Intro to Emerging - New Kids on Block
- Emerging Infectious Diseases (EIDs): Infections newly appeared in a population or with rapidly ↑ incidence or geographic range.
- Re-emerging EIDs: Diseases reappearing after a significant decline.
- Key Drivers:
- Microbial: Adaptation, mutation (e.g., Influenza antigenic drift/shift).
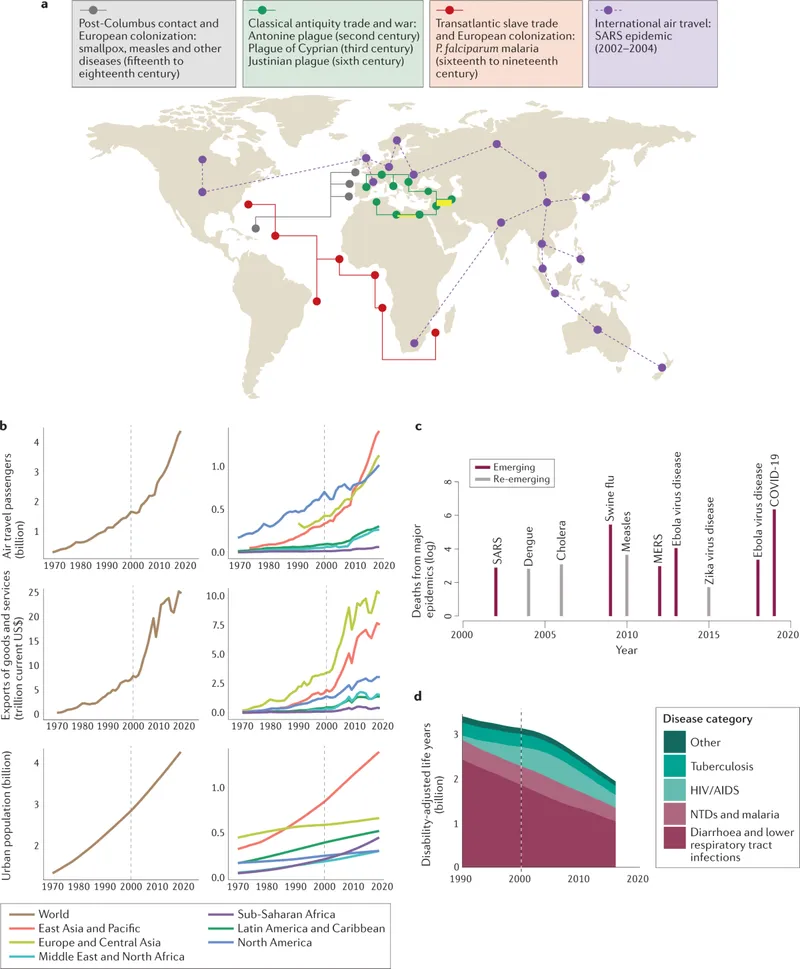
- Human: Demographics (urbanization), behavior (travel).
- Environmental: Climate change, deforestation, agricultural practices.
- Public Health: Breakdown in measures (e.g., ↓ vaccination coverage).
- Zoonotic Spillover: Majority of EIDs (e.g., Nipah, COVID-19, Ebola).
- One Health Concept: Interconnectedness of human, animal, & environmental health is crucial for prevention & control.
⭐ Approximately 75% of recently emerging infectious diseases in humans are of animal origin (zoonoses).
Key Viral Agents - Contagion Chronicles
| Feature | Nipah Virus (NiV) | COVID-19 (SARS-CoV-2) | Zika Virus (ZIKV) |
|---|---|---|---|
| Agent | RNA, Henipavirus | RNA, Sarbecovirus | RNA, Flavivirus |
| Vector | Fruit bats; Pigs; Direct contact | Respiratory droplets, aerosols | Aedes mosquitoes; Sexual, vertical |
| Key Sx | Fever, headache; Encephalitis (AMS, seizures); ARDS. Mortality 40-75%. | Fever, cough, fatigue, anosmia; Pneumonia, ARDS. | Rash, arthralgia, conjunctivitis; Guillain-Barré; Congenital microcephaly. |
| Dx | RT-PCR (CSF, urine, throat); IgM/IgG ELISA. | RT-PCR (nasopharyngeal); Rapid antigen; HRCT Chest. | RT-PCR (serum, urine); IgM ELISA (cross-reacts). |
| Prevention | Avoid contaminated sap, sick animals; PPE; Ribavirin (limited). | Vaccination; Masks, hygiene, distancing; Ventilation. | Mosquito control; Safe sex; Travel advisory (pregnant). |
⭐ Zika virus infection during pregnancy is a key cause of congenital microcephaly and is also linked to Guillain-Barré syndrome.
Other Pathogens - Beyond the Viruses
- Key non-viral threats: MDR-TB & Rickettsial diseases (e.g., Scrub Typhus).
| Feature | MDR-TB | Scrub Typhus (Tsutsugamushi Fever) |
|---|---|---|
| Agent | M. tuberculosis (INH & RIF resistant) | Orientia tsutsugamushi (Rickettsia) |
| Transmission | Airborne droplets | Chigger mite bite (larvae) |
| Key Sx | Chronic cough, fever, weight loss, night sweats, hemoptysis | Acute fever, headache, myalgia, rash; Eschar (pathognomonic) |
| Dx | Sputum culture (DST), NAAT (GeneXpert) | Serology (IgM ELISA), Weil-Felix (OX-K +ve), PCR |
| Key Rx | Regimen ≥4 effective 2nd-line drugs (Bedaquiline) | Doxycycline; Azithromycin (child/preg) |
⭐ MDR-TB: resistance to at least Isoniazid & Rifampicin (most potent first-line TB drugs).
Public Health Response - Track & Triumph
- Aim: Rapid detection, assessment, and response to emerging threats.
- Core Actions:
- Surveillance: Ongoing data collection (Passive, Active, Sentinel, Syndromic). IDSP is India's cornerstone.
- Outbreak Investigation: Systematic steps to identify source & spread.
- Control Measures: Isolation, quarantine, prophylaxis, vaccination, vector control.
- Risk Communication: Clear, timely updates to public & stakeholders.
- Standard Outbreak Response Flow:
⭐ IDSP (Integrated Disease Surveillance Programme) utilizes S (Syndromic), P (Presumptive), and L (Lab-confirmed) forms for weekly reporting from health facilities across India.
High‑Yield Points - ⚡ Biggest Takeaways
- Nipah virus: Reservoir fruit bats (Pteropus); causes severe encephalitis; high mortality.
- Kyasanur Forest Disease (KFD): Tick-borne (Haemaphysalis spinigera); hemorrhagic fever; Karnataka focus.
- Zika virus: Aedes mosquito transmission; associated with microcephaly and Guillain-Barré syndrome.
- Chandipura virus: Rhabdovirus causing acute encephalitis in Indian children.
- Avian Influenza (H5N1, H7N9): Primarily in birds; human infection via direct contact; high fatality.
- COVID-19: SARS-CoV-2; respiratory pandemic with multi-organ involvement.
- Antimicrobial Resistance (AMR): Critically impacts management of emerging and re-emerging infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

