Gram-Positive Cocci - Staph & Strep Showdown

- Staphylococcus (Catalase +ve):
- S. aureus (Coagulase +ve): Protein A. Skin/soft tissue infections (SSTI), TSS, osteomyelitis, food poisoning. MRSA.
⭐ S. aureus Protein A binds IgG Fc, evading phagocytosis.
- CoNS (Coagulase -ve): S. epidermidis (biofilms, device infections); S. saprophyticus (UTIs).
- S. aureus (Coagulase +ve): Protein A. Skin/soft tissue infections (SSTI), TSS, osteomyelitis, food poisoning. MRSA.
- Streptococcus (Catalase -ve):
- S. pneumoniae (α-hemolytic): Optochin-S. Pneumonia, meningitis.
- S. pyogenes (GAS, β-hemolytic): Bacitracin-S. Pharyngitis, Rheumatic Fever (RF), Post-Streptococcal Glomerulonephritis (PSGN).
- S. agalactiae (GBS, β-hemolytic): CAMP test +ve. Neonatal sepsis.
- Viridans Streptococci (α-hemolytic): S. mutans (caries), endocarditis.
- Enterococcus (γ-hemolytic or α/β): Grows in 6.5% NaCl. UTIs, endocarditis.
- S. gallolyticus (S. bovis group, γ-hemolytic or non-hemolytic): Association with colon cancer. 📌 Mnemonic (S. aureus diseases): STAPH (Skin, TSS, Abscess, Pneumonia, Heart/endocarditis).
Gram-Positive Rods - Toxin & Spore Terrors
- Spore-Formers:
- Bacillus anthracis: Anthrax (black eschar, pulmonary edema). Toxin (PA, EF, LF).
- Bacillus cereus: Food poisoning (emetic - rice; diarrheal).
- Clostridium tetani: Tetanus (spastic paralysis, "lockjaw"). Tetanospasmin (inhibits GABA/glycine).
- Clostridium botulinum: Botulism (flaccid paralysis). Botulinum toxin (blocks ACh).
⭐ Infant botulism: honey ingestion (spores).
- Clostridium perfringens: Gas gangrene (α-toxin, crepitus), food poisoning.
- Clostridioides difficile: Pseudomembranous colitis. Toxins A (enterotoxin) & B (cytotoxin).
- Non-Spore Formers:
- Corynebacterium diphtheriae: Diphtheria (pseudomembrane, myocarditis). Diphtheria toxin (inhibits EF-2).
- Listeria monocytogenes: Listeriosis (meningitis - neonates, IC). Tumbling motility, actin rockets. oka
Gram-Negative Germs - LPS & Endotoxin Empires
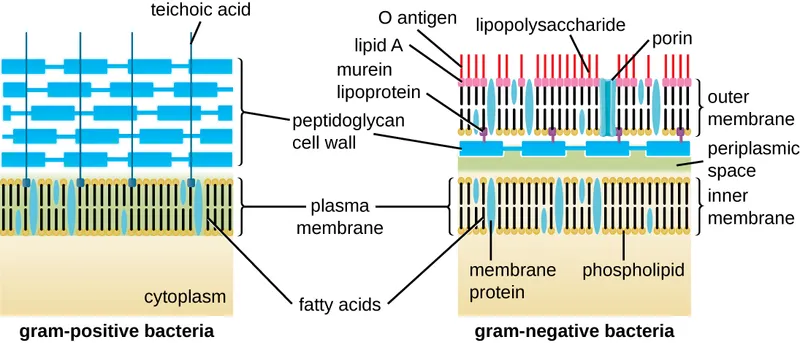
- Outer membrane: Key feature, contains Lipopolysaccharide (LPS).
- LPS: O-antigen (serotype), Core, Lipid A (Endotoxin).
- 📌 Mnemonic: LPS - Lipid A, Polysaccharide (Core), Somatic O-antigen.
- Endotoxin (Lipid A): Released on bacterial lysis. Binds TLR4 on macrophages.
- Induces: TNF-α, IL-1, IL-6 → fever, hypotension, Disseminated Intravascular Coagulation (DIC).
- Can lead to septic shock.
- Common culprits: E. coli, Pseudomonas, Klebsiella, Salmonella, Neisseria.
⭐ Lipid A is the principal endotoxic component of LPS, responsible for its pyrogenic and shock-inducing properties.
Atypical Agents - Acid-Fast & Spiral Spies
- Acid-Fast Bacilli (AFB): Resist acid decolorization (e.g., Ziehl-Neelsen stain: red bacilli).
- Mycobacterium tuberculosis: Aerobe. Culture: Lowenstein-Jensen (LJ) media. Ghon complex (lung lesion + hilar node). Rx: RIPE (📌 Rifampicin, Isoniazid, Pyrazinamide, Ethambutol).
- Mycobacterium leprae (Hansen's Disease): Non-culturable in vitro.
- Tuberculoid: Paucibacillary, strong Cell-Mediated Immunity (↑CMI), +ve lepromin test.
- Lepromatous: Multibacillary, weak CMI (↓CMI), -ve lepromin test, foam cells (lepra cells).
- Nocardia: Weakly acid-fast, Gram-positive branching filaments. Pulmonary, cutaneous, CNS infections.
- Spirochetes: Slender, spiral-shaped, motile. Visualized by dark-field microscopy or silver stains.
- Treponema pallidum (Syphilis): 1° chancre (painless); 2° rash (palms/soles), condyloma lata; 3° gummas, neurosyphilis, aortitis. Dx: VDRL/RPR (screen), FTA-ABS/TP-PA (confirm).
- Borrelia burgdorferi (Lyme Disease): Vector: Ixodes ticks. Erythema migrans (bull's-eye rash), Bell's palsy, arthritis, carditis.
- Leptospira interrogans (Leptospirosis): From animal urine. Weil's disease (severe: icterus, azotemia, hemorrhage, anemia).

⭐ Lepromatous leprosy features numerous acid-fast bacilli within foam cells (Virchow cells), a negative lepromin skin test, high antibody titers, and anergy to M. leprae antigens.
High‑Yield Points - ⚡ Biggest Takeaways
- Gram stain is key: Staphylococcus (G+ve cocci, clusters), Streptococcus (chains), E.coli (G-ve rod).
- Mycobacterium tuberculosis: Acid-fast bacillus (Ziehl-Neelsen stain), requires Lowenstein-Jensen medium.
- Exotoxins (secreted, protein, specific effects) vs. Endotoxin (LPS of G-ve bacteria, causes septic shock).
- MRSA (mecA gene) and ESBL-producing organisms are major antibiotic resistance threats.
- Atypical bacteria: Mycoplasma (no cell wall), Chlamydia (obligate intracellular parasites).
- Pseudomonas aeruginosa: Oxidase-positive G-ve rod, common in burns, CF, and ventilator-associated pneumonia (VAP).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

