Paraneoplastic Syndromes: Overview - Cancer's Sneaky Sidekicks
- Definition: Remote effects of malignancy; not due to direct tumor mass, invasion, metastasis, or therapy side effects.
- Prevalence: Affects ~10-15% of cancer patients.
- Clinical Impact: Earliest sign of occult cancer; mimics metastasis; causes significant morbidity/mortality.
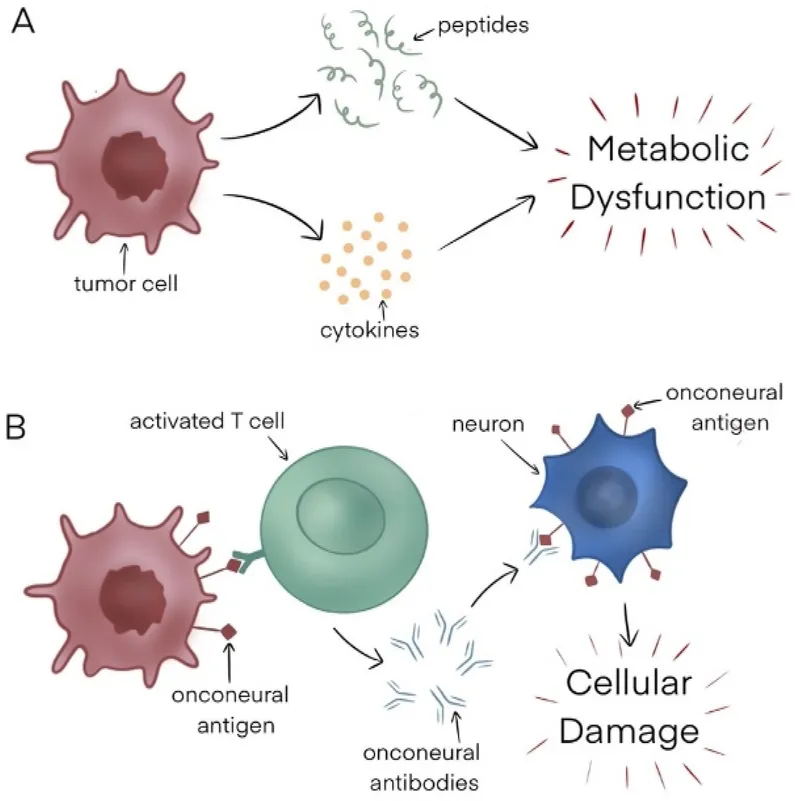
- **Pathogenesis (Mechanisms):
- Tumor secretion: Hormones, peptides, enzymes, cytokines (e.g., ACTH, ADH, PTHrP).
- Immunological: Autoantibodies or T-cells against tumor antigens cross-react with normal tissues.
⭐ Small cell lung cancer (SCLC) is notorious for causing multiple paraneoplastic syndromes, especially SIADH and Cushing's syndrome.
Paraneoplastic Syndromes: Endocrine - Hormones Gone Wild
Ectopic hormone production by non-endocrine tumors can cause a variety of syndromes. These often mimic primary endocrine disorders.
| Syndrome | Ectopic Product/Mediator | Common Cancers |
|---|---|---|
| Cushing's Syndrome | ACTH | SCLC, Pancreatic, Neural tumors |
| SIADH | ADH | SCLC, CNS malignancies |
| Hypercalcemia | PTHrP, TGF-$\alpha$, TNF, IL-1 | Lung (Squamous), Breast, Renal, Ovarian, Multiple Myeloma |
| Hypoglycemia | IGF-2 | Fibrosarcoma, Other mesenchymal sarcomas, Hepatocellular Ca |
| Carcinoid Syndrome (metastatic) | Serotonin, Bradykinin | Bronchial carcinoid, Pancreatic, Gastric |
| Polycythemia | Erythropoietin | Renal, Cerebellar hemangioblastoma, Hepatocellular Ca, Leiomyoma |
Paraneoplastic Syndromes: Neurological - Brain Under Siege
Neurological paraneoplastic syndromes arise from immune responses against tumors that cross-react with nervous system antigens. Early recognition is key.
| Syndrome | Associated Antibody (if any) | Common Cancers |
|---|---|---|
| Limbic Encephalitis | Anti-Hu, Anti-Ma2, Anti-NMDA Receptor | SCLC, Testicular, Ovarian teratoma |
| Paraneoplastic Cerebellar Degen. | Anti-Yo (PCA-1), Anti-Hu, Anti-Tr (DNER) | Ovarian, Breast, SCLC, Hodgkin Lymphoma |
| Lambert-Eaton Myasthenic Syndrome | Anti-VGCC (P/Q-type) | SCLC (~60%) |
| Opsoclonus-Myoclonus Syndrome | Anti-Ri (ANNA-2) (kids); often none | Neuroblastoma (kids), SCLC, Breast |
| Stiff-Person Syndrome | Anti-GAD, Anti-Amphiphysin | Breast, SCLC, Thymoma, Lung |
| Sensory Neuronopathy | Anti-Hu (ANNA-1) | SCLC, Neuroblastoma |
⭐ Lambert-Eaton Myasthenic Syndrome (LEMS) often presents with proximal muscle weakness that improves with exercise and autonomic dysfunction (e.g., dry mouth); strongly associated with SCLC (Small Cell Lung Cancer).
Paraneoplastic Syndromes: Other Systems - Systemic Shenanigans
- Hematologic:
- Polycythemia (↑EPO): Renal cell, hepatocellular ca, hemangioblastoma.
- Anemia: Chronic disease; Pure Red Cell Aplasia (Thymoma).
- Trousseau Syndrome (migratory thrombophlebitis): Pancreatic, lung ca.
- Eosinophilia (Hodgkin lymphoma); Leukemoid reaction.
- Dermatologic:
- Acanthosis Nigricans: GI (gastric), lung, uterine ca. Velvety plaques.
- Dermatomyositis/Polymyositis: Ovarian, lung, breast ca. Gottron's, heliotrope.
- Leser-Trélat Sign: Sudden seborrheic keratoses; GI adenocarcinomas.
- Sweet's Syndrome: AML. Painful red plaques.
- Rheumatologic:
- Hypertrophic Osteoarthropathy (HOA): Lung ca (NSCLC). Clubbing, periostitis.
- Palmar Fasciitis & Polyarthritis: Ovarian ca. "Tripe palms".

⭐ Trousseau syndrome (migratory thrombophlebitis) strongly suggests visceral malignancy, especially pancreatic adenocarcinoma.
Paraneoplastic Syndromes: Diagnosis & Significance - Unmasking the Culprit
- Diagnosis: High suspicion. Exclude mimics (metastasis, metabolic, infection, drugs). Test specific antibodies (anti-Hu, -Yo). Systematic tumor search.
- Significance: Often first malignancy sign. Signals recurrence. Severity ≠ tumor burden. Act as tumor markers.
⭐ Lambert-Eaton Myasthenic Syndrome (LEMS) is strongly associated with Small Cell Lung Cancer (SCLC).
High‑Yield Points - ⚡ Biggest Takeaways
- Eaton-Lambert syndrome (anti-Ca²⁺ channel Abs) is strongly linked to Small Cell Lung Cancer (SCLC).
- Hypercalcemia (PTHrP-mediated) is common with Squamous Cell Lung Cancer and Renal Cell Carcinoma.
- SIADH (hyponatremia) & ectopic ACTH (Cushing's) are classic paraneoplastic features of SCLC.
- Malignant acanthosis nigricans can indicate underlying gastric adenocarcinoma or other visceral cancers.
- Dermatomyositis/Polymyositis are frequently associated with ovarian, lung, and GI cancers.
- Polycythemia (ectopic EPO) can occur with Renal Cell Carcinoma, hepatocellular carcinoma, hemangioblastoma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

