Overview & Classification - Immune System Gaps
- Immunodeficiency: Immune system failure/dysfunction leading to ↑ susceptibility to infections & diseases.
- Types:
- Primary (PID): Intrinsic, often genetic, defects in immune cells/proteins.
- B-cell (antibody) defects (e.g., XLA)
- T-cell (cellular) defects (e.g., DiGeorge)
- Combined B & T cell (e.g., SCID)
- Phagocytic cell defects (e.g., CGD)
- Complement system defects
- Secondary (SID): Acquired; more common (e.g., HIV, malnutrition, immunosuppressive drugs).
- Primary (PID): Intrinsic, often genetic, defects in immune cells/proteins.
- Warning Signs (📌 SPURR):
- Severe infections
- Persistent infections
- Unusual organisms/sites
- Recurrent infections
- Runting (Failure to Thrive) / Family Hx
⭐ The majority of Primary Immunodeficiencies are X-linked, leading to a higher prevalence in males. SCID is a pediatric emergency!
B-Cell Deficiencies - Antibody Alarms
- XLA (Bruton's): 📌 Boys, Bruton, BTK gene, B-cells absent/↓, recurrent Bacterial infections.
- XLR; Onset: 6-12 mo.
- Labs: ↓ All Ig, absent/↓ B-cells (CD19+).
- Infections: Encapsulated bacteria, enteroviruses.
- CVID: Onset: Bimodal (20-40 yrs).
- Labs: ↓ IgG, ↓ IgA/IgM; B-cells N/↓, poor Ab response.
- Infections: Sinopulmonary, autoimmune, ↑ lymphoma risk.
- Selective IgA Deficiency: Most common PID. Often asymptomatic.
- Labs: ↓ IgA, N IgG/IgM.
- Infections: Sinopulmonary, GI; anaphylaxis to IgA-products.
- Hyper-IgM (X-linked): CD40L defect.
- Labs: ↑/N IgM, ↓↓ IgG, IgA, IgE. N B-cells.
- Infections: P. jirovecii, encapsulated bacteria, opportunistic.
⭐ CVID patients have an increased risk of developing autoimmune diseases and lymphoma.
T-Cell & Combined Deficiencies - Cellular Chaos Crew
- DiGeorge Syndrome (22q11.2 del)
- 📌 CATCH-22: Cardiac defects, Abnormal facies, Thymic hypoplasia, Cleft palate, Hypocalcemia.
- Labs: ↓ T-cells, variable Ig.
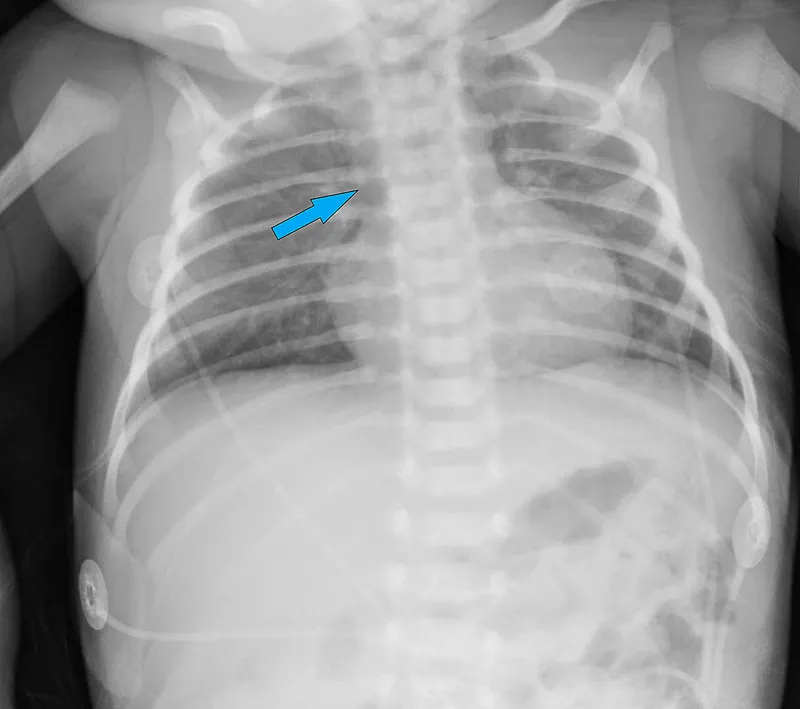
- Severe Combined Immunodeficiency (SCID)
- Genes: IL2RG (X-linked), ADA, RAG.
- Features: Severe recurrent infections (viral, fungal, bacterial), Failure To Thrive (FTT).
- Labs: Markedly ↓ T-cells (<20% lymphocytes), B-cells variable/non-functional, ↓ Ig.
⭐ SCID: Infancy onset, persistent infections, FTT. Absent thymic shadow on CXR is key.
- Wiskott-Aldrich Syndrome (WAS, X-linked)
- Triad: Eczema, Thrombocytopenia (small platelets), Recurrent infections.
- Labs: ↓ T-cells, ↓ IgM, ↑ IgA, ↑ IgE.
- Ataxia-Telangiectasia (ATM, AR)
- Triad: Cerebellar Ataxia, Oculocutaneous Telangiectasias, Immunodeficiency (recurrent sinopulmonary infections).
- Labs: ↓ T-cells, ↓ IgA/IgE/IgG2. ↑ AFP (Alpha-fetoprotein).
Phagocyte & Complement Defects - Defense Downfalls
- Phagocytic Defects:
- Chronic Granulomatous Disease (CGD): NADPH oxidase defect; NBT test ➖. Recurrent infections with catalase ➕ organisms. 📌 CGD: Susceptibility to Catalase-positive organisms (e.g., S. aureus, Aspergillus).
- Leukocyte Adhesion Deficiency (LAD): CD18 defect. Delayed umbilical cord separation (>30 days), recurrent bacterial infections.
- Chediak-Higashi Syndrome: LYST gene defect. Giant granules in phagocytes, partial albinism, recurrent pyogenic infections.
- Complement Deficiencies:
- C1/C2/C4: Associated with SLE-like syndrome.
- C3: Results in severe pyogenic infections.
- C5-C9 (MAC): Leads to recurrent Neisseria infections.
- C1 Inhibitor Deficiency: Causes Hereditary Angioedema (HAE).
⭐ Nitroblue Tetrazolium (NBT) test is negative in CGD, indicating defective phagocytic oxidative burst.
oka
Secondary IDs & Approach - Acquired Achilles' Heels
- Causes: HIV/AIDS, malnutrition, drugs (immunosuppressants, chemo), malignancy, splenectomy.
- Diagnosis:
- Initial: History, Physical Exam.
- Screening: CBC with diff, Ig levels, CH50.
- Confirmatory: Flow cytometry, NBT test, genetic tests.
- Management: Prophylaxis, IVIG, HSCT, Gene Rx.
⭐ A CBC with differential is a crucial initial screening test for suspected immunodeficiency.
High‑Yield Points - ⚡ Biggest Takeaways
- Bruton's (XLA): BTK defect, no B-cells/Igs, recurrent bacterial infections after 6 months.
- DiGeorge Syndrome: 22q11.2 deletion, T-cell deficiency, hypocalcemia, cardiac defects.
- SCID: Severe T-cell defect (e.g., IL-2Rγ, ADA), early severe infections, requires HSCT.
- Wiskott-Aldrich: X-linked WASp, Thrombocytopenia, Eczema, Recurrent infections.
- CGD: NADPH oxidase defect, recurrent catalase (+) infections, abnormal DHR/NBT test.
- Selective IgA Deficiency: Most common, often asymptomatic, risk of anaphylaxis to IgA.
- CVID: Adult onset, low Igs, recurrent infections, risk of autoimmunity, lymphoma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

