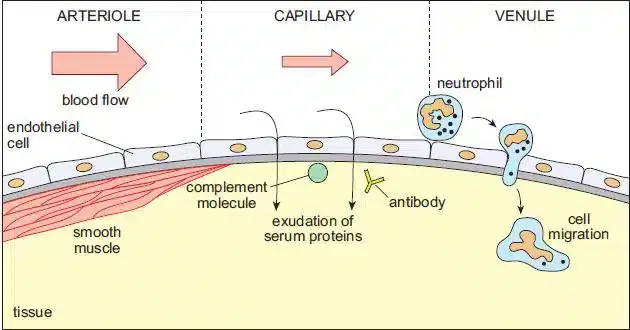
Introduction & Cardinal Signs - Red Carpet Rollout
- Acute inflammation: Rapid defense; delivers leukocytes & plasma proteins to injury.
- Hallmarks: Vascular changes (the "red carpet") causing visible signs.
- Cardinal Signs (Celsus & Virchow):
- Rubor (Redness): Vasodilation (e.g., histamine).
- Tumor (Swelling): ↑ Vascular permeability, fluid exudation.
- Calor (Heat): ↑ Blood flow.
- Dolor (Pain): Mediators (bradykinin, $PGE_2$), tissue tension.
- Functio laesa (Loss of function): Result of other signs.
📌 Mnemonic: PRISH (Pain, Redness, Immobility, Swelling, Heat).
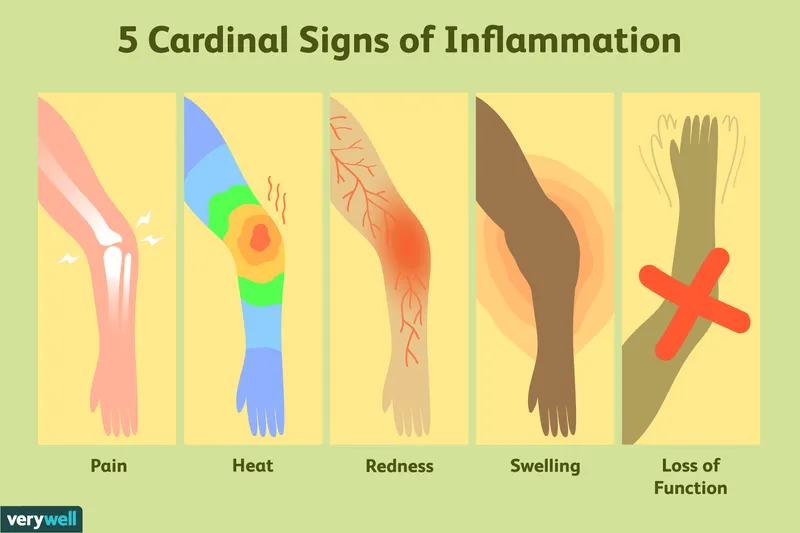
⭐ Celsus described the first four signs (rubor, tumor, calor, dolor); Virchow added the fifth, Functio laesa.
Vasodilation - Pipes Wide Open
- Initial, brief vasoconstriction (neurogenic; endothelin).
- Followed by sustained vasodilation:
- Primarily affects arterioles; later opens new capillary beds.
- Key Mediators:
- Histamine & Serotonin (early; from mast cells, platelets).
- Nitric Oxide (NO) (from endothelium via eNOS).
- Bradykinin.
- Prostaglandins (PGI₂, PGE₂, PGD₂).
- Mechanism: Relaxation of vascular smooth muscle.
- Results:
- ↑ Blood flow (active hyperemia) to the affected area.
- Causes cardinal signs: Rubor (redness) & Calor (heat).
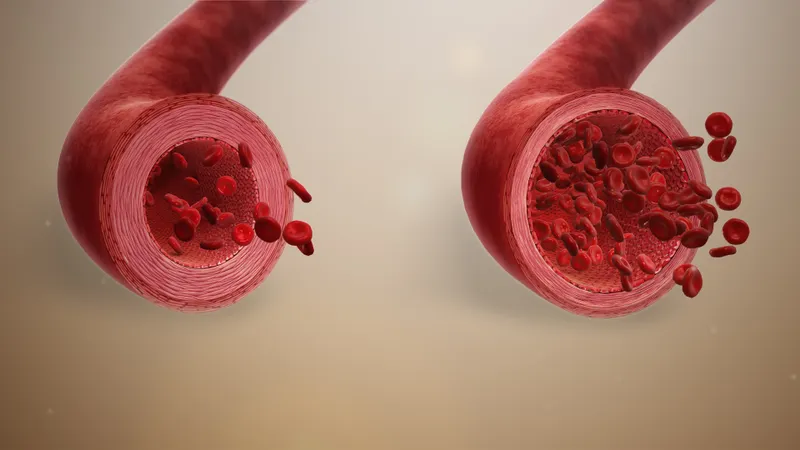
⭐ Histamine is a principal mediator of the immediate transient phase of increased vascular permeability and vasodilation, released mainly from mast cells, basophils, and platelets in response to various stimuli.
Increased Vascular Permeability - Leaky Vessels Ahoy!
Key to acute inflammation, allowing plasma proteins & leukocytes to exit vessels. Leads to exudate & edema.
- Mechanisms:
- Endothelial Cell Contraction (Most Common):
- Mediators: Histamine, bradykinin, leukotrienes (C4, D4, E4), Substance P.
- Rapid, short-lived (15-30 min).
- Mainly affects venules.
- Forms intercellular gaps.
- Endothelial Injury:
- Direct: Burns, toxins, trauma.
- Leukocyte-mediated: During adhesion/emigration.
- Rapid or delayed onset; prolonged duration.
- Affects arterioles, capillaries, venules.
- Transcytosis:
- ↑ Vesicular transport across cytoplasm.
- Mediator: Vascular Endothelial Growth Factor (VEGF).
- Mainly venules.
- Leakage from New Blood Vessels:
- During repair (angiogenesis); immature vessels are leaky.
- Endothelial Cell Contraction (Most Common):
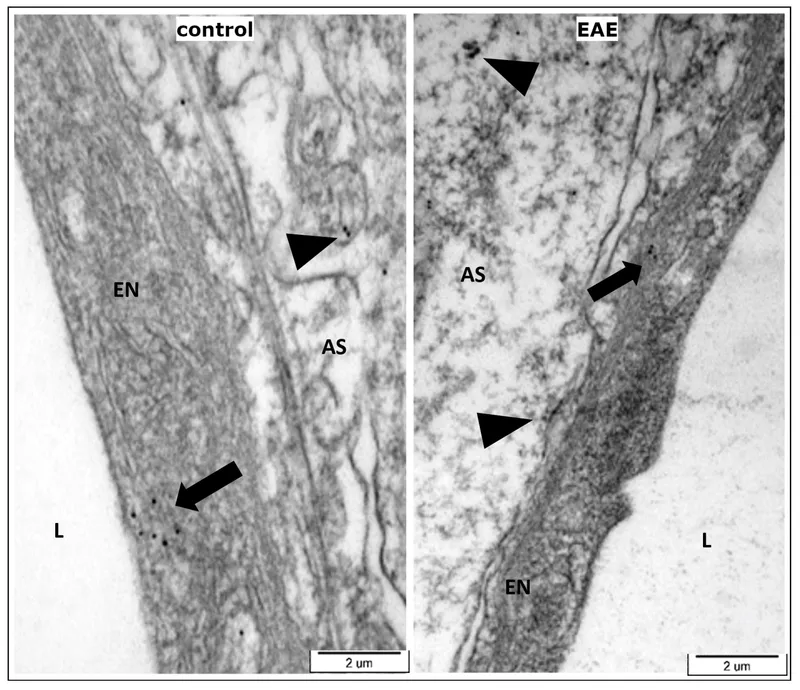
⭐ Exam Favourite: The most common mechanism of increased vascular permeability is endothelial cell contraction, primarily mediated by histamine, leading to transient leakage in venules.
Stasis & Exudation - Slowing & Spilling
- Stasis: Marked slowing of blood circulation in microvasculature.
- Mechanism: ↑ vascular permeability → loss of protein-rich fluid from plasma → ↑ blood viscosity & concentration of RBCs.
- Result: Small vessels become packed with slow-moving RBCs.
- Exudation: Escape of fluid, proteins, and blood cells from the vascular system into interstitial tissue or body cavities.
- Exudate: Inflammatory extravascular fluid with high protein content (specific gravity > 1.020), cellular debris. Often contains fibrinogen (→ fibrin).
- Significance: Implies significant alteration in small vessel permeability.
- Contrast: Transudate is low protein fluid (specific gravity < 1.012), an ultrafiltrate of plasma, due to hydrostatic imbalance, not permeability change.
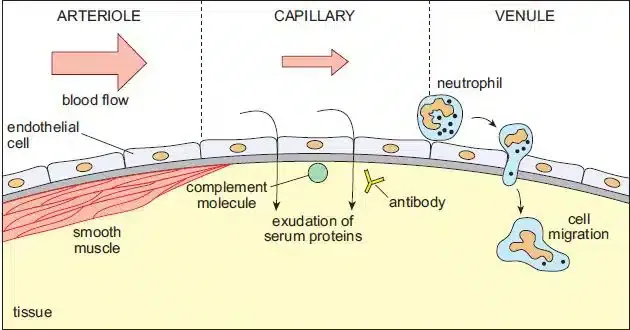
⭐ Accumulation of protein-rich exudate leads to swelling (tumor), a cardinal sign of acute inflammation.
Edema Formation - Puffing Up
- Fluid accumulation in interstitial tissue, causing swelling (tumor).
- Pathophysiology: Altered Starling forces.
- ↑ Hydrostatic pressure (capillary): Due to arteriolar dilation & ↑ blood flow.
- ↓ Colloid osmotic pressure (plasma): Due to protein leakage (albumin) from ↑ vascular permeability.
- Net result: ↑ Outward movement of fluid from capillaries into interstitium.
⭐ Inflammatory edema is typically an exudate: protein-rich (specific gravity >1.020, protein >2.5-3 g/dL) with inflammatory cells.
High‑Yield Points - ⚡ Biggest Takeaways
- Vasodilation (mediated by histamine, NO) causes rubor (redness) and calor (heat).
- Increased vascular permeability (driven by histamine, leukotrienes) leads to protein-rich exudate and edema (tumor).
- Endothelial cell contraction in post-capillary venules is the main mechanism for early, transient leakage.
- Stasis of blood flow, due to fluid loss, concentrates red blood cells, facilitating leukocyte margination.
- Exudate (SG > 1.020, protein > 2.5 g/dL) indicates inflammation, unlike transudate.
- The Triple Response of Lewis (flush, flare, wheal) demonstrates key histamine-mediated vascular events in skin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more