GTD Spectrum - Trophoblast Tales
Gestational Trophoblastic Disease (GTD) encompasses a spectrum of disorders arising from abnormal proliferation of placental trophoblasts. It ranges from premalignant to malignant conditions.
WHO Classification:
- Hydatidiform Mole
- Complete Mole (CHM)
- Partial Mole (PHM)
- Invasive Mole
- Choriocarcinoma
- Placental Site Trophoblastic Tumor (PSTT)
- Epithelioid Trophoblastic Tumor (ETT)
⭐ GTD originates from abnormal proliferation of placental trophoblast cells, the cells that normally develop into the placenta during pregnancy.
Molar Pregnancies - Grape Expectations
Hydatidiform Mole (HM), a key Gestational Trophoblastic Disease (GTD), includes Complete (CM) and Partial (PM) types.
| Feature | Complete Mole (CM) | Partial Mole (PM) |
|---|---|---|
| Karyotype | 46,XX (most) / XY; All paternal | 69,XXY/XXX; 2 Paternal, 1 Maternal |
| Genome | Diploid (Paternal only) | Triploid |
| Gross | Diffuse swelling; "bunch of grapes" | Focal swelling; Fetus often present |
| Villous Edema | Diffuse, marked | Focal, variable |
| Tropho. Prolif. | Diffuse, circumferential | Focal, slight |
| Fetal Tissues | Absent | Often present |
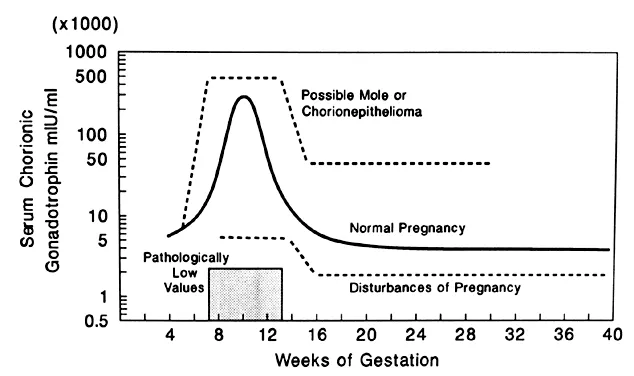
| hCG Levels | Markedly ↑ (often > 100,000 mIU/mL) | Moderately ↑ |
| Uterine Size | > dates (50%) | < dates or normal |
| Theca Lutein Cysts | Common (25-30%) | Rare |
| Complications | Hyperemesis, pre-eclampsia common | Less common |
| Ultrasound | "Snowstorm"; No fetus | Cystic placenta; Fetus/sac may be present |
| Risk of GTN | ↑ (15-20%) | ↓ (1-5%) |

⭐ Complete mole typically has a 46,XX karyotype, with all chromosomes being of paternal origin.
Malignant GTD - When Trophoblasts Attack
Malignant Gestational Trophoblastic Diseases (GTD) represent a spectrum of aggressive trophoblastic proliferations.
- Invasive Mole:
- Invades myometrium.
- Persistent ↑ hCG levels post-molar evacuation.
- Chorionic villi present.
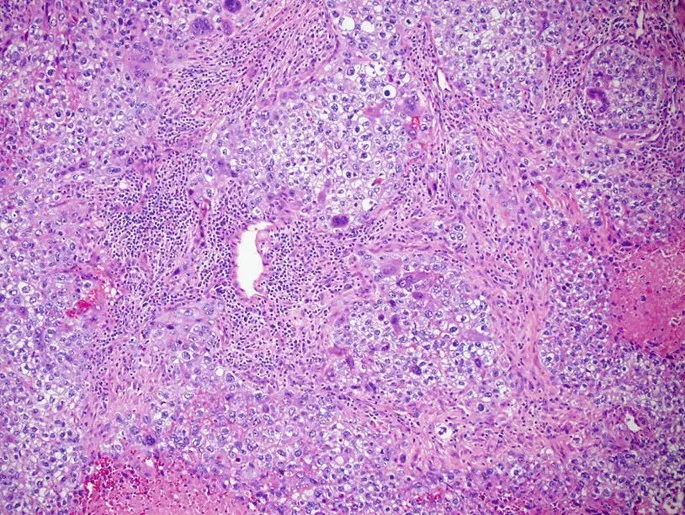
- Choriocarcinoma:
- Malignant proliferation of cytotrophoblasts & syncytiotrophoblasts.
- NO chorionic villi.
- Markedly ↑ hCG.
- Early hematogenous spread (lungs, vagina).
⭐ Choriocarcinoma is highly aggressive and metastasizes early via bloodstream, most commonly to the lungs and vagina.
- Placental Site Trophoblastic Tumor (PSTT):
- Arises from intermediate trophoblasts at placental site.
- Relatively ↓ hCG levels; hPL positive.
- Late metastasis (lymphatic/hematogenous).
- Epithelioid Trophoblastic Tumor (ETT):
- Rare, nodular proliferation of intermediate trophoblasts.
- Can mimic PSTT or squamous cell carcinoma.
- Variable hCG levels.
GTD Detective & Doctor - Spot, Stage, Solve
Spot GTD:
- Clinical: Vaginal bleeding, Uterine size > dates, Hyperemesis, Pre-eclampsia <20wks, Hyperthyroidism.
Key Investigations:
- Serial quantitative β-hCG (crucial for monitoring).
- Ultrasound (e.g., "snowstorm" for complete mole).
GTN Diagnosis (Post-Molar hCG Criteria):
- Plateau: 4 values (±10%) over 3 wks (days 1, 7, 14, 21).
- Rise: >10% for 3 values over 2 wks (days 1, 7, 14).
- Persistence: Detectable β-hCG 6 months post-evacuation.
- Histologic diagnosis (e.g., choriocarcinoma).
Stage & Solve GTN:
- FIGO 2000 anatomic staging. Prognostic risk score based on:
- Antecedent pregnancy, Interval from index pregnancy
- Pre-treatment hCG level, Largest tumor size
- Metastasis (site & number), Previous failed chemotherapy
- Score: Low risk ≤6; High risk ≥7.
⭐ Serial β-hCG monitoring is the cornerstone for diagnosis of GTN, assessment of treatment response, and detection of relapse.
High‑Yield Points - ⚡ Biggest Takeaways
- Complete moles: 46,XX (all paternal), no fetal parts, markedly ↑↑ hCG, higher choriocarcinoma risk.
- Partial moles: Triploid (e.g., 69,XXY), fetal parts present, hCG less elevated.
- hCG is the essential tumor marker for GTD diagnosis and follow-up.
- Choriocarcinoma: Highly malignant, early metastasis (lungs), excellent chemotherapy response.
- Invasive mole: Invades myometrium, persistent ↑ hCG post-evacuation.
- PSTT: Rare, from intermediate trophoblasts, produces hPL, often chemoresistant.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

