Molecular Dx Intro - Germ Secrets Unlocked
- Foundation: Leverages nucleic acid (NA) tech to identify pathogens via their unique DNA/RNA signatures.
- Core Principle: Specific NA targets (e.g., virulence genes) → Amplification (like PCR) → Detection.
- Key Advantages:
- ↑ Speed, sensitivity, specificity vs. traditional.
- Detects non-culturable/fastidious organisms.
- Quantifies pathogen load; monitors treatment.
- Identifies antimicrobial resistance markers.
⭐ Molecular methods can detect non-culturable or slow-growing organisms like Mycobacterium tuberculosis or certain viruses.
PCR Techniques - DNA's Copy Machine
Polymerase Chain Reaction (PCR) rapidly amplifies minute DNA segments, enabling detection of microbial genetic material.
- Principle: In vitro enzymatic DNA replication.
- Requires: DNA template, specific primers, Taq polymerase (heat-stable), dNTPs, MgCl₂ buffer.
- Core Steps (Thermal Cycling):
- Key PCR Variants:
- RT-PCR (Reverse Transcriptase): For RNA targets (e.g., HIV, HCV, Influenza). RNA → cDNA first.
- qPCR (Quantitative/Real-Time): Measures DNA/RNA quantity in real-time.
- Multiplex PCR: Detects multiple DNA/RNA targets simultaneously.
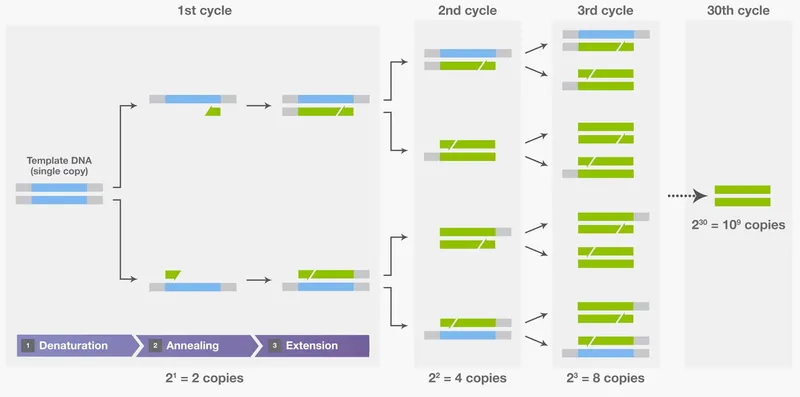
⭐ Quantitative PCR (qPCR) not only detects but also quantifies pathogen load, crucial for monitoring diseases like HIV or Hepatitis C.
Advanced Molecular Dx - Beyond Basic PCR
- Nucleic Acid Hybridization: Uses labeled probes to detect specific DNA/RNA sequences.
- Probes: Short, specific DNA/RNA sequences (radioactive/non-radioactive label).
- Fluorescence In Situ Hybridization (FISH): Visualizes nucleic acids in cells/tissues using fluorescent probes; rapid identification of pathogens (e.g., CMV, EBV).
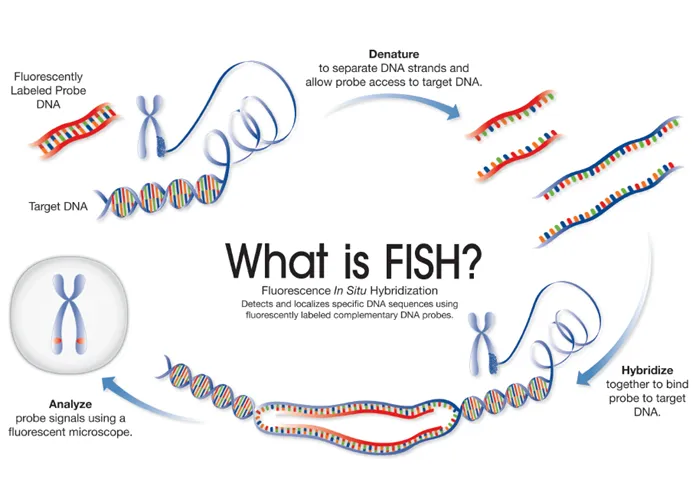 for pathogen detection)
for pathogen detection)
- Sequencing Methods: Determine exact nucleotide order.
- Sanger Sequencing: Gold standard for single gene analysis; identifies mutations, resistance.
- Next-Generation Sequencing (NGS): High-throughput, sequences millions of fragments simultaneously.
⭐ Next-Generation Sequencing (NGS) is revolutionizing outbreak investigations and the detection of antimicrobial resistance genes.
- Other Amplification Techniques: Isothermal methods, no thermocycler needed.
- Loop-mediated Isothermal Amplification (LAMP): Rapid, simple, cost-effective; good for point-of-care.
- Nucleic Acid Sequence-Based Amplification (NASBA): Amplifies RNA; useful for RNA viruses (e.g., HIV, HCV).
Clinical Molecular Dx - Pathogen Spotting
- Directly detects pathogen-specific nucleic acids (DNA/RNA) in clinical samples for diagnosis and management.
- Key Techniques:
- Polymerase Chain Reaction (PCR): Amplifies DNA (e.g., M. tuberculosis).
- Reverse Transcriptase PCR (RT-PCR): For RNA targets (e.g., HIV, HCV, Influenza, COVID-19).
- Nucleic Acid Amplification Tests (NAATs): General term for amplification methods.
- Sequencing: Genotyping, identifying resistance mutations (e.g., HIV drug resistance).
- Applications & Examples:
- Tuberculosis (TB):
⭐ Cartridge-Based Nucleic Acid Amplification Tests (CBNAAT), like GeneXpert, provide rapid, point-of-care diagnosis for diseases such as Tuberculosis (detecting M. tuberculosis and rifampicin resistance).
- HIV: Viral load (RT-PCR), genotypic resistance testing.
- HCV: Genotyping for therapy guidance, viral load.
- HPV: Detection and typing for cervical cancer screening.
- COVID-19: Rapid diagnosis via RT-PCR.
- Tuberculosis (TB):
- Advantages: High sensitivity & specificity, rapid results, detects non-culturable/fastidious organisms, antimicrobial resistance profiling.
- Limitations: Higher cost, infrastructure needs, potential for false positives (contamination), may detect non-viable organisms.
High‑Yield Points - ⚡ Biggest Takeaways
- PCR is the workhorse for detecting viral/bacterial nucleic acids (e.g., HIV, MTB).
- Real-time PCR (qPCR) quantifies pathogen load, crucial for monitoring treatment efficacy.
- Multiplex PCR allows simultaneous detection of several pathogens, useful for syndromic diagnosis.
- NAATs offer superior sensitivity/specificity over culture for many organisms.
- Genotyping/Sequencing is vital for drug resistance profiling and epidemiological tracking.
- Probes are essential for specific target sequence identification in various assays.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

