Hypertensive Nephropathy - Pressure Problems
-
Benign Nephrosclerosis: Chronic, mild-moderate hypertension.
-
Pathology: Hyaline arteriolosclerosis (thickened arteriolar walls, narrowed lumen).
-
Gross: Symmetrically atrophic kidneys, finely granular cortical surface ('granular contracted kidneys').
-
Clinical: Slow, progressive renal insufficiency.
-
-
Malignant (Accelerated) Nephrosclerosis: Severe, rapidly rising BP (often >180/120 mmHg).
-
Pathology:
- Fibrinoid necrosis of arterioles (smudgy, eosinophilic deposits).
- Hyperplastic arteriolosclerosis ('onion-skinning' due to concentric smooth muscle cell proliferation & collagen deposition).
-
Gross: Normal size or slightly enlarged kidneys; petechial hemorrhages on cortical surface ('flea-bitten' kidney).
-
Clinical: Acute renal failure, papilledema, hypertensive encephalopathy, headaches, visual disturbances.
-
⭐ 'Onion-skin' appearance of arterioles is pathognomonic for malignant hypertension.
📌 Mnemonic: Benign = Boringly slow, hyaline. Malignant = Madly fast, fibrinoid & onion skinning, Many petechiae (flea-bitten).
Renal Artery Stenosis - Pipe Dreams
- Causes
- Atherosclerosis: Most common; elderly males, ostial.
- Fibromuscular Dysplasia (FMD): Young females; 'string of beads'. 📌 FMD - 'Females, Medial, Dysplasia'.
- Pathophysiology: ↓ Renal Perfusion → RAAS activation → Renovascular HTN.
- Clinical Features
- Refractory HTN (>70% stenosis).
- Abdominal bruit.
- Flash pulmonary edema.
- AKI on ACEi/ARB.
- Diagnosis
- Doppler US: Initial.
- CTA / MRA.
- DSA: Gold standard.
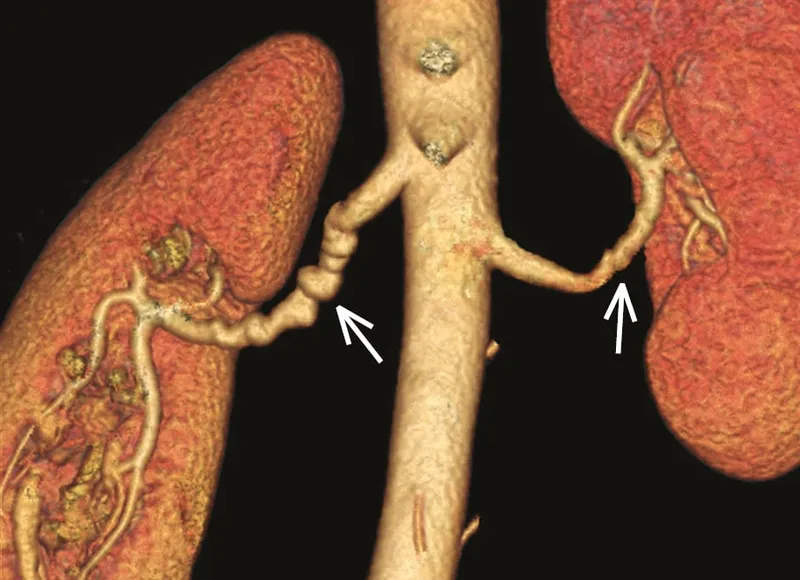

⭐ Unexplained hypokalemia can be a clue for Renal Artery Stenosis due to secondary hyperaldosteronism.
Thrombotic Microangiopathies - Clot Chaos
- Pathophysiology: Endothelial injury → platelet activation → microvascular thrombi.
- Hallmarks: Microangiopathic Hemolytic Anemia (MAHA), thrombocytopenia, organ damage (kidney, CNS).
| Feature | Hemolytic Uremic Syndrome (HUS) | Thrombotic Thrombocytopenic Purpura (TTP) |
|---|---|---|
| Etiology | Typical (D+): Shiga toxin (E.coli O157:H7) | Acquired: Anti-ADAMTS13 Abs |
| Atypical (D-): Complement dysregulation | Hereditary: ADAMTS13 mutations. Activity <10% | |
| Key Features | Predominant acute renal failure (children) | Predominant neurological symptoms, fever (adults) |
| Lab Findings | MAHA, thrombocytopenia, schistocytes, ↑ creatinine | MAHA, thrombocytopenia, schistocytes, severe ADAMTS13 deficiency |
| Organ Inv. | Kidney (severe) >> CNS | CNS (prominent), Kidney (milder) |


⭐ Presence of schistocytes on peripheral blood smear is a hallmark of thrombotic microangiopathies.
Emboli & Infarcts - Vascular Blockades
- Atheroembolic Renal Disease (AERD):
- Cause: Cholesterol crystal emboli, typically after invasive arterial procedures (e.g., angiography).
- Clinical: Subacute renal failure (↑creatinine), eosinophilia, livedo reticularis, purple toes, ↓complement.
- Patho: Biconvex, needle-shaped cholesterol crystal clefts in small renal vessels.
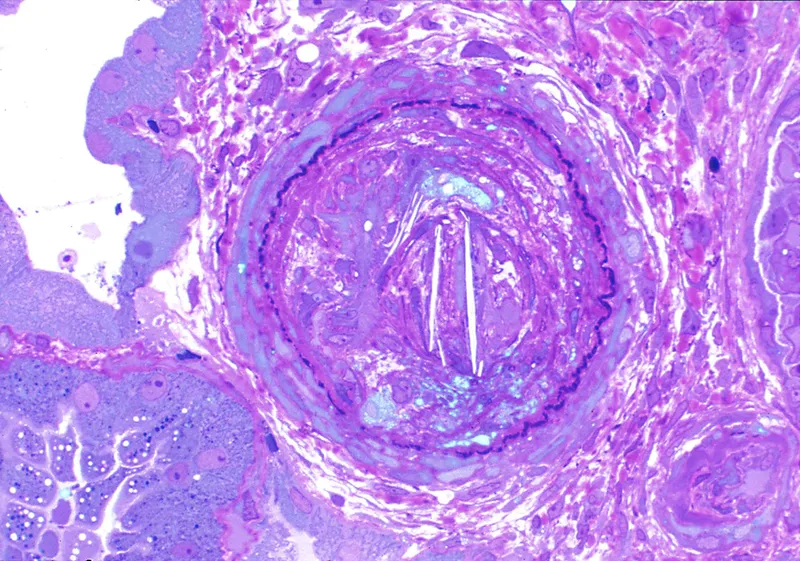
- Renal Infarction:
- Etiology: Thromboembolism (e.g., AF, endocarditis, mural thrombi); also trauma, vasculitis (PAN).
- Gross: Wedge-shaped pale cortical necrosis. Old infarcts: shrunken, fibrotic.

- Features: Acute flank pain, hematuria, fever, nausea, markedly ↑LDH.
⭐ Atheroembolic renal disease often presents with a subacute rise in creatinine, eosinophilia, and low complement levels after an invasive vascular procedure.
High‑Yield Points - ⚡ Biggest Takeaways
- Renal Artery Stenosis (RAS): Key cause of secondary HTN; atherosclerosis (elderly), fibromuscular dysplasia (young women).
- Malignant Hypertension: Fibrinoid necrosis, hyperplastic arteriolosclerosis ("onion-skin"), "flea-bitten" kidney. Benign: hyaline arteriolosclerosis.
- Thrombotic Microangiopathies (TMAs): HUS (Shiga toxin, child, renal failure) vs. TTP (ADAMTS13, adult, neuro).
- Renal Infarcts: Wedge-shaped cortical necrosis, usually embolic.
- Atheroembolic Disease: Cholesterol crystals post-procedure; eosinophilia, livedo reticularis.
- Scleroderma Renal Crisis: Abrupt severe HTN & AKI.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

