Intro & Etiology - Cystic Conundrum
- Definition: Localized fluid collection (amylase-rich) near pancreas, enclosed by a non-epithelialized, fibrous, or granulation tissue wall.
- Lacks true epithelial lining (unlike true cysts).
- Etiology:
- Acute Pancreatitis: Most common cause.
⭐ Most pseudocysts (75-85%) are a sequela of acute pancreatitis.
- Chronic Pancreatitis: Often due to ductal obstruction.
- Pancreatic Trauma: Blunt abdominal injury, iatrogenic (post-surgical/ERCP).
- Pancreatic Neoplasms (rarely).
- Idiopathic.
- Acute Pancreatitis: Most common cause.

Pathophys & Histo - Wall Woes
Error generating content for this concept group: Failed to process successful response
Clinical Features & Diagnosis - Tummy Troubles & Tell-Tales
- Symptoms: Often asymptomatic. If present: epigastric pain (radiates to back), nausea, vomiting, early satiety, weight loss. Palpable mass. Jaundice (biliary compression).
- History: Prior pancreatitis or trauma.
- Labs: Amylase/lipase may be ↑ or normal (esp. if chronic, >6 wks). CA 19-9 mildly ↑ possible.
- Imaging:
- USG: Initial scan for fluid.
- CECT Abdomen: Confirms (wall forms ~4-6 wks), details size, location, complications (infection, hemorrhage).
- MRI/MRCP: If CECT unclear or for ductal anatomy.
- EUS+FNA: Complex cases/rule out neoplasm (fluid: ↑ amylase, low CEA).
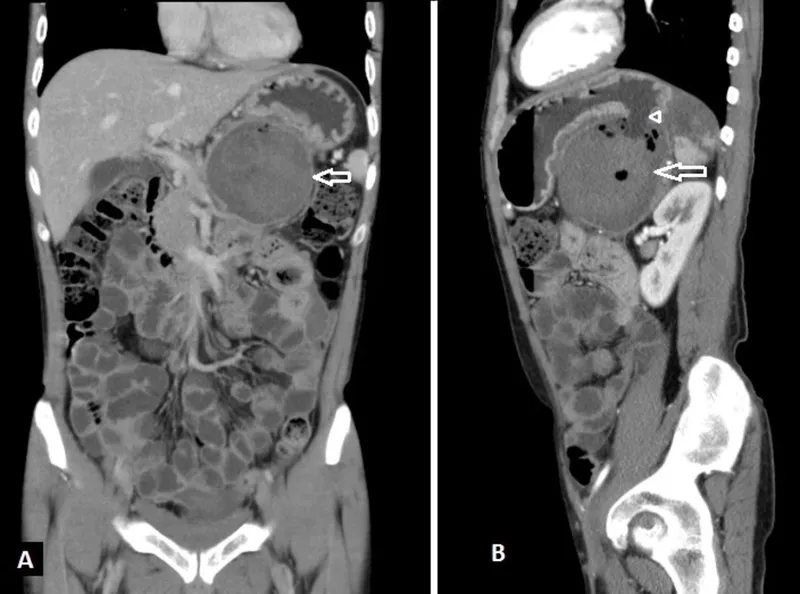
⭐ CECT abdomen is the gold standard for diagnosing pancreatic pseudocysts (mature wall visible after 4-6 weeks) and assessing complications.
Complications & Management - Perilous Pockets & Plans
- Key Complications:
- Infection (abscess formation), hemorrhage (e.g., from pseudoaneurysm).
- Rupture (peritonitis), obstruction (gastric, biliary), persistent severe pain.
- Management Strategy:
- Conservative: Watchful waiting if asymptomatic, <6cm, AND <6wks old.
⭐ Spontaneous resolution in up to 50% of pseudocysts, especially if <6cm and asymptomatic; watchful waiting is often the initial approach.
- Intervention indicated if: Symptomatic, size >6cm, duration >6wks, or complications present.
- Endoscopic drainage (cystogastrostomy/duodenostomy) is first-line.
- Percutaneous drainage: Alternative, especially for infected pseudocysts.
- Surgical drainage (e.g., cystojejunostomy): Reserved for failures or specific anatomical challenges.
- Conservative: Watchful waiting if asymptomatic, <6cm, AND <6wks old.

High‑Yield Points - ⚡ Biggest Takeaways
- Most common pancreatic cystic lesion, often a sequela of acute/chronic pancreatitis or trauma.
- Distinctive feature: lacks a true epithelial lining; wall is fibrous and granulation tissue.
- Typically peripancreatic, frequently located in the lesser sac.
- Fluid analysis reveals markedly elevated amylase and lipase levels.
- CT scan is the primary diagnostic imaging modality.
- Major complications: infection, hemorrhage, rupture, pseudoaneurysm.
- Management: observation for asymptomatic cases; drainage if symptomatic, large (>6cm), or complicated.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

