HAIs: The Unwanted Guests
- Infections acquired during healthcare delivery; manifest >48h post-admission. Not present/incubating at admission.
- Major cause of morbidity & mortality; prevention is crucial (e.g., hand hygiene, bundles).
- Common Types:
- CAUTI (Catheter-Associated UTI): UTI with indwelling catheter >2 days.
- SSI (Surgical Site Infection): Infection post-surgery at/near incision within 30-90 days.
- CLABSI (Central Line-Associated BSI): Lab-confirmed BSI with central line >2 days.
- VAP (Ventilator-Associated Pneumonia): Pneumonia >48-72h post-intubation.
- CDI (C. difficile Infection): Antibiotic-associated diarrhea/colitis.
Key Pathogens: 📌 (Mnemonic: KEEPS CC)
| Category | Pathogens |
|---|---|
| Bacteria | Klebsiella spp., E. coli, Enterococcus (VRE), Pseudomonas aeruginosa, S. aureus (MRSA), C. difficile |
| Fungi | Candida spp. |
Device Drama: CAUTI & CLABSI
Catheter-Associated UTI (CAUTI)
- Def: UTI with indwelling catheter (IUC) or ≤48h post-removal.
- Risk: ↑ IUC duration.
- Pathogens: E. coli (most common), Klebsiella, Proteus, Pseudomonas, Enterococcus, Candida.
- Dx: Symptoms + culture $\ge$10^5 CFU/mL; OR Catheterized: $\ge$10^3 CFU/mL.
- Prevention Bundle: Aseptic insertion, closed drainage, daily review for removal.
⭐ Most common pathogen for CAUTI: Escherichia coli.
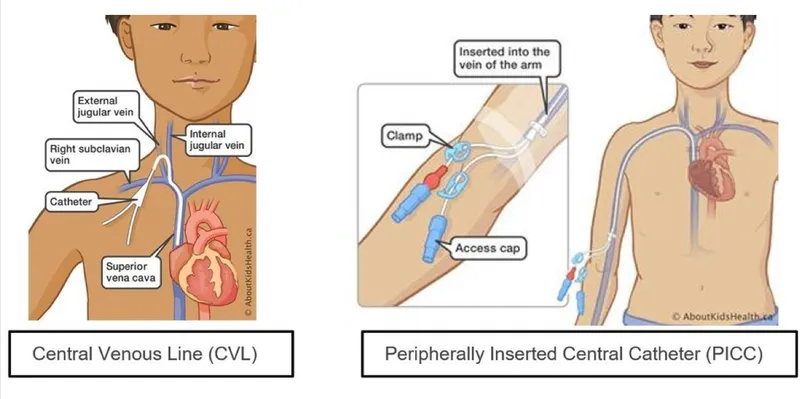
Central Line-Associated Bloodstream Infection (CLABSI)
- Def: Lab-confirmed BSI with central line (CL) or ≤48h post-removal; not from other infection site.
- Risk: ↑ CL duration, insertion site (femoral > jugular > subclavian).
- Pathogens: CoNS (S. epidermidis), S. aureus, Gram-negatives, Candida spp.
- Dx: Blood culture + signs; Differential Time to Positivity (DTP) >2 hours.
- Prevention Bundle: Hand hygiene, CHG prep, full barriers, daily line review.
Infection Hotspots: SSI, VAP, CDI
- Surgical Site Infection (SSI)
- Def: Infection at/near surgical incision within 30 days (no implant) or 90 days (implant).
- Classification: Superficial, Deep, Organ/Space. 📌 SDO.

- Pathogens: S. aureus, CoNS, Enterococcus, Gram-negatives.
- Risk Factors: Obesity, smoking, DM, poor surgical technique, prolonged surgery.
- Prevention: Hand hygiene, skin prep (chlorhexidine), timely antibiotic prophylaxis.
- Ventilator-Associated Pneumonia (VAP)
- Def: Pneumonia developing >48-72h post-endotracheal intubation.

- Pathogens: Pseudomonas aeruginosa, Acinetobacter baumannii, Klebsiella pneumoniae, S. aureus (incl. MRSA).
- Risk Factors: Prolonged ventilation, aspiration, immunosuppression, reintubation, supine position.
- Prevention: Head elevation (30-45°), oral care (chlorhexidine), daily sedation interruption & weaning assessment.
- Def: Pneumonia developing >48-72h post-endotracheal intubation.
- Clostridioides difficile Infection (CDI)
- Pathogen: C. difficile (anaerobic, Gram-positive, spore-forming bacillus).
- Toxins: Toxin A (enterotoxin) & Toxin B (cytotoxin).
- Risk Factors: Antibiotics (clindamycin, cephalosporins, fluoroquinolones), PPIs, ↑age, hospitalization.
- Dx: Stool test for GDH + Toxin; or NAAT.
- Mgmt: Oral vancomycin or fidaxomicin (preferred for recurrence). ⭐ > Key antibiotic historically strongly associated with CDI: Clindamycin.
Germ Warfare: AMR & Defense
⭐ Hand hygiene is the single most effective measure to prevent HAIs.
- Precautions:
- Standard: Apply to ALL patients, assumes all are potentially infectious.
- Transmission-Based: For specific known/suspected pathogens. See flowchart.
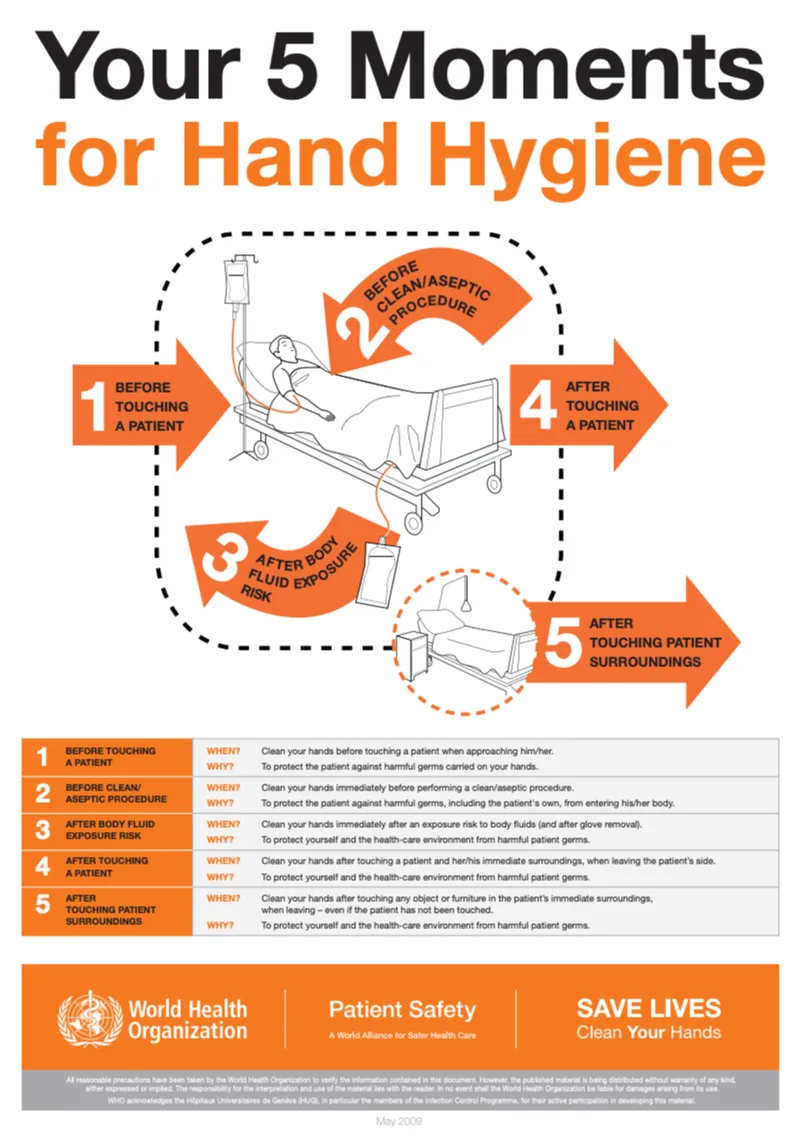
- Hand Hygiene: 📌 WHO 5 Moments: Critical to break transmission. Alcohol rubs preferred.
- Antimicrobial Stewardship (AMS):
- Goals: Optimize antibiotic use, ↓resistance, better outcomes.
- Key Interventions: Formulary, audit, de-escalation, IV-oral switch.
- Environmental Cleaning & Disinfection: Clean patient environment & shared equipment.
- Surveillance of HAIs:
- Purpose: Monitor trends, detect outbreaks, evaluate prevention.
- Methods: Active (lab, ward rounds), passive (codes).
- AMR in HAIs (Key Pathogens):
- MRSA (mecA): Beta-lactam resistant. Skin/soft tissue, pneumonia.
- VRE (vanA/B): Vancomycin-resistant Enterococci. Bloodstream, UTI.
- ESBL-producers (e.g., CTX-M in E.coli, Klebsiella): Resist penicillins, cephalosporins.
- CRE (KPC, NDM, OXA-48): "Superbugs"; limited treatment, high mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Healthcare-Associated Infections (HAIs): Acquired during healthcare delivery, absent upon admission.
- Commonest types: CAUTI, CLABSI, SSI, and VAP.
- Key pathogens include MRSA, Clostridioides difficile (C. diff), and multidrug-resistant organisms like CRE.
- Effective hand hygiene is the most crucial, single measure for HAI prevention.
- Adhere strictly to Standard Precautions and relevant Transmission-Based Precautions.
- Antimicrobial stewardship programs are essential to control emerging resistance.
- Prevention bundles for device-associated infections (e.g., CAUTI, CLABSI) significantly reduce HAI rates.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

