Demyelination Basics - Myelin Under Siege
- Myelin: Vital lipid-protein sheath insulating nerve axons.
- CNS: Formed by oligodendrocytes (one cell supports multiple axons).
- PNS: Formed by Schwann cells (one cell per axon segment).
- Function: Facilitates saltatory conduction for rapid (↑) nerve impulse velocity.
- Demyelination: Pathological loss or damage to myelin; axons initially preserved.
- Impact: Slows, blocks, or desynchronizes nerve signals, causing neurological deficits.
- Prolonged demyelination can lead to secondary axonal degeneration and permanent loss.
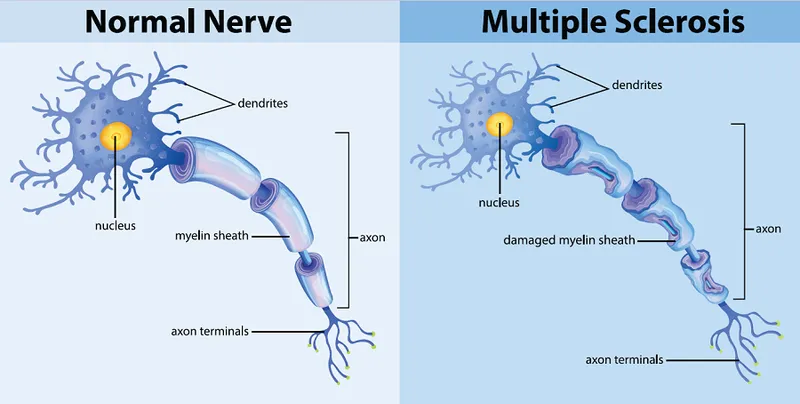
⭐ The CNS has limited capacity for remyelination compared to the PNS, contributing to chronic disability in diseases like MS.
Multiple Sclerosis - Plaque Attack Central
- Autoimmune CNS demyelination; HLA-DR2, EBV, ↓Vit D.
- Patho: T-cell attack on myelin/oligodendrocytes → axonal damage.
- Key Features:
- Optic neuritis (painful ↓vision, RAPD).
- Internuclear Ophthalmoplegia (INO).
- Lhermitte’s sign (spinal shock on neck flexion).
- Uhthoff's phenomenon (symptoms worsen with heat).
- Charcot's Neurologic Triad (📌 NISS): Nystagmus, Intention Tremor, Scanning Speech.
- Sensory loss, weakness, fatigue, bladder/bowel issues.
- Diagnosis: McDonald Criteria (DIS & DIT).
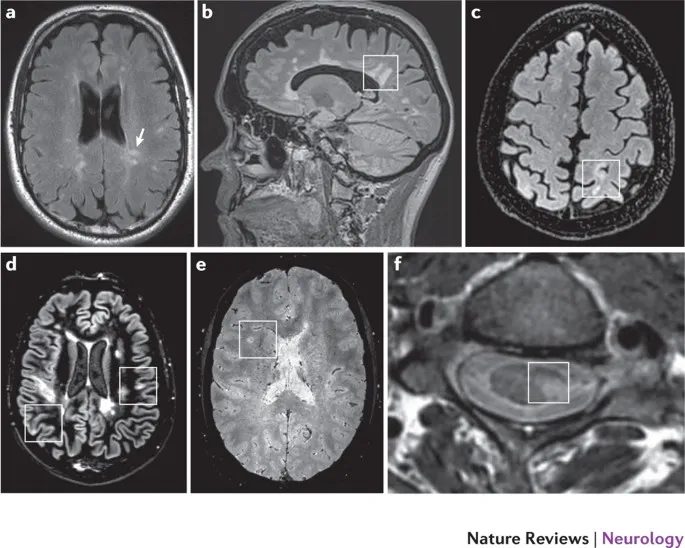
- MRI: Periventricular plaques (Dawson's fingers), corpus callosum, brainstem, spinal cord. Active lesions: Gd-enhancement.
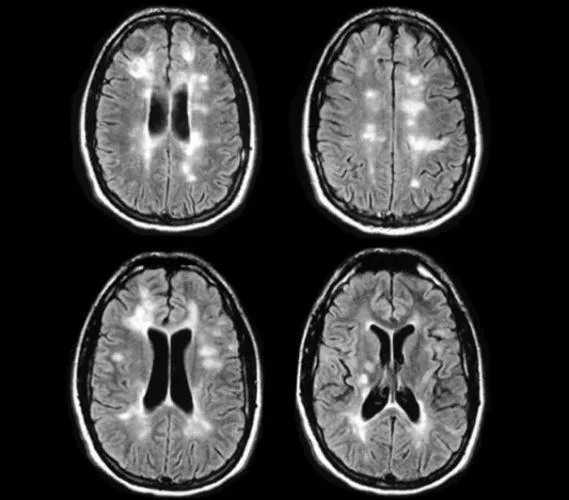
- CSF: ↑IgG index, Oligoclonal Bands (OCBs).
- MRI: Periventricular plaques (Dawson's fingers), corpus callosum, brainstem, spinal cord. Active lesions: Gd-enhancement.
- Plaques: Demyelination foci. Acute (inflammation) → Chronic (gliosis, axonal loss). Shadow plaques (remyelination).
- Types: RRMS (~85%), SPMS, PPMS.
> ⭐ Periventricular white matter plaques (Dawson's fingers) are highly characteristic on MRI.
- Acute Relapse: IV Methylprednisolone. Refractory: Plasma exchange.
- DMTs: IFN-β, Glatiramer acetate, Fingolimod, Natalizumab, Ocrelizumab.
MS Variants & NMOSD - Mimicry Mayhem
- MS Variants (Atypical):
- Marburg: Acute, fulminant; large, destructive lesions. Often fatal.
- Balo's Concentric Sclerosis: Rare; concentric rings of demyelination.
- Schilder's Disease: Extensive, bilateral demyelination; typically children.
- NMOSD (Devic's Disease):
- Key: AQP4-IgG positive (most cases).
- Classic triad: Optic neuritis (often bilateral, severe) + Transverse myelitis (longitudinally extensive, ≥3 segments) + Area postrema syndrome.
- Brain lesions: Periependymal, hypothalamus, brainstem; not typical MS pattern.
⭐ NMOSD is an astrocytopathy (targeting AQP4 on astrocytes), whereas MS is primarily a disease of oligodendrocytes/myelin.
Other CNS Demyelinators - Swift Sheath Strippers
- Progressive Multifocal Leukoencephalopathy (PML)
- Etiology: JC virus reactivation.
- Risk: Immunocompromised (AIDS, immunosuppressants).
- Patho: Lysis of oligodendrocytes → multifocal demyelination.
- Clinical: Rapid, progressive neurological deficits; often fatal.
- Dx: JC virus DNA in CSF.
- Osmotic Demyelination Syndrome (ODS)
- A.k.a. Central Pontine Myelinolysis (CPM).
- Etiology: Rapid correction of severe hyponatremia.
⭐ Prevention is key: correct hyponatremia slowly, typically ≤ 8-10 mEq/L in 24 hours.
- Site: Pons (classic), extrapontine areas.
- Clinical: Quadriparesis, dysarthria, dysphagia, "locked-in" syndrome.
- Marchiafava-Bignami Disease (MBD)
- Rare; associated with chronic alcoholism & nutritional deficiency.
- Patho: Demyelination & necrosis of corpus callosum.
- Subacute Sclerosing Panencephalitis (SSPE)
- Etiology: Persistent, aberrant measles virus infection.
- Onset: Years after initial measles.
- Clinical: Progressive cognitive decline, myoclonic jerks, seizures.
- Dx: ↑ measles antibodies in CSF/serum; EEG: periodic complexes. Fatal.
High‑Yield Points - ⚡ Biggest Takeaways
- MS: Most common, autoimmune; relapsing-remitting course; periventricular plaques (Dawson's fingers), oligoclonal bands in CSF.
- ADEM: Monophasic, post-infectious/vaccinial, common in children; widespread perivenular demyelination.
- PML: JC virus in immunocompromised (HIV); non-inflammatory demyelination of oligodendrocytes.
- Osmotic Demyelination Syndrome (CPM): Rapid correction of hyponatremia; affects pons, may cause locked-in syndrome.
- GBS (AIDP): Ascending paralysis, areflexia, post-Campylobacter; albumino-cytological dissociation in CSF.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

