Cervical Anatomy & Histology - Neck of the Matter
- Cervix: Lower, narrow part of uterus opening into vagina.
- Ectocervix: Projects into vagina; lined by stratified squamous non-keratinized epithelium.
- Endocervix (canal): Lined by simple columnar (mucinous) epithelium.
- Key Junctions:
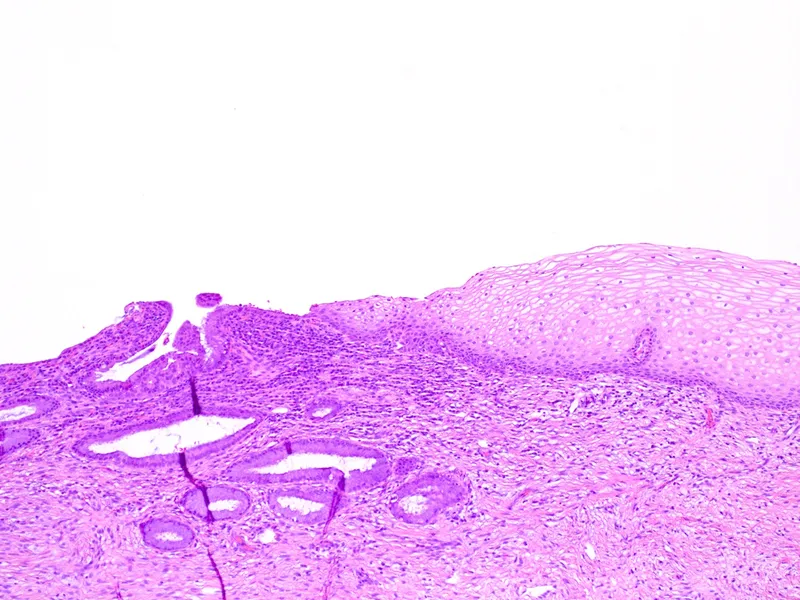
- Squamocolumnar Junction (SCJ): Original meeting point of squamous and columnar epithelia.
- Transformation Zone (TZ): Area between original and new SCJ; undergoes squamous metaplasia.
⭐ The transformation zone (TZ) is the primary site for development of cervical intraepithelial neoplasia and cervical cancer.
Cervicitis & Benign Lesions - Inflamed Gateway
- Cervicitis: Inflammation of cervix; acute (neutrophils; e.g., Chlamydia, Gonorrhea) or chronic (lymphocytes, plasma cells).
- Symptoms: Discharge, postcoital bleeding.
- Benign Lesions:
- Endocervical Polyps: Common; may cause bleeding.
- Microglandular Hyperplasia: OCP/pregnancy-linked.
⭐ Nabothian cysts are common benign findings, resulting from blocked endocervical glands.
CIN & SIL - Dysplasia Drama
Cervical Intraepithelial Neoplasia (CIN) and Squamous Intraepithelial Lesion (SIL) are spectra of pre-invasive cervical disease. Caused mainly by persistent high-risk HPV (types 16, 18). CIN grading (1, 2, 3) reflects dysplasia severity; Bethesda system (LSIL, HSIL) guides management. $p16^{INK4a}$ overexpression is a key HSIL marker.
| Feature | CIN 1 | CIN 2 | CIN 3 / CIS |
|---|---|---|---|
| Bethesda System | LSIL (Low-grade SIL) | HSIL (High-grade SIL) | HSIL (High-grade SIL) |
| Dysplasia Extent | Mild; Immature cells in lower 1/3 | Moderate; Immature cells up to lower 2/3 | Severe; Full thickness atypia (CIS) |
| Mitotic Activity | Usually basal | Suprabasal, atypical forms | Diffuse, numerous, atypical |
| $p16^{INK4a}$ (IHC) | Negative / Patchy positive | Strong, diffuse block positive | Strong, diffuse block positive |
| HPV Association | Productive infection | Transforming infection | Transforming infection |
Management depends on grade: observation for LSIL, treatment (e.g., LEEP) for HSIL to prevent progression.
⭐ HSIL (CIN 2/3) encompasses lesions with a high risk of progression to invasive carcinoma and requires management.
HPV & Carcinogenesis - Viral Villains
Human Papillomavirus (HPV), a DNA virus, is the main etiological agent.
- Types:
- High-Risk (HR-HPV): 16, 18, 31, 33, 45 (oncogenic).
- Low-Risk (LR-HPV): 6, 11 (condylomas).
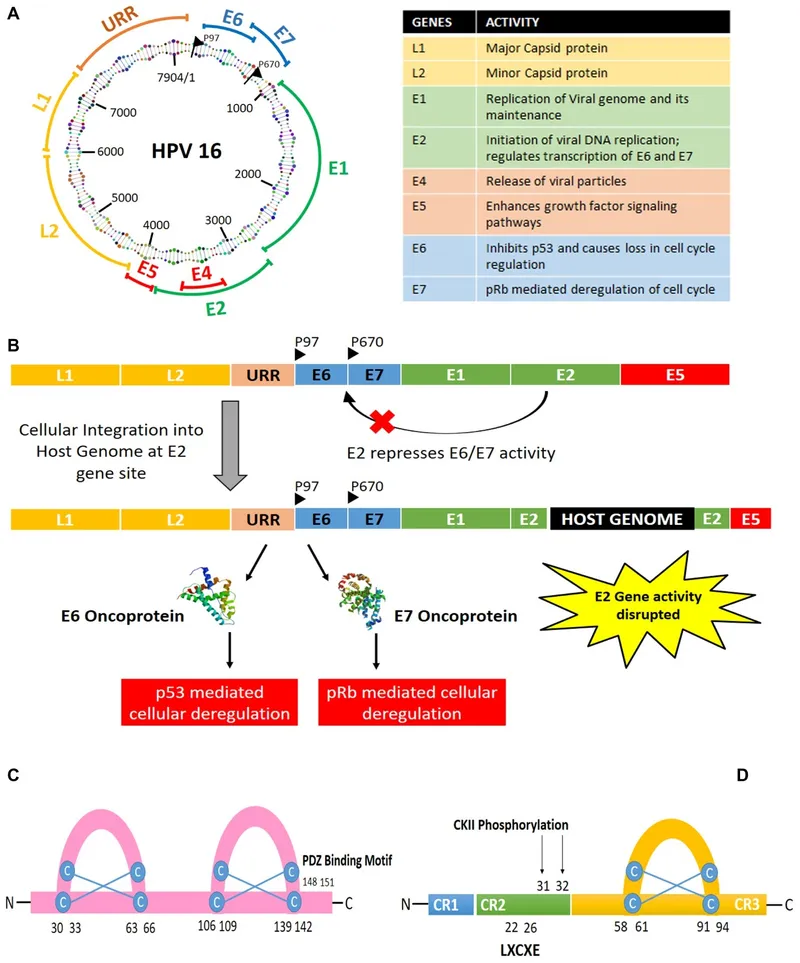
- Oncogenic Proteins (HR-HPV):
- E6: Degrades p53 (tumor suppressor) → ↓apoptosis.
- E7: Inactivates Rb (tumor suppressor) → releases E2F → ↑cell proliferation.
- Mechanism:
⭐ High-risk HPV types 16 and 18 account for over 70% of cervical cancers worldwide.
- Key Risk Factors: Multiple sexual partners, early coitarche, immunosuppression (e.g., HIV), smoking.
Invasive Cervical Cancer - Malignant March
⭐ Squamous cell carcinoma is the most common histological type of invasive cervical cancer.
-
Types & Characteristics:
Feature Squamous Cell Ca (SCC) Adenocarcinoma Epidemiology Most common type; HPV 16, 18 ↑ incidence; Younger; HPV 18 > 16 Morphology Nests/sheets of squamous cells, keratin pearls, intercellular bridges Glandular differentiation, mucin production Markers p63+, CK5/6+, p40+ CEA+, CA-125+, p16+, HIK1083 -
FIGO Staging: Crucial for management. Stage I: Cervix only. II: Beyond cervix (not to pelvic wall/lower ⅓ vagina). III: Extends to pelvic wall/lower ⅓ vagina/hydronephrosis. IV: Invades bladder/rectum or distant metastasis.
Screening & Prevention - Guarding the Gate
- Screening Tests: Pap smear (cytology), high-risk HPV (hrHPV) DNA testing, Co-testing (Pap + hrHPV).
- Key Guidelines: Pap q3yrs (21-29y); hrHPV or Co-test q5yrs (30-65y).
- Primary Prevention: HPV vaccination (e.g., Gardasil 9) protects against oncogenic HPV types.
⭐ The Bethesda System is the standard for reporting cervical cytology (Pap smear) results.
High‑Yield Points - ⚡ Biggest Takeaways
- High-risk HPV (16, 18) causes most CIN and cervical cancer.
- Koilocytes (halo, wrinkled nucleus) signify HPV infection.
- LSIL (CIN I) often regresses; HSIL (CIN II/III) has higher progression risk to invasive cancer.
- p16INK4a overexpression is a key biomarker for HSIL.
- Most cervical cancers arise in the transformation zone.
- Squamous cell carcinoma is the most common type.
- Pap smear and HPV DNA testing are vital for screening.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


