Specimen Handling - Get It Right!
- Aseptic technique is crucial. Collect before antimicrobials.
- 📌 5 Rights: Right Patient, Right Site, Right Time, Right Specimen, Right Container.
- Adequate quantity essential. Label meticulously: Name, ID, Date, Time, Site.
- Transport ASAP. Use transport media (e.g., Stuart's, Amies) if delay >2h.
- Special handling: Anaerobes (anaerobic vial), Viruses (VTM).

⭐ For suspected bacteremia, collect 2-3 blood culture sets (aerobic & anaerobic bottles each) from different sites before antibiotics administration to maximize yield and guide therapy effectively.
Microscopy & Stains - Stain & See
- Foundation of rapid diagnosis; initial pathogen clues.
- Gram Stain: Differentiates bacteria based on cell wall.
- Gram +ve: Purple/Violet (e.g., Staphylococcus, Streptococcus)
- Gram -ve: Pink/Red (e.g., E. coli, Klebsiella)
- 📌 Positive Purple, Negative piNk.
- Ziehl-Neelsen (ZN) Stain: For acid-fast bacilli (AFB).
- Mycobacterium tuberculosis (red bacilli, blue background).
- Modified ZN: Nocardia, Cryptosporidium.
- KOH Mount ($10-20%$): Visualizes fungal elements (hyphae, yeasts) by dissolving host cells.
- India Ink: Negative stain for capsules, classically Cryptococcus neoformans.
- Giemsa Stain: For blood parasites (Malaria, Leishmania), Chlamydia inclusions, Borrelia.
- Albert's Stain: Detects metachromatic granules in Corynebacterium diphtheriae.
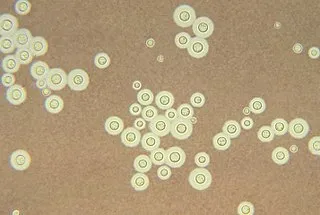
⭐ Ziehl-Neelsen stain uses carbolfuchsin (primary stain), heat (mordant), acid-alcohol (decolorizer), and methylene blue (counterstain).
Culture Methods - Growth & ID
- Goal: Isolate, ID microbes, & enable Antimicrobial Susceptibility Testing (AST). Gold standard for many infections.
- Culture Media Types:
- Basal: e.g., Nutrient agar, Peptone water.
- Enriched: Blood Agar (BA), Chocolate Agar (CA for Haemophilus, Neisseria).
- Selective: MacConkey (Gram-neg), Lowenstein-Jensen (LJ for TB), TCBS (Vibrio).
- Differential: MacConkey (Lactose Fermenter/Non-Lactose Fermenter), CLED (urine pathogens).
- Transport: Stuart's, Amies, Cary-Blair (fecal).
- Incubation: Standard 35-37°C; O₂ needs (aerobic; anaerobic - Robertson Cooked Meat (RCM); microaerophilic - Campylobacter; capnophilic - 5-10% CO₂ for Neisseria, Haemophilus).
- Identification: Colony morphology, Gram stain, biochemical tests (catalase, oxidase, IMViC), automated systems (e.g., VITEK).

⭐ For blood cultures, the optimal blood-to-broth ratio is 1:5 to 1:10 to dilute antibacterial substances in blood & improve recovery of organisms.
Immunological Dx - Immune Scope
- Detects host immune response (antibodies, CMI) or microbial antigens.
- Antibody Detection:
- IgM: Acute infection indicator.
- IgG: Past/chronic infection, immunity.
- Seroconversion: Appearance of antibodies.
- Significant rise: ≥4-fold increase in titre (acute vs. convalescent sera).
- Antigen Detection:
- Directly identifies microbial components (e.g., proteins, polysaccharides).
- Enables rapid diagnosis.
- Cell-Mediated Immunity (CMI) Tests:
- E.g., Tuberculin skin test (TST), Interferon-Gamma Release Assays (IGRAs) for TB.
- Techniques: ELISA, Rapid tests (immunochromatography), Immunofluorescence (IF), Agglutination.

⭐ ELISA is a versatile, highly sensitive, and specific technique widely used for detecting either antigens or antibodies, crucial for HIV and Hepatitis diagnosis.
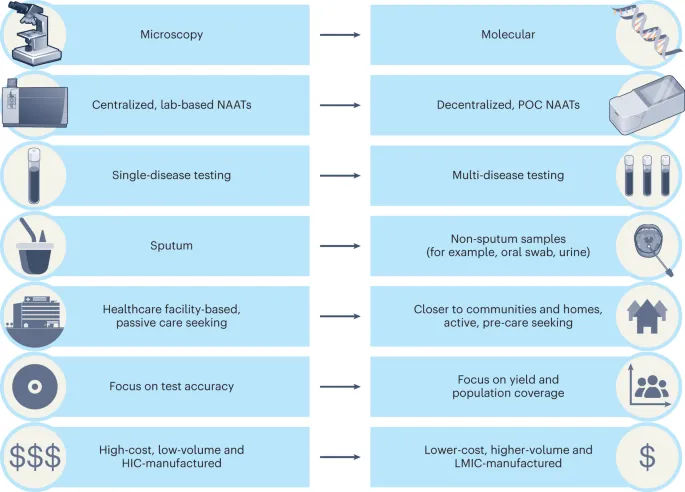
Molecular Techniques - Gene Detectives
Directly detect microbial genetic material (DNA/RNA). They offer high sensitivity, specificity, and rapid results, vital for unculturable or slow-growing pathogens.
- PCR (Polymerase Chain Reaction): Core method for DNA amplification.
- RT-PCR: Detects RNA (e.g., HIV, Influenza).
- qPCR (Real-time PCR): Allows quantification of pathogen load.
- Nucleic Acid Hybridization: Uses labeled probes to find specific DNA/RNA sequences (e.g., FISH).
- Sequencing (e.g., NGS): Determines exact nucleotide order for precise ID, genotyping, resistance.
⭐ PCR can detect as few as 1-10 microbial genomes, revolutionizing diagnosis of infections like TB from paucibacillary samples.
High‑Yield Points - ⚡ Biggest Takeaways
- Gram stain (cell wall) & ZN stain (acid-fast bacilli) are key microscopy tests.
- Culture is gold standard for ID & antibiotic susceptibility testing (AST).
- Serology (antibodies/antigens) indicates infection stage; IgM suggests acute infection.
- Molecular tests (e.g., PCR) offer rapid, sensitive microbial nucleic acid detection.
- India Ink for Cryptococcus (capsule); KOH mount for rapid fungal element detection.
- Optimal blood culture collection (volume, timing, multiple sets) is crucial for sepsis diagnosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

