Introduction to Genetic Counseling - Genes & Guidance
- Definition: A communication process addressing human problems associated with the occurrence, or risk of occurrence, of a genetic disorder in a family.
- Core Goals:
- Help individuals/families comprehend medical facts (diagnosis, prognosis, management).
- Appreciate inheritance patterns & recurrence risk (e.g., 25% for autosomal recessive).
- Understand available options for dealing with risk.
- Make informed choices and appropriate adjustments.
- Crucial for India: Addresses high rates of consanguinity, β-thalassemia.
⭐ Genetic counseling is fundamentally non-directive, empowering individuals and families to make autonomous decisions consistent with their own values and beliefs.
Indications for Genetic Counseling - When To Refer
- Family history of known/suspected genetic disorder.
- Previous child with birth defect, intellectual disability, or genetic condition.
- Advanced maternal age (AMA >35 yrs); advanced paternal age (APA >40 yrs).
- Recurrent pregnancy loss (≥2-3 miscarriages) or unexplained infertility.
- Consanguinity (parents related by blood).
- Significant teratogen exposure during pregnancy.
- Abnormal prenatal screening results or ultrasound findings.
- Personal or family history suggestive of hereditary cancer syndrome.
- Before undergoing or after receiving results of genetic testing.
- Child with developmental delay, dysmorphic features, or congenital anomalies.
⭐ Advanced maternal age (>35 yrs) is a key indication for prenatal genetic counseling.
Components of Counseling Session - The Patient Journey
- Initial Phase:
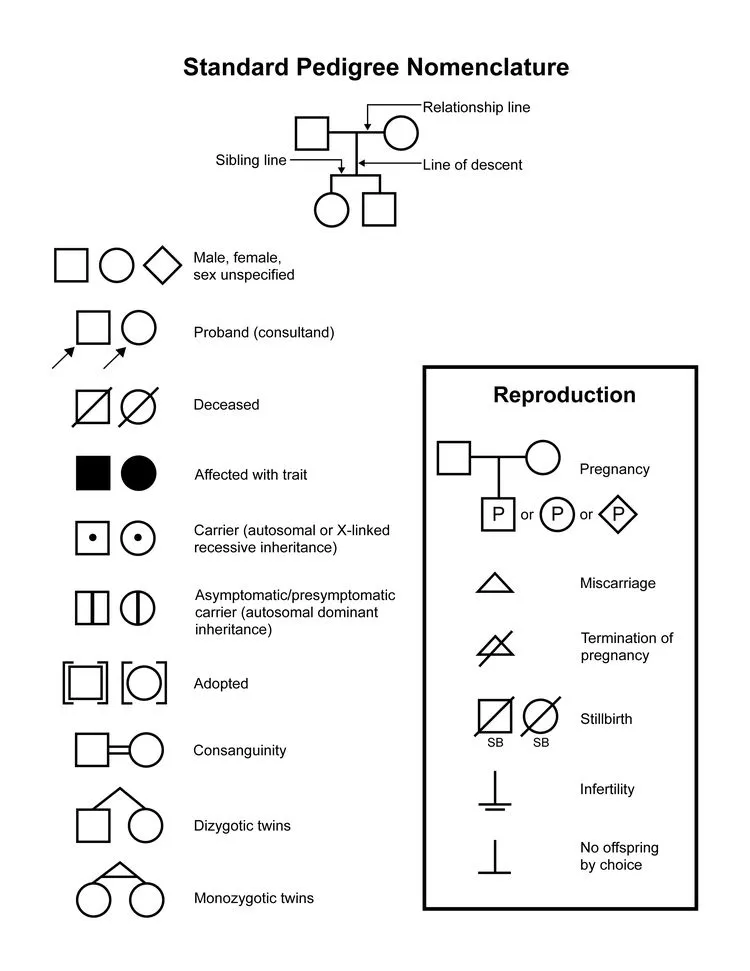
- Referral, history (medical, family - 3-gen pedigree).
- Pre-Test Counseling:
- Risk assessment, genetic education.
- Test options (benefits, limits, implications), informed consent.
- Testing Phase (if applicable):
- Sample collection (e.g., blood, saliva), lab analysis.
- Post-Test Counseling:
- Result disclosure & interpretation.
- Management strategies, psychosocial support.
- Family implications & communication.
- Long-term follow-up plan.
⭐ Pedigree construction is a cornerstone of genetic counseling, typically extending to at least three generations to identify patterns of inheritance.
Risk Assessment Methods - Calculating Chances
- Pedigree Analysis: Visualizes inheritance patterns; crucial for initial assessment.
- Helps determine mode of inheritance (e.g., AD, AR, X-linked).
- Bayesian Calculation: Refines pre-test (prior) probabilities using additional information (e.g., test results, unaffected relatives) to yield post-test (posterior) probability.
- Recurrence Risks (RR) per pregnancy:
- Autosomal Dominant (AD): $50%$ if one parent is affected. New mutations are possible.
- Autosomal Recessive (AR): $25%$ if both parents are carriers.
- X-linked Recessive (XLR): For a carrier mother:
- Sons: $50%$ risk of being affected.
- Daughters: $50%$ risk of being carriers.
⭐ For an autosomal recessive condition, if parents have an affected child, the recurrence risk for each subsequent pregnancy is $25%$.
ELSI in Genetic Counseling - Dilemmas & Duties
- Ethical: Principles (📌 ABNJ: Autonomy, Beneficence, Non-maleficence, Justice). Dilemmas: confidentiality vs. duty to warn; incidentalomas.
- Legal: Informed consent is paramount. 🇮🇳 PCPNDT Act (prohibits sex selection). Anti-discrimination laws.
- Social: Stigma, family dynamics, reproductive choices.
- Implications/Duties: Non-directive counseling, respect patient choices, uphold privacy.
⭐ The PCPNDT Act, 1994, aims to curb female feticide in India by regulating prenatal diagnostic techniques.
High‑Yield Points - ⚡ Biggest Takeaways
- Pedigree analysis is key for identifying inheritance patterns (e.g., AD, AR, X-linked).
- Recurrence risk calculation for single-gene disorders is a primary goal of genetic counseling.
- Bayesian analysis modifies prior genetic risks using additional family or test information.
- Non-directive counseling is the ethical standard, emphasizing patient autonomy in decision-making.
- Key indications include positive family history, advanced maternal age (>35 years), and consanguinity.
- Carrier screening identifies asymptomatic heterozygotes for common recessive disorders like thalassemia or cystic fibrosis.
- Understanding concepts like variable expressivity and incomplete penetrance is crucial for accurate risk assessment and counseling.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more