Placental Anatomy & Development - Basic Blueprint
- Dual Origin:
- Fetal: Chorion frondosum (forms villi)
- Maternal: Decidua basalis (basal plate)
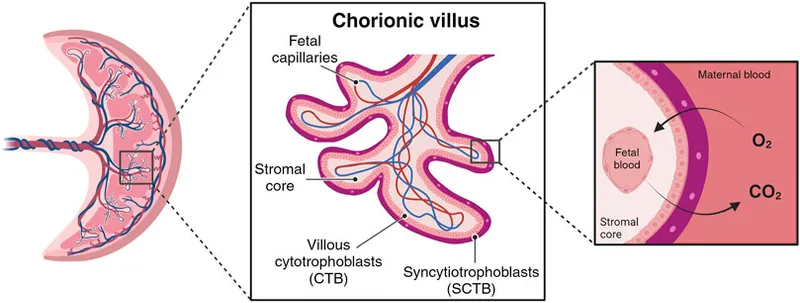
- Villous Development:
- Primary (cytotrophoblast core)
- Secondary (mesenchymal core)
- Tertiary (vascularized); stem, intermediate & terminal villi.
- Key Cells:
- Syncytiotrophoblast (outer, multinucleated, hormones)
- Cytotrophoblast (Langhans'; inner, proliferative)
- Hofbauer cells (stromal macrophages)
- Maternal Interface: Intervillous space (maternal blood); spiral artery remodeling crucial.
⭐ Nitabuch's layer: Fibrinoid zone at utero-placental junction, limits placental invasion.
Placental Infections - Pathogen Parade
- Routes: Ascending (commonest), hematogenous.
- Chorioamnionitis: Maternal (chorion/amnion neutrophils) & Fetal (funisitis - umbilical cord vasculitis) response.
- Villitis: Villi inflammation. Specific (CMV, Toxo) vs. VUE (Villitis of Unknown Etiology).
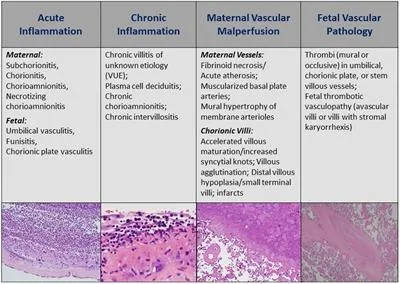
- 📌 TORCH Infections:
- Toxoplasma: Necrotizing villitis.
- Others: Syphilis (large placenta, funisitis), Listeria (microabscesses), Varicella (necrotizing villitis, inclusions), Parvo B19 (hydrops, erythroblast inclusions).
- Rubella: Mild villitis.
- CMV: Plasma cell deciduitis, owl's eye inclusions.
- HSV: Necrotizing villitis, inclusions.
⭐ Plasma cell deciduitis is highly suggestive of chronic endometritis and can be seen with certain infections like CMV.
Vascular & Implantation Disorders - Flow Failures
- Placenta Previa: Painless APH. Types: complete, partial, marginal, low-lying. Risk: prior C-section.

- Placental Abruption: Painful APH, premature separation. Concealed/revealed. Risk: HTN. Couvelaire uterus.
- Placenta Accreta Spectrum: Abnormal invasion.
Type Definition Accreta Villi attach to myometrium (no decidua) Increta Villi invade myometrium Percreta Villi penetrate serosa/adjacent organs ⭐ Prior Cesarean section is the single most important risk factor for placenta accreta spectrum disorders.
- Maternal Floor Infarct: Basal plate fibrin deposition, ↓ perfusion. IUGR, stillbirth.
- Fetal Thrombotic Vasculopathy: Fetal vessel thrombosis. Stillbirth, neuro injury.
Gestational Trophoblastic Disease - Molar Mayhem
- Hydatidiform Mole: Abnormal trophoblast proliferation.
- Complete (CM): 46,XX/XY (paternal). Diffuse villous edema ('grapes'), diffuse trophoblast hyperplasia. Markedly ↑hCG. p57KIP2 negative. Risk of choriocarcinoma ~15-20%.
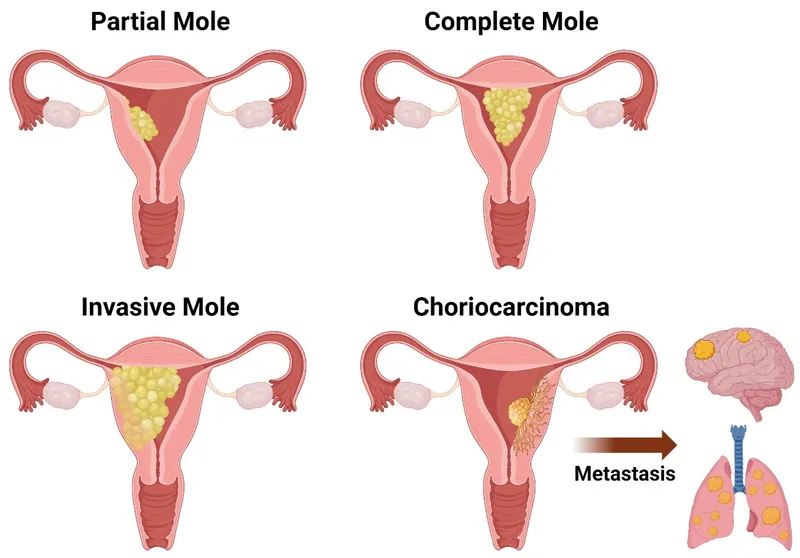
- Partial (PM): 69,XXY/XXX (triploid). Fetal parts; focal villous edema & trophoblast hyperplasia. Moderately ↑hCG. p57KIP2 positive. Risk <5%.
- Complete (CM): 46,XX/XY (paternal). Diffuse villous edema ('grapes'), diffuse trophoblast hyperplasia. Markedly ↑hCG. p57KIP2 negative. Risk of choriocarcinoma ~15-20%.
- Invasive Mole: Mole invades myometrium. Persistent ↑hCG post-evac.
- Choriocarcinoma: Malignant cyto/syncytio; NO villi. Hematogenous (lungs). Very ↑hCG.
- PSTT (Placental Site Trophoblastic Tumor): Neoplastic intermediate trophoblasts. hPL positive; low hCG.
⭐ p57KIP2: Negative in CM (no maternal genome), Positive in PM (maternal genome present).
Other Placental Pathologies - Oddball Outcomes
- Abnormal Shape/Size:
- Bilobed: Two lobes.
- Succenturiate: Accessory lobe; risk of retained products, PPH.
- Circumvallate: Rolled edges, fibrin; ↑abruption, preterm labor.
- Placenta Membranacea: Diffuse, thin placenta; accreta risk.
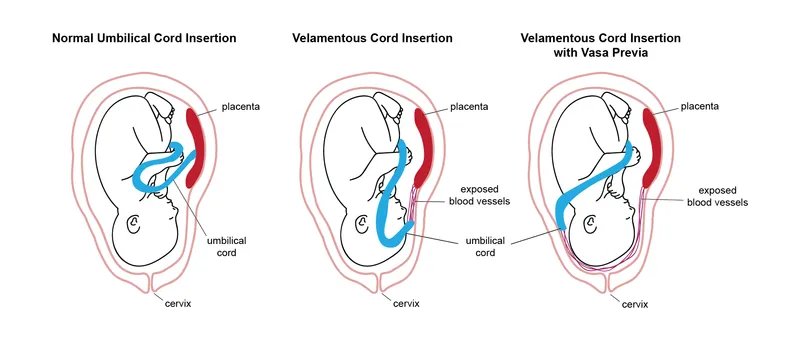
- Cord Abnormalities:
- Velamentous/Marginal Insertion: Unprotected vessels; risk of rupture, vasa previa.
- True Knots: Can impede fetal circulation, fetal demise.
- Vasa Previa: Fetal vessels overlie internal os; high fetal mortality if ruptured.
⭐ A single umbilical artery is associated with an increased risk of congenital anomalies, particularly cardiac and renal.
- Meconium Staining:
- Greenish discoloration of membranes/cord. Histo: meconium-laden macrophages in amnion/chorion.
- Twin Placenta:
- Determine chorionicity (mono/di) & amnionicity.
- TTTS (Twin-Twin Transfusion Syndrome): Monochorionic; donor anemic, oligohydramnios; recipient polycythemic, polyhydramnios.
High‑Yield Points - ⚡ Biggest Takeaways
- Placenta accreta spectrum: Abnormal adherence (accreta, increta, percreta); prior C-section is a major risk.
- Abruptio placentae: Premature separation; painful bleeding, fetal distress, risk of DIC.
- Placenta previa: Low implantation; painless 3rd-trimester bleeding.
- Chorioamnionitis: Ascending infection; neutrophils in membranes, fetal tachycardia.
- Complete mole: 46,XX (paternal), no fetus, diffuse villous edema, markedly ↑ hCG, ↑ choriocarcinoma risk.
- Partial mole: Triploid (69,XXX/XXY), fetus present, focal edema, moderately ↑ hCG.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

