Embryology - Budding Beginnings
- Origin: Foregut endoderm forms dorsal & ventral buds at duodenal level (wk 5).
- Rotation & Fusion: Ventral bud rotates dorsally with duodenal C-loop, fusing with dorsal bud (wk 7).
- Derivatives:
⭐ Ventral bud forms the uncinate process and inferior part of head, along with the main pancreatic duct (of Wirsung); Dorsal bud forms the rest (body, tail, superior part of head) and accessory duct (of Santorini).

Pancreas Divisum - Duct Drama
- Pathogenesis: Failure of fusion of dorsal & ventral pancreatic buds in embryogenesis.
- Dorsal duct (Santorini) drains most of pancreas (body, tail, superior head) via minor papilla.
- Ventral duct (Wirsung) drains small part of head (uncinate) via major papilla.
- Clinical Features:
- Mostly asymptomatic.
- Minority: Recurrent acute pancreatitis or chronic pancreatitis due to relative stenosis of minor papilla. 📌 "Divisum = Divided drainage, Dominant Dorsal duct."
- Diagnosis: MRCP, ERCP (gold standard).
⭐ Pancreas divisum is the most common congenital anomaly of the pancreas, resulting from failure of fusion of dorsal and ventral pancreatic buds.
Annular Pancreas - Duodenal Hug
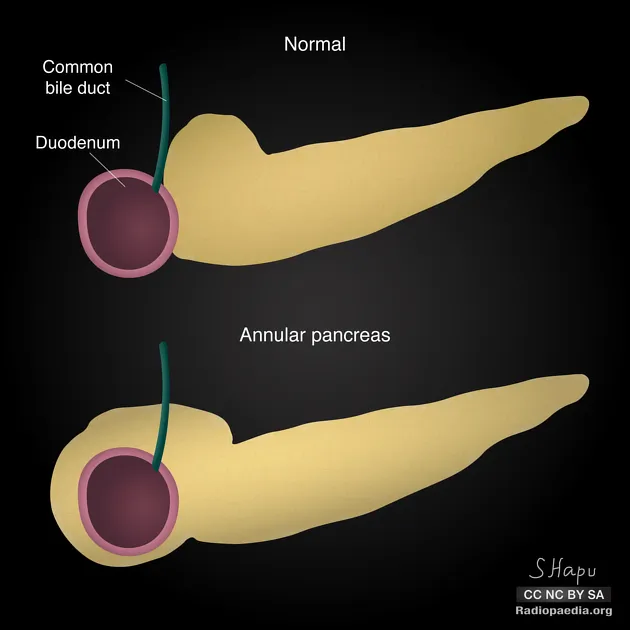
- Definition: Rare congenital anomaly where a ring of pancreatic tissue, continuous with the pancreatic head, encircles the second part of the duodenum.
- Embryology: Results from abnormal migration/fusion of the ventral pancreatic bud, which fails to rotate completely with the duodenum, instead splitting and encircling it.
- Clinical Presentation:
- Neonates: Duodenal obstruction (bilious or non-bilious vomiting, abdominal distension), feeding intolerance. Can be complete or partial obstruction.
- Adults: Often asymptomatic. May present with peptic ulcer disease, pancreatitis, or duodenal obstruction.
- Associations:
- Down syndrome (Trisomy 21)
- Intestinal atresia (especially duodenal atresia)
- Malrotation
- Pancreas divisum
- Diagnosis:
- Abdominal X-ray:
Ectopic & Rarities - Pancreas Outliers
- Ectopic Pancreas:
- Pancreatic tissue outside normal location, no ductal/vascular connection.
- Sites: Stomach (commonest), duodenum, jejunum, Meckel's diverticulum.
- Clinical: Usually asymptomatic; can cause pain, bleeding, obstruction.
- Histology: Normal acini, ducts, ± Islets of Langerhans.
- Complications: Pancreatitis, pseudocyst, rarely malignancy.
- Pancreatic Agenesis:
- Complete: Rare, lethal. Often with other anomalies.
- Partial (Dorsal Agenesis): More common. Absence of body/tail. May cause diabetes mellitus (↓ islets).
- Congenital Cysts:
- True cysts: ductal epithelium lining.
- Often solitary. Multiple in syndromes (Von Hippel-Lindau, ADPKD).
- Differentiate from pseudocysts (no epithelial lining, post-inflammatory).

⭐ The most common site for ectopic pancreatic tissue is the stomach, followed by the duodenum and jejunum.
Diagnosis - Anomaly Hunt
- Imaging Modalities:
- Ultrasound (USG): Initial, often incidental.
- CT Scan: Defines anatomy, complications (pancreatitis, pseudocysts).
- Endoscopic Ultrasound (EUS): Detailed parenchyma/duct views.
- Ductal System Evaluation:
- ERCP: Diagnostic & therapeutic potential.
⭐ MRCP (Magnetic Resonance Cholangiopancreatography) is the non-invasive imaging modality of choice for diagnosing most congenital pancreatic anomalies by visualizing ductal anatomy.
- Confirmatory (if needed):
- Biopsy/Histopathology: If malignancy suspected or diagnosis unclear.
High‑Yield Points - ⚡ Biggest Takeaways
- Pancreas divisum: Most common anomaly; failed fusion of dorsal/ventral buds; Santorini drains most pancreas via minor papilla; ↑ risk of pancreatitis.
- Annular pancreas: Encircles duodenum causing neonatal obstruction (bilious vomiting); associated with Down syndrome.
- Ectopic pancreas: Commonest in stomach, duodenum, Meckel's diverticulum; mostly asymptomatic, can cause pain or bleeding.
- Pancreatic agenesis: Rare; dorsal agenesis more common than complete; leads to neonatal diabetes mellitus.
- Congenital cysts: True cysts; may be associated with von Hippel-Lindau (VHL) disease or ADPKD.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

