Biliary Atresia - Bile Duct Blockade
Progressive fibro-obliteration of extrahepatic biliary tree causing bile flow obstruction. Commonest cause of surgical neonatal jaundice.
- Types (Kasai):
- Type I: Common bile duct.
- Type II: Common hepatic duct.
- Type III: Porta hepatis (most common, ~90%).
- Clinical: Jaundice (>2 wks), acholic stools, dark urine, hepatomegaly.
- Diagnosis:
- ↑ Direct bilirubin, ↑ GGT.
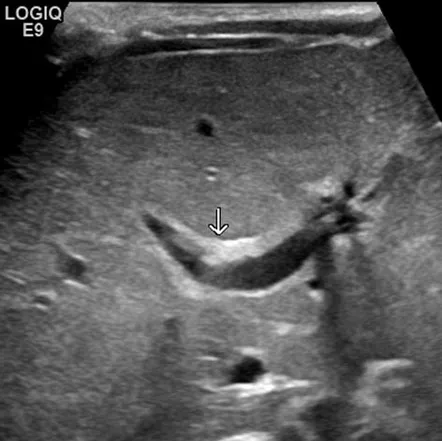
- Ultrasound: Triangular cord sign.
⭐ Triangular cord sign on US is highly suggestive.
- HIDA scan: No bowel excretion.
- Liver biopsy: Ductular proliferation, fibrosis.
- Intraoperative cholangiogram (gold standard).
- Management:
- Kasai portoenterostomy (ideal <60-90 days).
- Liver transplant (failed Kasai/late).
- Complications: Cholangitis, portal HTN, cirrhosis.
Neonatal Cholestasis & Hepatitis - When Yellow Spells Trouble
- Definition: Jaundice >14 days + conjugated hyperbilirubinemia (CB >1 mg/dL or >20% of Total Bilirubin).
- Etiology:
- Obstructive: Biliary Atresia (BA), choledochal cyst.
- Intrahepatic:
- Idiopathic Neonatal Hepatitis (INH): Commonest; giant cells on biopsy.
- Infections (TORCH), Metabolic (A1AT def.).
- Clinical: Jaundice, dark urine, acholic stools, hepatomegaly.
- Investigations: LFTs (↑CB, ↑GGT), USG, HIDA, Liver Biopsy.
⭐ GGT markedly ↑ in Biliary Atresia (>300 IU/L), helps differentiate from Neonatal Hepatitis.
- Management: Treat cause. Supportive: MCT oil, Vitamins A,D,E,K, UDCA.

Metabolic Liver Diseases - Enzyme Errors Wreak Havoc
- Inherited enzyme defects disrupting liver metabolism, leading to organ damage.
- Wilson's Disease: ATP7B gene defect → ↓copper (Cu) excretion. Kayser-Fleischer rings, ↑urinary Cu. Tx: Chelators (e.g., Penicillamine, Trientine).
- Hereditary Hemochromatosis: HFE gene defect → ↑iron (Fe) absorption. "Bronze diabetes", cirrhosis, cardiomyopathy. ↑Ferritin, ↑transferrin saturation. Tx: Phlebotomy.
- Alpha-1 Antitrypsin (A1AT) Deficiency: SERPINA1 gene defect → misfolded A1AT protein accumulates in hepatocytes (PAS+ globules, diastase-resistant). Results in cirrhosis & emphysema.
- Galactosemia: Galactose-1-Phosphate Uridyltransferase (GALT) enzyme deficiency → galactose-1-phosphate accumulation. Jaundice, hepatomegaly, cataracts, E. coli sepsis in neonates. Tx: Lactose/galactose-free diet.

⭐ Alpha-1 Antitrypsin deficiency characteristically shows PAS-positive, diastase-resistant globules, typically found in periportal hepatocytes.
Syndromic & Structural Conditions - When Liver's Not Alone
- Alagille Syndrome (ALGS): AD; JAG1/NOTCH2. Paucity of intrahepatic bile ducts.
- Key: Cardiac (pulm. stenosis), skeletal (butterfly vertebrae), ocular (post. embryotoxon), characteristic facies. 📌 5 major criteria (cardiac, skeletal, ocular, facial, liver).
⭐ Liver biopsy: paucity of interlobular bile ducts (<0.5 bile ducts/portal tract).
- Caroli Disease: AR; PKHD1. Saccular intrahepatic bile duct dilatation.
- "Central dot sign" (portal vein in dilated duct) on imaging.
- Risks: cholangitis, stones, cholangiocarcinoma.
- Caroli Syndrome: Caroli disease + Congenital Hepatic Fibrosis (CHF) → portal HTN.
- Congenital Hepatic Fibrosis (CHF): AR; PKHD1. Portal fibrosis, abnormal portal veins.
- Portal HTN (varices), preserved LFTs initially. Assoc. ARPKD.
- Biliary Atresia Splenic Malformation (BASM): Biliary atresia + splenic/laterality defects (e.g., asplenia, situs inversus).

High‑Yield Points - ⚡ Biggest Takeaways
- Gilbert's syndrome: Mild unconjugated hyperbilirubinemia due to UGT1A1 mutation.
- Crigler-Najjar Type I: Severe unconjugated hyperbilirubinemia, absent UGT, kernicterus. Type II responds to phenobarbital.
- Dubin-Johnson syndrome: Conjugated hyperbilirubinemia, black liver, defective MRP2.
- Rotor syndrome: Conjugated hyperbilirubinemia, no liver pigmentation, defective OATP1B1/3.
- Alagille syndrome: Paucity of bile ducts, butterfly vertebrae, pulmonary stenosis.
- Biliary atresia: Neonatal cholestasis, acholic stools, Kasai procedure needed.
- Congenital hepatic fibrosis: Linked to ARPKD, causes portal hypertension.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

