Tumor Antigens - Cancer's ID Tags
- Molecules on tumor cells recognized by the immune system (T cells, antibodies).
- Key to immunotherapy & diagnostics.
Types of Tumor Antigens:
- Tumor-Specific Antigens (TSAs):
- Exclusively on tumor cells.
- Arise from mutations (e.g., mutated p53, RAS) or viral oncogenes (e.g., HPV E6/E7).
- Ideal targets for therapy.
- Tumor-Associated Antigens (TAAs):
- Also on normal cells, but overexpressed or aberrantly expressed on tumors.
- Examples:
- Oncofetal antigens: AFP (liver cancer), CEA (colon cancer).
- Differentiation antigens: PSA (prostate cancer), MART-1 (melanoma).
- Overexpressed self-proteins: HER2/neu (breast cancer).

⭐ CEA (Carcinoembryonic Antigen) is a classic TAA used primarily for monitoring colorectal cancer recurrence, not for initial diagnosis due to low specificity/sensitivity.
📌 Mnemonic: Tumor Specific = Solely on Tumors; Tumor Associated = Also on normal, but Abnormal on Tumors.
Immune Surveillance - Body's Cancer Cops
- Natural defense: Recognizes & eliminates nascent transformed cells.
- Mediated by both innate & adaptive immunity.
- Key Effector Cells:
- Innate:
- Natural Killer (NK) cells: Target cells with ↓MHC-I or stress ligands (e.g., MICA/B). Release perforin, granzymes.
- M1 Macrophages: Phagocytosis, release TNF-α, NO.
- Adaptive:
- Cytotoxic T Lymphocytes (CTLs/CD8+ T cells): Recognize tumor antigens on MHC-I. Induce apoptosis (perforin/granzymes, Fas-FasL).
- Helper T cells (Th1/CD4+ T cells): Secrete IFN-γ (activates CTLs, Mφ), TNF-α.
- Innate:
⭐ IFN-γ, produced mainly by Th1 cells and NK cells, is pivotal for anti-tumor immunity by activating macrophages and enhancing CTL differentiation and killing.
- Evidence: ↑cancer incidence in immunosuppressed individuals (e.g., AIDS, transplant recipients).
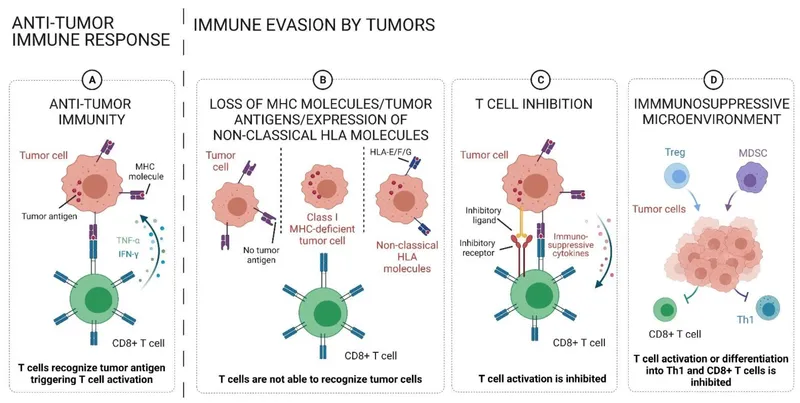
Tumor Evasion - Cancer's Escape Artistry
- ↓ MHC-I Expression:
- Tumor cells evade CTL recognition.
- Mutations in TAP, β2-microglobulin.
- Antigen Masking/Shedding:
- Glycocalyx (sialomucins) hides antigens.
- Shed antigens neutralize antibodies.
- Immunosuppressive Microenvironment:
- Secretion: TGF-β, IL-10.
- Recruitment: Tregs, MDSCs.
- Checkpoint Ligands:
- PD-L1 (tumor) binds PD-1 (T-cell) → T-cell exhaustion.
- CTLA-4 (T-cell) binds B7 ligands (tumor/APCs) → ↓ T-cell activation.
- Induce T-cell Apoptosis:
- Tumor FasL binds Fas on T-cells → apoptosis.
- Lack of Co-stimulation:
- Absent B7 (CD80/CD86) on tumor cells → T-cell anergy.
- Antigenic Variation:
- Immune selection of antigen-negative variants.
- Immune selection of antigen-negative variants.
⭐ PD-L1 expression on tumor cells binds PD-1 on T-cells, causing T-cell exhaustion. This is a key immune escape targeted by checkpoint inhibitors (e.g., Pembrolizumab).
Cancer Immunotherapy - Boosting The Defense
- Principle: Augmenting patient's immune system to target and destroy cancer cells.
- Key Strategies:
- Immune Checkpoint Inhibitors (ICIs):
- Block T-cell inhibitory signals (PD-1/PD-L1, CTLA-4).
- E.g., Pembrolizumab (anti-PD-1), Ipilimumab (anti-CTLA-4).
- Unleashes T-cell anti-tumor response.
- Adoptive Cell Therapy (ACT):
- CAR T-cells: T-cells engineered with Chimeric Antigen Receptors (e.g., anti-CD19 for B-cell malignancies).
- TILs: Ex vivo expanded Tumor-Infiltrating Lymphocytes.
- Cancer Vaccines: E.g., Sipuleucel-T (prostate cancer).
- Oncolytic Viruses: E.g., T-VEC (melanoma).
- Cytokines: Non-specific immunostimulants (IL-2, IFN-α).
- Immune Checkpoint Inhibitors (ICIs):
⭐ Immune Checkpoint Inhibitors (ICIs) targeting PD-1/PD-L1 (e.g., Pembrolizumab) have revolutionized treatment for melanoma, NSCLC, and renal cell carcinoma.

High‑Yield Points - ⚡ Biggest Takeaways
- Tumor Antigens: Include Tumor-Specific Antigens (TSAs) and Tumor-Associated Antigens (TAAs).
- Immune Surveillance: Primarily mediated by Cytotoxic T Lymphocytes (CTLs) and NK cells.
- Tumor Evasion Strategies: Include ↓MHC-I expression, PD-L1 upregulation, and immunosuppressive cytokines.
- Immune Checkpoint Blockade: Anti-PD-1/PD-L1 and Anti-CTLA-4 therapies reinvigorate T-cell responses.
- Adoptive Cell Therapy: CAR T-cells are engineered to recognize and kill cancer cells.
- Chronic Inflammation: Can promote tumorigenesis by creating a favorable microenvironment_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

