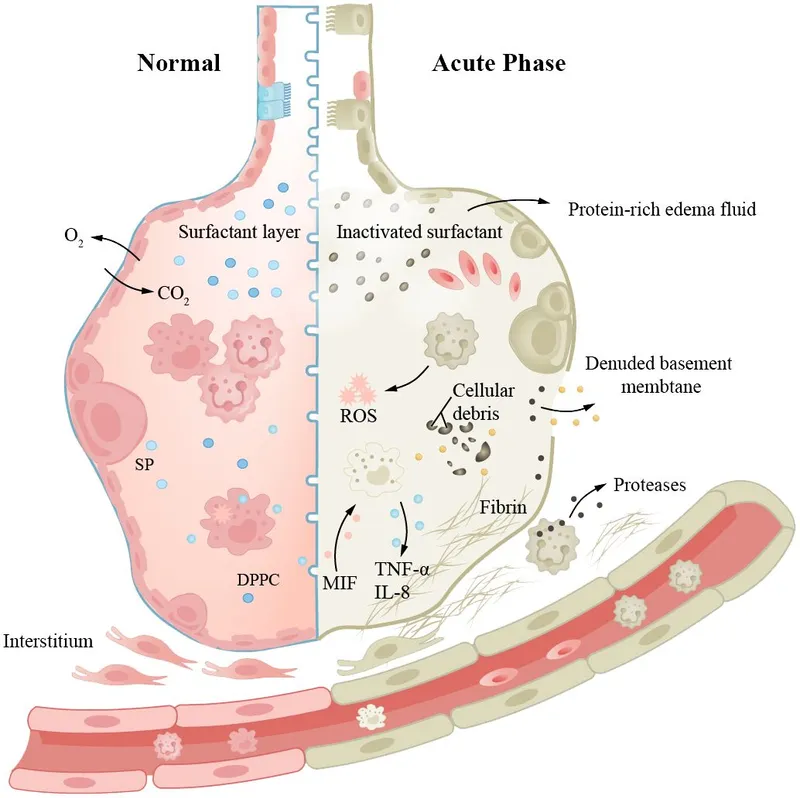
- Definition: Diverse group of diffuse parenchymal lung diseases (DPLDs) primarily affecting the interstitium - the tissue space between alveolar epithelium and capillary endothelium, including basement membrane, perivascular, and perilymphatic tissues.
- Common Pathological Features: Varying degrees of inflammation and fibrosis of the pulmonary interstitium.
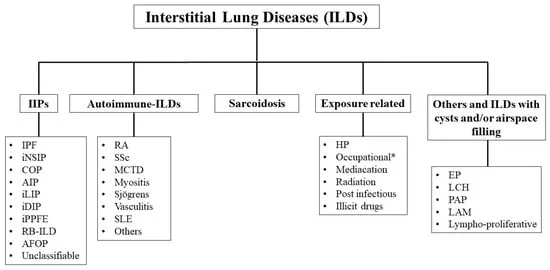
- Major Categories:
- Idiopathic Interstitial Pneumonias (IIPs) (e.g., IPF)
- ILD of known cause (e.g., CTD, drug, occupational pneumoconioses)
- Granulomatous ILDs (e.g., Sarcoidosis, Hypersensitivity Pneumonitis)
- Other rare ILDs
⭐ Idiopathic Pulmonary Fibrosis (IPF) is the most common and has the worst prognosis among IIPs.
IIPs Deep Dive - Mysterious Mists
| IIP | Key Histology | HRCT Findings | Prognosis |
|---|---|---|---|
| IPF (UIP) | Temporal & spatial heterogeneity, fibroblastic foci | Basal, subpleural predominant honeycombing, traction bronchiectasis | Poor (median survival 2-5 yrs) |
| NSIP | Cellular/fibrotic (temporally uniform inflammation/fibrosis) | Bilateral, symmetric GGO; fine reticulation; subpleural sparing | Variable, better than IPF |
| COP (BOOP) | Masson bodies (intraluminal organizing PNA plugs) | Patchy, peripheral/peribronchial consolidations; GGOs | Good, steroid-responsive |
| AIP (Hamman-Rich) | Diffuse Alveolar Damage (DAD) - hyaline membranes | Diffuse, bilateral GGOs and/or consolidations, rapid progression | Very poor, high acute mortality |
⭐ Cryptogenic Organizing Pneumonia (COP) often presents with flu-like symptoms and shows excellent response to corticosteroids.
Secondary ILDs - Environmental & Autoimmune Invaders
- Pneumoconioses: Chronic mineral dust inhalation.
Disease Agent Occupation Key Pathology CXR/CT Finding Silicosis Silica Mining, Sandblasting Silicotic nodules, ↑TB risk Apical "rock-like" nodules, Eggshell calcification (hilar) CWP Coal Coal mining Coal macules, Progressive Massive Fibrosis (PMF) - Asbestosis Asbestos Shipbuilding, Insulation Asbestos bodies, Pleural plaques Basal fibrosis, ↑Mesothelioma risk Berylliosis Beryllium Aerospace, Electronics Non-caseating granulomas Hilar lymphadenopathy 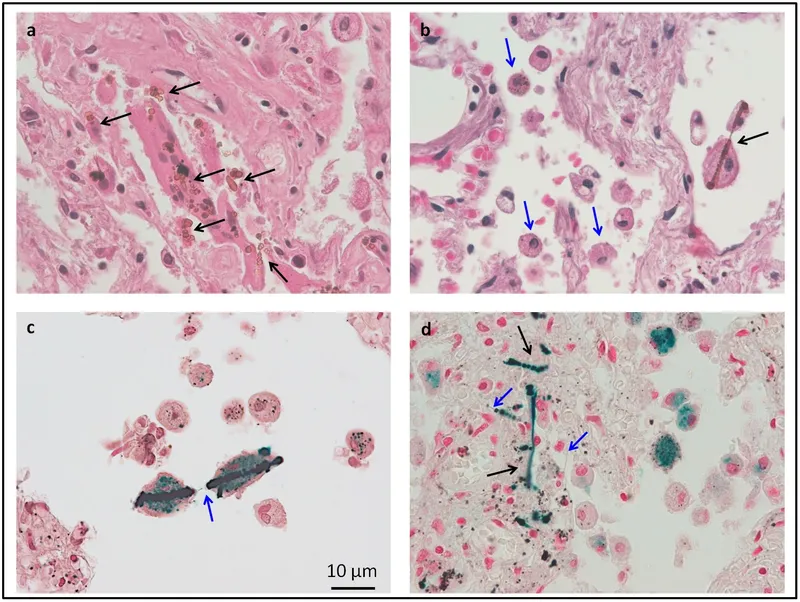
- Hypersensitivity Pneumonitis (HP): Immune reaction to inhaled organic antigens (Farmer's, Bird fancier's lung).
- Acute: Neutrophils.
- Chronic: Lymphocytes, granulomas, fibrosis.
- Drug-induced ILD: Amiodarone, Bleomycin, Methotrexate. Patterns: pneumonitis, fibrosis.
- ILD in Connective Tissue Diseases (CTD): RA, Scleroderma (NSIP common), SLE.
⭐ Asbestosis: ↑ risk of lung cancer (esp. smokers) & primary cause of mesothelioma.
Sarcoidosis Focus - Granuloma Galaxy
- Definition: Multisystem granulomatous disorder of unknown etiology, characterized by immune cell accumulation.
- Pathology: Hallmark is non-caseating epithelioid granulomas.
- May contain Schaumann bodies (laminated calcium concretions) or Asteroid bodies (stellate inclusions).

- May contain Schaumann bodies (laminated calcium concretions) or Asteroid bodies (stellate inclusions).
- Pulmonary: Bilateral hilar lymphadenopathy (BHL) is classic. Also, pulmonary infiltrates, fibrosis.
- Lofgren's syndrome: Acute BHL, erythema nodosum, fever, arthralgia.
- Extrapulmonary: Skin (erythema nodosum, lupus pernio), eyes (uveitis), heart, nervous system.
- Labs: Elevated serum Angiotensin-Converting Enzyme (ACE) levels (↑~60% cases), hypercalcemia.
⭐ Bilateral hilar lymphadenopathy (BHL) is the most common radiographic finding in pulmonary sarcoidosis.
ILD Diagnosis - Detective's Toolkit
- Clinical: Progressive dyspnea, non-productive cough, bibasilar crackles.
- PFTs: Restrictive pattern: ↓TLC, ↓FVC, ↓DLCO; FEV1/FVC normal or ↑.
- HRCT Chest: Key! Patterns: Ground-glass opacity (GGO), reticular, honeycombing (UIP), traction bronchiectasis.

- Biopsy: Transbronchial, cryobiopsy, or surgical (SLB) if diagnosis uncertain. Multidisciplinary discussion (MDD) vital.
⭐ Honeycombing on HRCT, often bibasilar and subpleural, is a hallmark of Usual Interstitial Pneumonia (UIP) pattern and indicates advanced fibrosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Idiopathic Pulmonary Fibrosis (IPF) typically presents with a UIP pattern on histology and honeycomb lung on HRCT; prognosis is poor.
- Sarcoidosis is characterized by non-caseating granulomas, bilateral hilar lymphadenopathy, and often elevated serum ACE levels.
- Hypersensitivity Pneumonitis results from an immune reaction to inhaled organic antigens (e.g., Farmer's lung, Bird fancier's lung).
- Pneumoconioses are caused by inorganic dust inhalation; key examples include silicosis (eggshell calcification, ↑TB risk) and asbestosis (pleural plaques, ↑mesothelioma risk).
- Many drugs can induce ILD, notably amiodarone, bleomycin, and methotrexate.
- Connective tissue diseases such as rheumatoid arthritis and scleroderma are frequently associated with ILD development.
- Smoking-related ILDs include respiratory bronchiolitis-ILD (RB-ILD) and desquamative interstitial pneumonia (DIP), primarily affecting smokers.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

