Testicular Tumors Overview & Classification - The Ball Game Basics
- Neoplasms of the testes; most common solid malignancy in men aged 15-35 years.
- Classification:
- Germ Cell Tumors (GCTs): ~95%; derived from primordial germ cells.
- Seminoma (most common GCT)
- Non-Seminomatous GCTs (NSGCTs)
- Sex Cord-Stromal Tumors (SCSTs): ~5%; arise from supportive tissues (Sertoli, Leydig cells).
- Leydig cell tumors
- Sertoli cell tumors
- Germ Cell Tumors (GCTs): ~95%; derived from primordial germ cells.
- Key Risk Factors:
- Cryptorchidism (↑ 3-5x risk; most significant).
- Family history; previous testicular GCT.
- Klinefelter syndrome; testicular dysgenesis.
⭐ Cryptorchidism is the most significant predisposing factor for testicular germ cell tumors (especially seminoma).
Germ Cell Tumors: Seminoma - The Classic Contender
- Most common testicular germ cell tumor (GCT), peak incidence 30s.
- Gross: Homogenous, tan-yellow, lobulated cut surface; no hemorrhage/necrosis typically.
- Micro: Sheets of uniform cells with clear cytoplasm & prominent nucleoli ("fried egg" appearance), separated by fibrous septa with lymphocytic infiltrate.
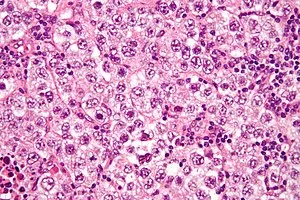
- Markers: Positive for PLAP (placental alkaline phosphatase), OCT3/4, KIT (CD117). ↑hCG in ~15% (syncytiotrophoblastic cells).
- Excellent prognosis; highly radiosensitive & chemosensitive.
⭐ Seminomas are the male GCT equivalent of ovarian dysgerminomas.
- 📌 Mnemonic: Seminoma = Sensitive (to radiation), Simple (uniform cells), Syncytiotrophoblasts (sometimes present, produce hCG).
Germ Cell Tumors: Non-Seminomatous (NSGCTs) - The Diverse Villains
- Heterogeneous group with varied differentiation and aggressive potential. More aggressive than seminomas.
- Often occur as mixed germ cell tumors.
| Tumor | Peak Age / Key Histo | Markers (↑) | Key Behavior |
|---|---|---|---|
| Embryonal Carcinoma | 20-30 yrs; hemorrhagic, pleomorphic cells, primitive glands | AFP (50%), hCG (50%) | Aggressive |
| Yolk Sac Tumor | <3 yrs (commonest); Schiller-Duval bodies | AFP (always) | Good (kids) |
| Choriocarcinoma | 20-30 yrs; cytotropho- & syncytiotrophoblasts; early hematogenous spread | hCG (always, high) | Highly Aggressive |
| Teratoma (Post-pub.) | Variable; ≥2 germ layers (e.g., cartilage, glands); All potentially malignant | Often normal | Variable |
⭐ Yolk Sac Tumors are the most common testicular tumor in infants and children (<3 years), characterized by pathognomonic Schiller-Duval bodies and consistently elevated AFP.
Sex Cord-Stromal & Other Tumors - The Specialized Players
- Leydig Cell Tumors:
- Androgen ↑ (precocious puberty in boys, gynecomastia in men).
- Reinke crystals (eosinophilic, pathognomonic cytoplasmic inclusions).
- Usually benign.
- Sertoli Cell Tumors:
- Rare; may produce estrogens.
- Form tubules/cords.
- Usually benign.
- Testicular Lymphoma:
- Most common testicular tumor in men >60 years.
- Usually Diffuse Large B-cell Lymphoma (DLBCL).
- Aggressive; often bilateral. Poor prognosis.
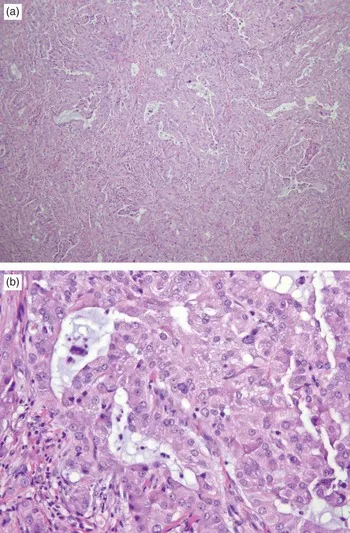
⭐ Testicular Lymphoma is the most common testicular tumor in men over 60 years, typically DLBCL.
Clinical Approach & Staging - The Diagnostic Drill
- Presentation: Typically painless testicular mass; may have dull ache/heaviness.
- Key Investigations:
- Scrotal Ultrasound: Initial imaging to confirm solid mass.
- Serum Tumor Markers (AFP, β-hCG, LDH): Baseline pre-orchiectomy. β-hCG ↑ in ~15% seminomas. Aid diagnosis, staging, prognosis, monitoring.
- Staging: AJCC TNM system; CT Chest/Abdomen/Pelvis for metastases.
⭐ Pure seminomas never produce AFP. If AFP is elevated, a non-seminomatous germ cell tumor (NSGCT) component is present.
High‑Yield Points - ⚡ Biggest Takeaways
- Germ cell tumors (GCTs) comprise 95% of cases; cryptorchidism is a key risk factor.
- Seminoma: most common GCT, radiosensitive, ↑PLAP, sometimes ↑hCG.
- Yolk Sac Tumor: most common in infants/children <3 yrs, ↑AFP, Schiller-Duval bodies.
- Choriocarcinoma: aggressive, early hematogenous spread, ↑↑hCG.
- Leydig Cell Tumor: may cause precocious puberty (androgens) or gynecomastia (estrogens).
- Teratoma: in adults malignant, in children benign; contains diverse tissues.
- Lymphoma: most common testicular malignancy in men >60 years an_bilateral_often_B-cell_type_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

