Wound Healing - Stitching Stories
Restoration of tissue architecture & function post-injury.
- Healing Types:
- Regeneration: Complete tissue restitution; original structure restored.
- Repair: Patching with connective tissue; scar formation.
| Feature | Primary Intention | Secondary Intention |
|---|---|---|
| Edges | Clean, apposed (sutured) | Not apposed, large defect |
| Infection Risk | Low | High |
| Granulation | Minimal | Abundant |
| Contraction | Minimal | Marked (myofibroblasts) |
| Scar | Small, neat | Large, irregular |
| Duration | Faster | Slower |
⭐ Wound strength reaches ~70-80% of normal skin by 3 months, mainly due to Type I collagen deposition and remodeling.
Wound Healing - Repair Relay
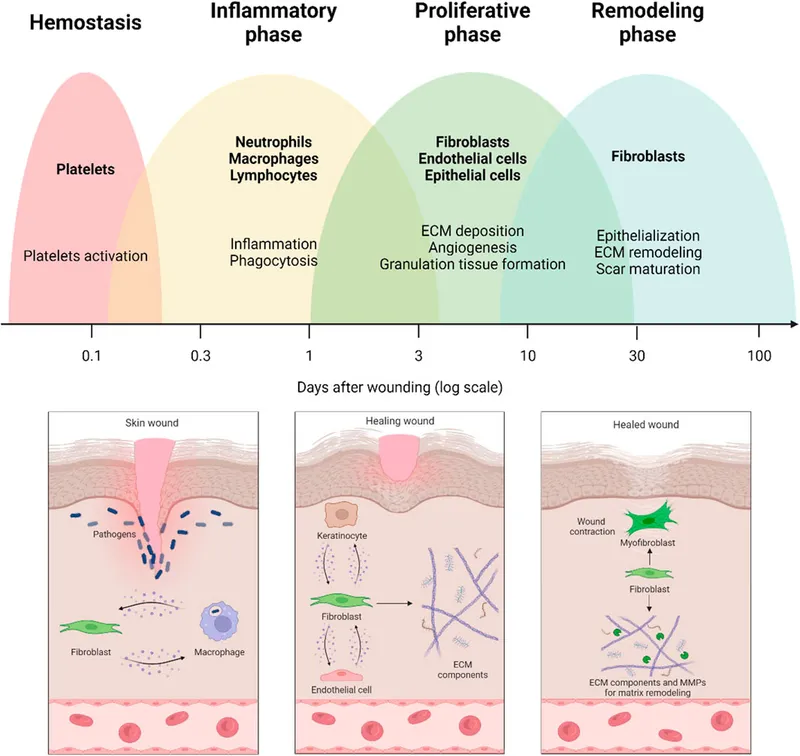
- 1. Hemostasis & Inflammation (0-3 days)
- Cells: Platelets (clot), Neutrophils (PMNs; debris removal ~24-48h), Macrophages (phagocytosis, growth factors).
- Events: Vasoconstriction, platelet plug, coagulation, inflammation.
- 2. Proliferation (3 days - 3 weeks)
- Cells: Fibroblasts (Collagen Type III), Endothelial cells (angiogenesis), Keratinocytes (epithelialization).
- Events: Granulation tissue, neovascularization, re-epithelialization, wound contraction (myofibroblasts).
- 3. Maturation & Remodeling (3 weeks - 2 years)
- Cells: Fibroblasts.
- Events: Collagen Type III → Type I, ↑ cross-linking & tensile strength, scar maturation, vascular regression.
⭐ Wound tensile strength reaches ~70-80% of normal skin by 3 months. The critical switch from Type III to Type I collagen occurs during remodeling.
Wound Healing - Cellular Crew
-
Key Cells & Timeline:
- Platelets (Seconds-Hours): Hemostasis, release growth factors (PDGF, TGF-β).
- Neutrophils (24-48 hrs): Phagocytosis, debris removal.
- Macrophages (48-96 hrs → weeks):
- M1: Pro-inflammatory, phagocytosis.
- M2: Anti-inflammatory, repair, angiogenesis (VEGF), fibroblast activation (TGF-β, PDGF).
- Lymphocytes (Week 1 onwards): Immune modulation.
- Fibroblasts/Myofibroblasts (Day 3 → weeks): Collagen (Type III then I) synthesis, wound contraction.
- Endothelial Cells (Day 3 → weeks): Angiogenesis (VEGF, FGF).
- Keratinocytes (Day 1 → weeks): Re-epithelialization (EGF, KGF).
-
Key Growth Factors:
- PDGF: Platelets, MΦ; chemotaxis, proliferation (fibroblasts, smooth muscle).
- FGF (FGF-2): MΦ, fibroblasts; angiogenesis, fibroblast proliferation, ECM deposition.
- TGF-β: Platelets, MΦ, fibroblasts; ↑collagen synthesis, ↓MMP activity, fibrosis.
- VEGF: MΦ, endothelial cells; angiogenesis, ↑vascular permeability.
- EGF/KGF: Platelets, MΦ, keratinocytes; keratinocyte migration, proliferation.
-
ECM Dynamics:
- Components: Collagen (Type III → Type I), Elastin, Proteoglycans, Fibronectin.
- Remodeling: Matrix Metalloproteinases (MMPs) degrade ECM; Tissue Inhibitors of Metalloproteinases (TIMPs) regulate MMPs.
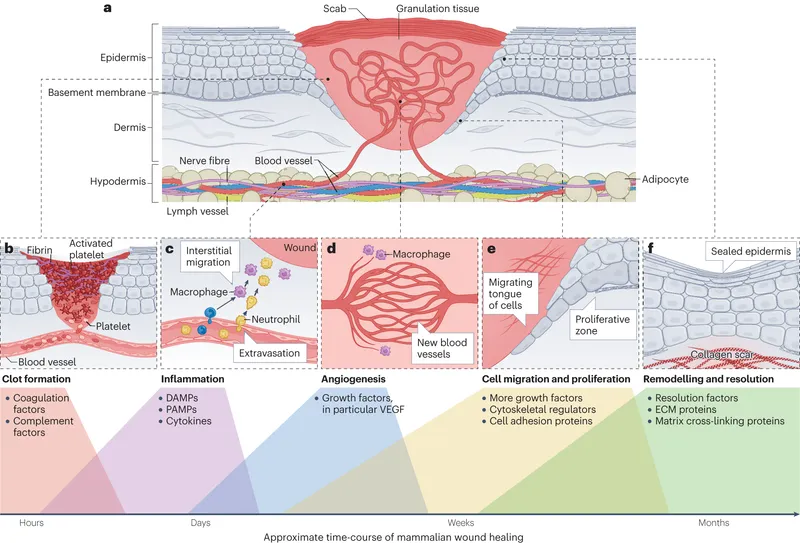
⭐ Type III collagen is predominant in early granulation tissue (first few days), later replaced by stronger Type I collagen (by week 2-3). Ratio of Type I to Type III collagen increases as the wound matures. 📌 Three comes before One in Tissue repair (Type III then Type I).
Wound Healing - Boosters & Blockers
- Systemic Factors:
- Boosters: Good nutrition (Protein, Vit C, Zinc, Copper).
- Blockers: Advanced age, Diabetes (DM), Glucocorticoids, Chemotherapy, Poor perfusion (PVD, shock), Anemia, Immunosuppression, Smoking.
- Local Factors:
- Boosters: Good blood supply, clean wound, appropriate closure.
- Blockers: Infection (most common delay), Mechanical stress (movement, tension), Foreign bodies, Ischemia, Necrosis, Large size/poor location, Radiation.
⭐ Infection is the single most common and important cause of delayed wound healing.
Wound Healing - Repair Mishaps
- Deficient Scar Formation:
- Dehiscence: Wound rupture, often post-surgery.
- Ulceration: Inadequate vascularization during healing.
- Excessive Scar Formation:
-
Hypertrophic Scar: ↑ Type I collagen; confined to original wound boundaries.
-
Keloid: ↑ Type I & III collagen; grows beyond original boundaries; genetic link.
⭐ Keloids are particularly common in individuals of African descent and frequently recur after excision.
-
- Exuberant Granulation (Proud Flesh): Excessive granulation tissue; protrudes, blocking re-epithelialization.
- Contractures: Exaggerated wound contraction leading to deformities (e.g., palms, soles, post-burns).
High‑Yield Points - ⚡ Biggest Takeaways
- Primary intention: Clean edges, minimal scar. Secondary: Large defect, granulation, myofibroblast contraction, marked scar.
- Healing: Inflammation (PMNs, Mφ), Proliferation (Type III collagen, granulation), Maturation (Type I collagen, ↑strength).
- Keloids grow beyond wound margins; Hypertrophic scars stay confined. Both = excess collagen.
- Infection is the #1 cause of impaired healing.
- Vitamin C (collagen synthesis) & Zinc vital for repair.
- Tensile strength: ~70-80% original strength by 3 months; never 100%.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

