Definition & Cells - Granuloma Fortress Intro
- Granuloma: A focal, organized collection of activated macrophages (epithelioid cells), typically surrounded by a lymphocytic rim. Represents a chronic inflammatory response.
- Purpose: To contain or "wall off" persistent, poorly digestible injurious agents (e.g., M. tuberculosis, fungi, foreign material).
- Cellular "Bricks" of the Fortress:
- Epithelioid Macrophages: Activated, modified macrophages; hallmark. Elongated, pale eosinophilic cytoplasm, indistinct cell borders.
- Multinucleated Giant Cells (MGCs): Formed by fusion of epithelioid cells.
- Langhans type: Nuclei arranged peripherally (horseshoe/ring).
- Foreign body type: Nuclei scattered haphazardly.
- Lymphocytes: Predominantly T-cells (CD4+ > CD8+), forming a collar.

⭐ The presence of epithelioid cells is the defining histological feature of a granuloma.
Types & Classification - Granuloma Varieties
- Immune Granulomas:
- T-cell (CD4+ Th1) mediated; Type IV hypersensitivity.
- Response to persistent, poorly soluble antigens.
- Subtypes:
- Caseating Granulomas:
- Central amorphous, eosinophilic necrosis. 📌 "Caseous = Cheesy necrosis".
- Examples: Tuberculosis (classic), Fungal (Histoplasma, Coccidioides), Syphilis (gumma).
- Key: Loss of cellular detail in center.
- Non-caseating Granulomas:
- No central necrosis; cells intact.
- Examples: Sarcoidosis, Crohn's disease, Tuberculoid leprosy, Berylliosis.
-
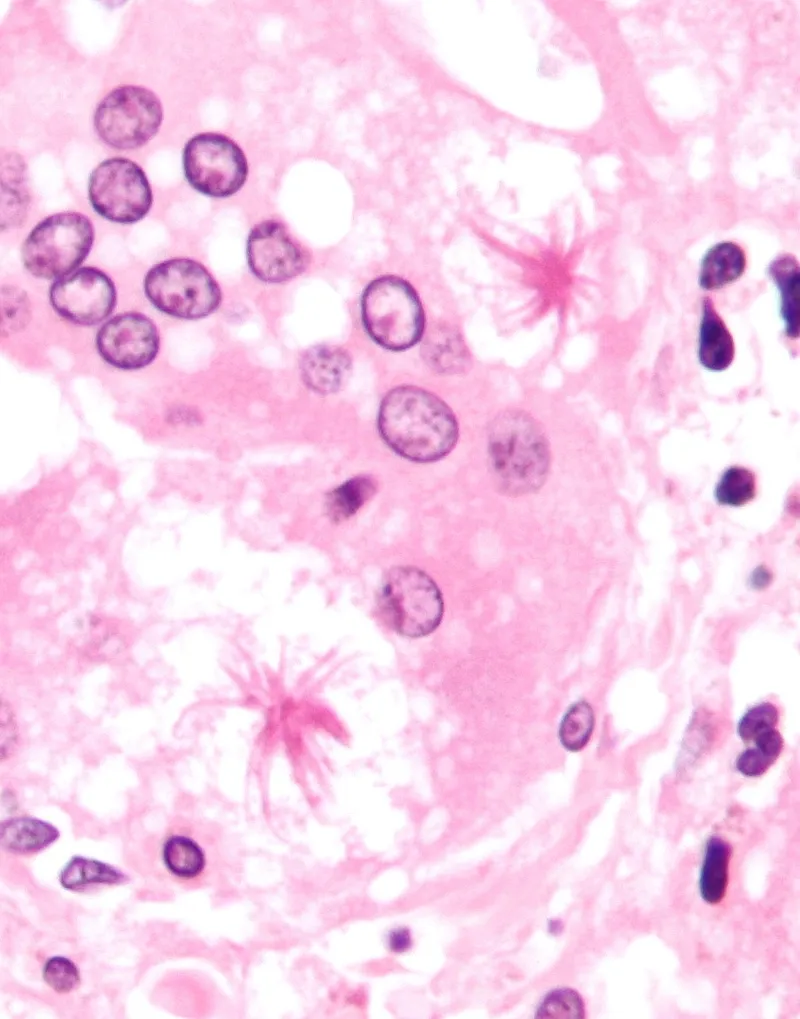
⭐ In Sarcoidosis, look for Schaumann bodies (laminated calcium concretions) & Asteroid bodies (stellate inclusions within giant cells).
- Caseating Granulomas:
- Foreign Body Granulomas:
- Reaction to inert materials (e.g., sutures, talc, silica, splinters).
- Material often visible (may be birefringent under polarized light).
- Foreign body giant cells engulf material; less lymphocytic infiltrate.
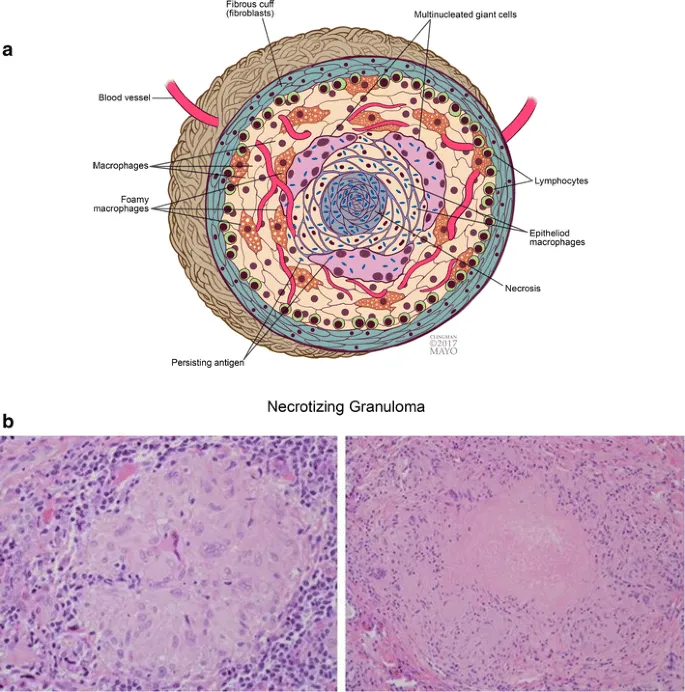
Pathogenesis - Making a Granuloma
- Initiation: Caused by indigestible antigens (e.g., M. tuberculosis, fungal hyphae, suture material) or T-cell mediated hypersensitivity.
- Mechanism - Immune Granuloma Formation:
- Key Mediators & Cells:
- Macrophages: Activated by IFN-γ, transform into:
- Epithelioid cells: Elongated, pink cytoplasm; primary function is secretion.
- Giant cells: Fusion of epithelioid cells (e.g., Langhans, foreign body type).
- CD4+ Th1 cells: Orchestrate response via IFN-γ.
- Cytokines:
- IFN-γ: Prime macrophage activator.
- TNF-α: Essential for recruiting macrophages and maintaining granuloma structure.
- IL-12: Drives Th1 differentiation.
- Macrophages: Activated by IFN-γ, transform into:
⭐ TNF-α inhibitors, used for autoimmune diseases, can disrupt granulomas and lead to reactivation of latent tuberculosis.
Associated Diseases - Granuloma Rogues' Gallery
- Infectious:
- Bacterial:
- Tuberculosis (TB): Caseating necrosis; Langhans giant cells. AFB positive.
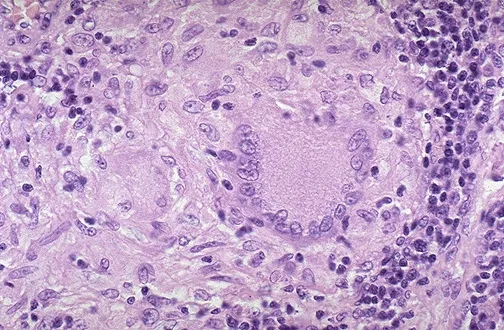
- Leprosy: Tuberculoid (non-caseating), Lepromatous (foamy macrophages).
- Syphilis (tertiary): Gumma (central coagulative necrosis).
- Cat-scratch disease (Bartonella henselae): Stellate, necrotizing granulomas.
- Tuberculosis (TB): Caseating necrosis; Langhans giant cells. AFB positive.
- Fungal: (e.g., Histoplasmosis, Coccidioidomycosis, Blastomycosis): Caseating or non-caseating. PAS/GMS+.
- Parasitic: (e.g., Schistosomiasis): Granulomas around ova; eosinophils.
- Bacterial:
- Non-Infectious:
- Immune-Mediated:
- Sarcoidosis: Non-caseating. Bilateral hilar lymphadenopathy. Schaumann/Asteroid bodies. ↑Serum ACE.
- Crohn's Disease: Non-caseating granulomas in bowel wall.
- Granulomatosis with Polyangiitis (Wegener's): Necrotizing; respiratory tract, kidneys; c-ANCA+.
- Sarcoidosis: Non-caseating. Bilateral hilar lymphadenopathy. Schaumann/Asteroid bodies. ↑Serum ACE.
- Foreign Body: (e.g., Sutures, talc, beryllium-Berylliosis): Around material.
- Idiopathic: (e.g., Granuloma annulare): Dermal.
- Immune-Mediated:
⭐ Sarcoidosis is a multisystem disorder characterized by non-caseating epithelioid granulomas, frequently involving bilateral hilar lymphadenopathy and elevated serum Angiotensin-Converting Enzyme (ACE).
High‑Yield Points - ⚡ Biggest Takeaways
- Granulomatous inflammation: Chronic inflammation with aggregates of epithelioid macrophages.
- Features epithelioid histiocytes, Langhans and Foreign body giant cells.
- Caseating granulomas (e.g., Tuberculosis) have central necrosis; Non-caseating (e.g., Sarcoidosis) do not.
- Mediated by Type IV hypersensitivity; IFN-γ from Th1 cells is crucial.
- Key causes: Tuberculosis, Sarcoidosis, fungal infections, Crohn's disease, leprosy.
- Look for Schaumann and Asteroid bodies in Sarcoidosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

