Intro to Cancer Epidemiology - Numbers & Trends Game
- Cancer Epidemiology: Study of cancer distribution & determinants in populations.
- Key Metrics:
- Incidence: New cases/defined pop/time. (Measures risk)
- Prevalence: Total existing cases (new+old)/pop/point in time. (Measures burden)
- Mortality Rate: Deaths from cancer/pop/time.
- Survival Rate: % alive for period (e.g., 5-yr) post-diagnosis.
- Important Rates:
- Crude Rates: Observed rates in a pop.
- Age-Standardized Rates (ASR): Age-adjusted for fair comparison across pops.
- Data Source: GLOBOCAN (IARC): Global stats.
- General Trends: ↑ global incidence; improving survival for many.
⭐ Lung cancer: most common diagnosis in males & leading cause of cancer death globally.
Cancer Risk Factors & Etiology - The Usual Suspects
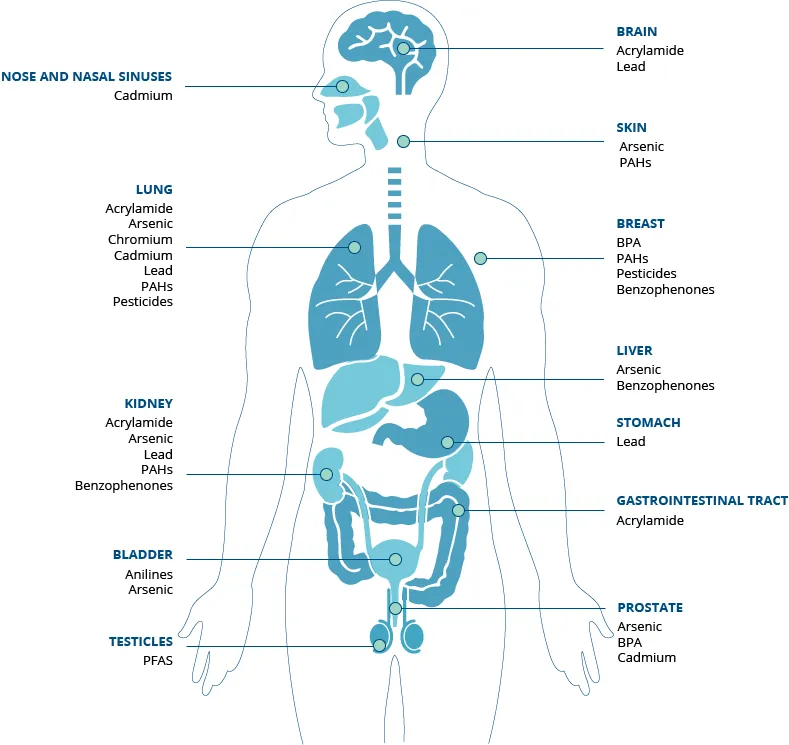
- Chemicals:
- Tobacco (Polycyclic Aromatic Hydrocarbons, Nitrosamines): Lung, oral, bladder.
- Aflatoxin $B_1$ (Aspergillus): Hepatocellular carcinoma (HCC).
- Asbestos: Lung, mesothelioma, laryngeal.
- Arsenic: Skin (palms/soles), lung, bladder.
- Benzene: Leukemia.
- Vinyl chloride: Liver angiosarcoma.
- Radiation:
- Ionizing (X-rays, radon): Leukemia, thyroid.
- UV (Sunlight - UVB): Skin (melanoma, BCC, SCC).
- Infections:
- Viruses: HPV (cervical, anal, oropharyngeal), HBV/HCV (HCC), EBV (Burkitt's, nasopharyngeal), HTLV-1 (ATL), HHV-8 (Kaposi).
- Bacteria: H. pylori (gastric adenocarcinoma, MALToma).
- Parasites: Schistosoma haematobium (bladder SCC), Clonorchis sinensis (cholangiocarcinoma).
- Lifestyle/Heredity:
- Alcohol (synergistic with tobacco).
- Diet (↑fat/↓fiber, obesity).
- Genetics (BRCA, Lynch).
⭐ Tobacco smoke is the single most important environmental carcinogen, implicated in ~30% of all cancer deaths in developed countries.
Indian Cancer Scenario - India's Cancer Atlas
- Source: National Centre for Disease Informatics and Research (NCDIR-ICMR).
- Leading Cancers (India): Lung, Breast, Cervical, Oral, Colorectal.
- Common Cancers by Gender:
- Males: Lung, Oral cavity, Prostate, Stomach, Colorectal.
- Females: Breast, Cervix uteri, Ovary, Colorectal, Lung.
- Regional Hotspots:
- Northeast: ↑ Oesophageal, Stomach cancers.
- Gangetic belt: ↑ Gallbladder cancer (females).
- Notable Trends:
- ↑ Breast cancer (especially urban).
- ↑ Colorectal cancer.
- ↓ Cervical cancer (variable, improved screening).
- High burden of tobacco-related cancers (TRCs).
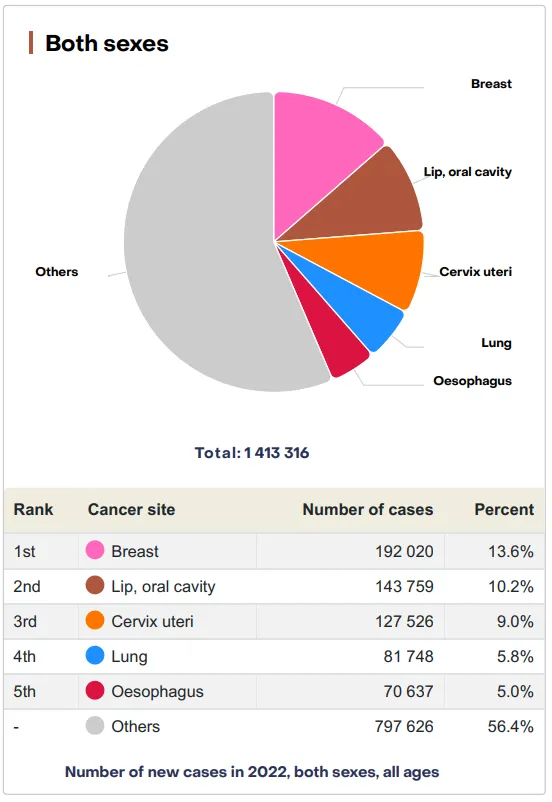
⭐ Tobacco-related cancers (TRCs) constitute about 30% of the cancer burden in males and 10-12% in females in India.
Cancer Prevention & Screening - Shield & Scope
- Levels of Prevention:
- Primary: Prevent cancer onset.
- Lifestyle: Healthy diet, exercise, no tobacco/alcohol.
- Vaccines: HPV (Cervical, H&N), HBV (Liver).
- Chemoprevention: Tamoxifen (Breast), Aspirin (CRC).
- Secondary (Screening): Early detection.
- Cervical: Pap smear (Age 30-65 yrs, q3-5 yrs); VIA/VILI.
- Breast: SBE, CBE, Mammography (Age >50 yrs, or >40 high-risk).
- Oral: OVE (tobacco users).
- Colorectal: FOBT/Colonoscopy (Age >50 yrs).
- Tertiary: Limit complications post-diagnosis (rehab, palliative).
- Primary: Prevent cancer onset.
⭐ Screening is justified if benefits (early detection, improved outcomes) outweigh harms (overdiagnosis, cost, anxiety) - core of Wilson-Jungner criteria.
High‑Yield Points - ⚡ Biggest Takeaways
- Tobacco is the leading preventable cause of cancer mortality in India.
- Key oncogenic infections: HPV (cervical), HBV/HCV (liver), H. pylori (stomach).
- Early detection via screening for cervical, breast, and oral cancers is vital.
- Lifestyle modifications: ↑fruits/vegetables, regular exercise, ↓alcohol significantly reduce risk.
- Occupational carcinogens like asbestos (mesothelioma) and benzene (leukemia) are important.
- Common cancers in India: Men - Lung/Oral; Women - Breast/Cervical.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

